Swimming: Enhancing Mobility Naturally for Spinal & Back Health
Uncover the impact of swimming on spinal and back health. Find tips on how to incorporate this activity into your routine.
Unlocking Optimal Spinal Health: The Powerful Synergy of Chiropractic Care and Swimming for Back Pain Relief and Musculoskeletal Wellness
Living with chronic back pain can transform everyday activities into daunting challenges, affecting your quality of life, productivity, and overall well-being. Whether you’re dealing with acute discomfort following an injury or managing persistent spinal issues that have plagued you for years, finding effective, non-invasive treatment solutions remains paramount. Two powerful therapeutic approaches have emerged as cornerstones of comprehensive spinal health management: chiropractic care and aquatic exercise, particularly swimming. When combined, these complementary modalities create a synergistic healing protocol that addresses both the structural alignment of the spine and the functional strength of the musculoskeletal system (Jimenez, n.d.-a; Peng et al., 2022).
At Injury Medical Chiropractic and Functional Medicine Clinic in El Paso, Texas, Dr. Alexander Jimenez, DC, APRN, FNP-BC, CFMP, IFMCP—a uniquely qualified board-certified Family Practice Nurse Practitioner and Doctor of Chiropractic—has pioneered an integrative approach to spinal health that leverages the most current evidence-based protocols. His dual-scope practice combines advanced clinical expertise with functional medicine principles to deliver personalized, patient-centered care that addresses the root causes of back pain rather than merely masking symptoms (Jimenez, n.d.-a).
This comprehensive guide explores the transformative benefits of integrating chiropractic adjustments with swimming exercises for optimal spinal and back health, drawing from Dr. Jimenez’s clinical insights and the latest peer-reviewed research. We’ll examine how these complementary approaches work together to relieve pain, restore function, strengthen supporting musculature, and prevent future injuries.
Understanding the Musculoskeletal System and Spinal Anatomy
Before delving into treatment approaches, it’s essential to understand the remarkable complexity of the musculoskeletal system and the critical role your spine plays in overall health and function. The musculoskeletal system comprises two integrated components: the muscular system, which includes all muscles, tendons, and connective tissues; and the skeletal system, encompassing bones, joints, cartilage, and ligaments (Kenhub, 2023). Together, these systems provide the body with movement, stability, shape, and support while protecting vital organs and enabling daily activities.
The Spinal Column: Architecture of Support
Your spine is one of the most intricate structures in the human body, consisting of 33 individual bones called vertebrae, which are stacked atop one another to form the spinal column (National Spine Health Foundation, 2024). This remarkable architecture is divided into five distinct regions, each serving specialized functions:
Cervical Spine (C1-C7): The seven vertebrae in your neck support the head’s weight—approximately 10 to 12 pounds—while allowing an extensive range of motion for rotation, flexion, and extension (Texas Spine & Sports Therapy Center, 2025). The first two cervical vertebrae, the atlas (C1) and axis (C2), enable the head’s nodding and rotational movements.
Thoracic Spine (T1-T12): These twelve mid-back vertebrae attach to the rib cage, providing stability and protection for vital organs, including the heart and lungs (American Association of Neurological Surgeons, 2024). The thoracic region demonstrates less mobility than other spinal segments due to these structural attachments.
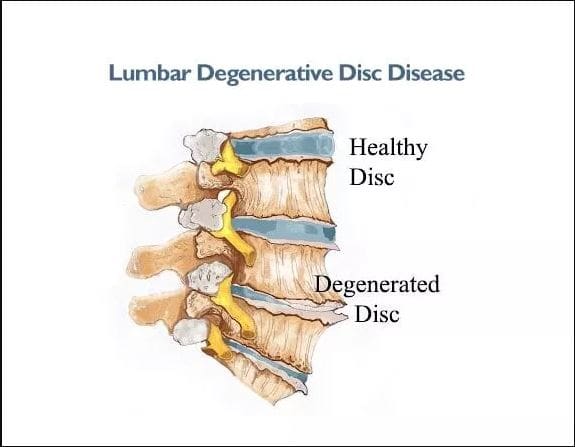
Lumbar Spine (L1-L5): The five lumbar vertebrae in your lower back are the largest and strongest, designed to support most of the body’s weight and withstand significant mechanical stress (National Spine Health Foundation, 2024). This region experiences the highest incidence of degenerative changes and injury due to constant loading forces.
Sacrum (S1-S5): Five fused vertebrae form this triangular bone that connects the spine to the pelvis, serving as the foundation for numerous muscle and ligament attachments (National Spine Health Foundation, 2024).
Coccyx: Four to five fused vertebrae comprise the tailbone, which provides attachment points for pelvic floor muscles and ligaments.
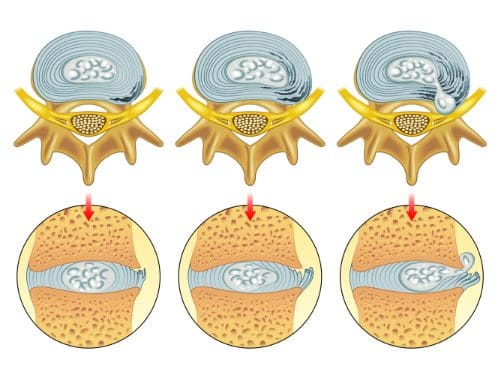
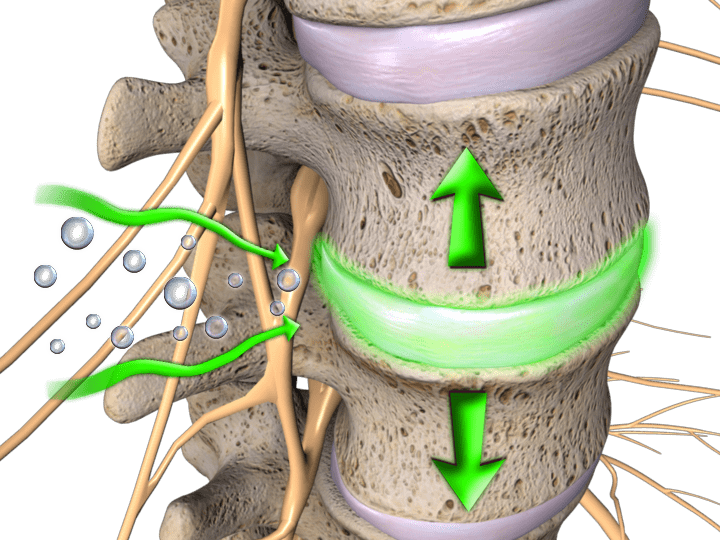
Intervertebral Discs: Nature’s Shock Absorbers
Between each vertebra (except the first two cervical vertebrae) lie specialized structures called intervertebral discs, which serve three primary functions: shock absorption, structural support, and facilitation of slight spinal mobility (Spine-health, 2017). These discs consist of two distinct components:
Annulus Fibrosus: The tough outer ring is composed of concentric sheets of collagen fibers that hydraulically seal the inner core and distribute forces evenly across the structure.
Nucleus Pulposus: The gel-like inner core containing a loose network of fibers suspended in a mucoprotein gel, which at birth consists of approximately 80% water (Spine-health, 2017). Proper hydration remains essential for optimal disc function, as the nucleus pulposus serves as the major carrier of the body’s axial load.
The Spinal Cord and Nerve Function
Protected within the vertebral column runs the spinal cord—a long, tubular bundle of neural tissue extending from the brainstem down through the vertebral canal (National Spine Health Foundation, 2024). This critical structure serves as the central communication pathway, transmitting sensory and motor signals between the brain and the body. At each vertebral level, spinal nerves exit through small openings called intervertebral foramina, branching out to innervate specific body regions and enabling the nervous system’s remarkable coordination of movement, sensation, and organ function.
The Foundation of Healing: Chiropractic Care for Spinal Health
Chiropractic care has evolved into a respected, evidence-based healthcare discipline focused on diagnosing, treating, and preventing mechanical disorders of the musculoskeletal system, particularly those involving the spine (Sleigh Family Chiropractic, 2024). The foundational principle underlying chiropractic philosophy holds that proper alignment of the body’s musculoskeletal structure—especially the spine—enables the body to heal itself without surgery or medication, emphasizing the body’s inherent recuperative powers (Tigard Chiropractic Auto Injury, 2024).
Dr. Alexander Jimenez’s Integrative Chiropractic Approach
Dr. Jimenez’s unique dual certification as both a Doctor of Chiropractic and a board-certified Family Practice Nurse Practitioner (FNP-BC) positions him to deliver truly comprehensive, integrative care that bridges traditional and alternative medicine (Jimenez, n.d.-a; Academy of Anti-Aging Medicine, 2016). His holistic evaluation process considers not only physical symptoms but also nutritional factors, lifestyle behaviors, environmental exposures, psychological elements, and genetic predispositions that may contribute to chronic pain conditions.
At the Injury Medical Chiropractic and Functional Medicine Clinic, Dr. Jimenez employs advanced diagnostic evaluations to clinically associate patient injuries with underlying pathology. His assessment protocols include:
Comprehensive History Taking: Thorough documentation of the patient’s chief complaints, history of present illness (using the OPQRST mnemonic: Onset, Provocation/Palliation, Quality, Region/Radiation, Severity, and Time), past medical history, family history, psychosocial factors, and detailed review of systems (KMC University, 2024). This meticulous history-gathering process drives the subsequent physical examination and establishes medical necessity for treatment.
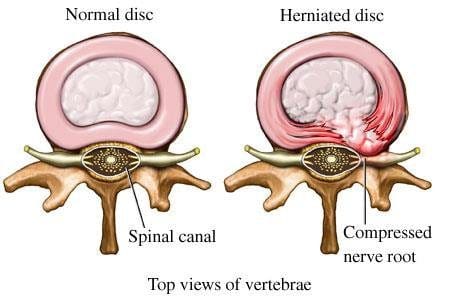
Advanced Imaging and Diagnostic Testing: When clinically indicated, Dr. Jimenez utilizes state-of-the-art imaging technologies, including Magnetic Resonance Imaging (MRI), Computed Tomography (CT) scans, and fluoroscopy, to visualize soft tissues, bones, nerves, and spinal structures with exceptional detail (Spine Diagnostic, 2025). MRI proves particularly valuable for identifying herniated discs, spinal cord compression, nerve root irritation, and soft tissue pathology, while CT scans excel at evaluating bony structures, fractures, spinal stenosis, and arthritic changes (Great Lakes Medical Imaging, 2025). Fluoroscopy provides real-time imaging guidance during interventional procedures, ensuring precise needle placement for therapeutic injections.
Functional Medicine Assessments: As an Institute for Functional Medicine Certified Practitioner (IFMCP), Dr. Jimenez conducts detailed health assessments using the Living Matrix Functional Medicine platform, evaluating genetics, current nutrition, activity patterns, toxic environmental exposures, and emotional factors that may contribute to chronic disorders (Jimenez, n.d.-a). This root-cause analysis enables truly personalized treatment plans that address underlying imbalances rather than simply suppressing symptoms.
Physical Examination and Orthopedic Testing: Comprehensive musculoskeletal examination including postural analysis, range of motion assessment, orthopedic provocative tests, neurological evaluation, and palpation to identify areas of restriction, tenderness, or dysfunction (International Chiropractors Association, n.d.).
Movement Medicine: Chiropractic Care- Video
The Science Behind Chiropractic Adjustments
Spinal manipulation—also called chiropractic adjustment—represents the cornerstone technique in chiropractic care, focusing on improving spinal motion and overall physical function (Recovery Chiro Med, 2024). Research demonstrates that chiropractic adjustments significantly reduce acute low back pain and improve physical function, offering an effective alternative to invasive procedures and pharmaceutical interventions (SCUHS, 2025; Duke Health, 2025).
The American College of Physicians recommends non-medication treatments such as spinal manipulation, exercise, and yoga for chronic low back pain before considering medications (SCUHS, 2025). A landmark 2017 study published in the Journal of the American Medical Association found that spinal manipulation was associated with moderate improvements in short-term back pain and function compared to placebo treatment for up to six weeks (SCUHS, 2025).
Key Benefits of Chiropractic Care for Back Pain
Natural Pain Relief: By correcting spinal misalignments (subluxations) and restoring proper joint function, chiropractic adjustments alleviate pressure on nerves and reduce inflammation, providing both immediate relief and long-term pain management without relying on medications (Medical Wellness Group, 2023; Doc Moss, 2024). The adjustments help release endorphins—the body’s natural pain-relieving chemicals—which contribute to pain reduction and promote relaxation.
Improved Spinal Alignment: Full-body chiropractic adjustments restore proper alignment of the vertebrae, reducing abnormal stress on joints, discs, muscles, and ligaments (Cityview Chiropractor, 2025). This realignment process minimizes bone friction, potentially slowing the progression of degenerative conditions like arthritis, and creates optimal biomechanical function throughout the kinetic chain.
Enhanced Range of Motion and Flexibility: By addressing joint restrictions and muscle tension, chiropractic care improves mobility and flexibility, enabling patients to move more freely and comfortably in daily activities (Recovery Chiro Med, 2024). Increased range of motion contributes to better athletic performance, reduced risk of injury, and improved quality of life.
Reduced Muscle Tension and Spasm: Spinal adjustments help normalize muscle tone by addressing the neurological factors that contribute to muscle hypertonicity and spasm (SCUHS, 2025). When vertebrae are properly aligned, the nervous system functions more efficiently, reducing abnormal muscle guarding and allowing tissues to relax.
Better Posture: Regular chiropractic care helps correct postural imbalances that develop from prolonged sitting, repetitive movements, or previous injuries (Sleigh Family Chiropractic, 2024). Improved posture reduces strain on the spine and supporting structures, preventing the development or progression of chronic pain conditions.
Improved Nerve Function: Chiropractic adjustments optimize nervous system function by removing interference caused by spinal misalignments (SCUHS, 2025). When the spine is properly aligned, nerve signals can flow freely between the brain and body, supporting optimal organ function, immune response, and overall health.
Holistic Wellness: Chiropractic care takes a whole-body approach to health, considering the interconnectedness of physical, nutritional, and lifestyle factors (Medical Wellness Group, 2023). Chiropractors provide guidance on ergonomics, exercise, nutrition, and stress management to support optimal spinal health and prevent future problems.
Preventive Care: Regular chiropractic adjustments help maintain proper alignment, strengthen supporting muscles, and reduce the risk of re-injury (Medical Wellness Group, 2023). This proactive approach enables patients to maintain their health rather than waiting for problems to develop.
Non-Invasive and Drug-Free: Chiropractic care offers a conservative treatment option that avoids the potential risks and side effects associated with medications or surgical interventions (Medical Wellness Group, 2023). This approach aligns with patients’ increasing preference for natural, holistic healthcare solutions.
Common Chiropractic Techniques
Dr. Jimenez and chiropractic professionals employ various adjustment techniques tailored to each patient’s specific needs, condition severity, and comfort level:
Manual Adjustments: The chiropractor uses their hands to apply controlled force to specific joints, correcting misalignments and restoring proper function (Recovery Chiro Med, 2024). These hands-on adjustments represent the classic chiropractic technique and remain highly effective for most patients.
Instrument-Assisted Adjustments: Special tools like activators deliver precise, gentle manipulation to targeted areas, providing an alternative for patients who prefer less forceful techniques (Recovery Chiro Med, 2024). These instruments allow for controlled force application with minimal discomfort.
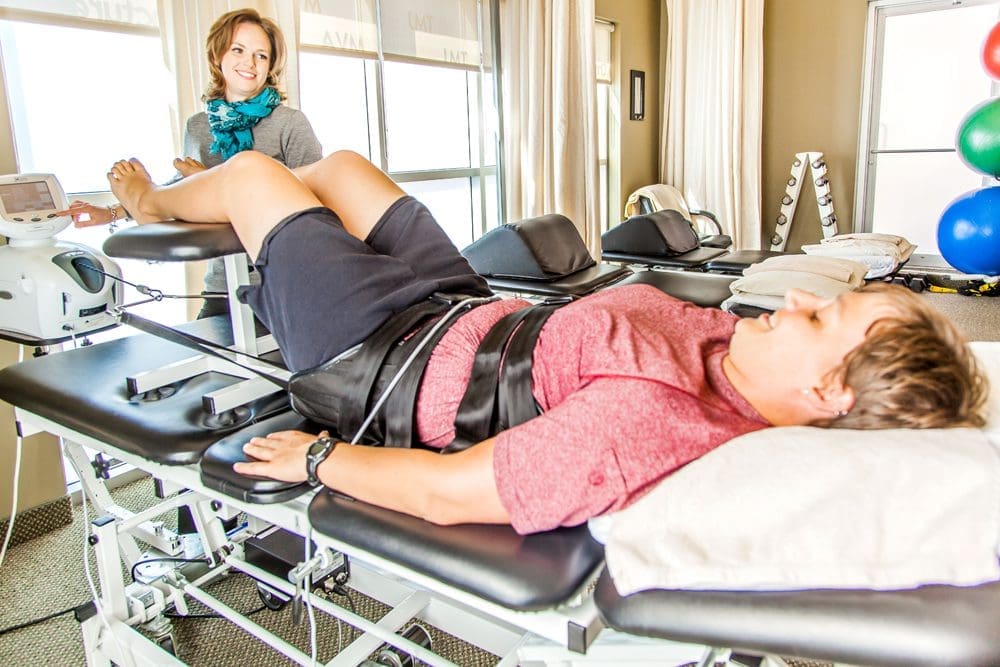
Flexion-Distraction: This technique utilizes a specialized table that gently stretches the spine using a pumping action, creating negative pressure within the discs to promote healing of bulges and herniations (Recovery Chiro Med, 2024). The method proves particularly beneficial for patients with acute disc problems or those who cannot tolerate more forceful adjustments.
Soft Tissue Therapy: Chiropractors often incorporate massage, myofascial release, trigger point therapy, and other soft tissue techniques to relax tight muscles, improve circulation, and reduce pain and inflammation (Medical Wellness Group, 2023). These complementary therapies enhance the effectiveness of spinal adjustments and promote tissue healing.
Therapeutic Exercises: Prescribed exercises strengthen core muscles, improve posture, enhance flexibility, and stabilize the spine (Medical Wellness Group, 2023). These exercises form a critical component of rehabilitation and help prevent future episodes of back pain.
The Transformative Power of Swimming for Spinal and Back Health
Swimming and aquatic exercise represent ideal complementary therapies to chiropractic care, offering unique advantages for individuals dealing with back pain and spinal conditions. The aquatic environment provides properties that cannot be replicated on land, making water-based exercise exceptionally beneficial for musculoskeletal rehabilitation and maintenance (Jimenez, n.d.-b).
Why Swimming Excels for Back Pain Management
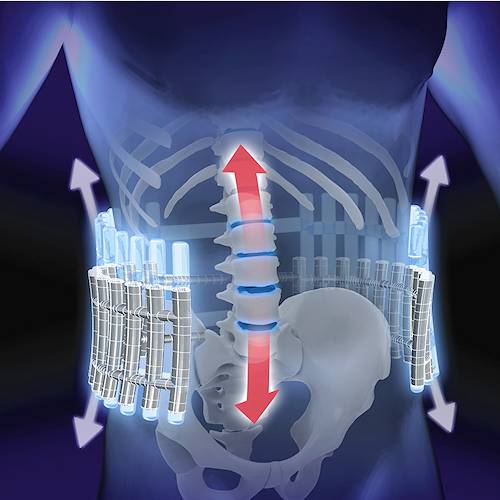
Buoyancy Reduces Spinal Compression: Water’s buoyancy supports up to 90% of body weight, substantially reducing compressive forces on the spine and weight-bearing joints (Physio Inq, 2022; Spine. MD, 2022). This dramatic reduction in gravitational loading allows individuals with back pain to move freely and exercise comfortably without aggravating their condition. Research indicates that performing rehabilitation exercises in water can reduce spinal compression by more than half, depending on water depth (Sutton Place PT, 2024).
Low-Impact Aerobic Conditioning: Unlike running, jumping, or other high-impact land exercises that jar the spine and joints, swimming provides cardiovascular conditioning without impact stress (Jimenez, n.d.-b). The water suspends the body, eliminating the shock forces that occur with each footstrike during land-based activities. This characteristic makes swimming accessible to individuals who cannot tolerate traditional exercise due to pain or injury.
Natural Resistance Strengthens Muscles: Water is 600-700 times more resistant than air, providing natural resistance in all directions that helps strengthen muscles without requiring heavy weights (Helen Hayes Hospital, 2021). This uniform resistance engages muscles throughout their full range of motion, building functional strength that supports the spine and improves overall stability. Swimming works muscles not always activated during land activities, particularly those essential for spinal stability (Jimenez, n.d.-b).
Warm Water Promotes Relaxation and Healing: Therapeutic pools typically maintain water temperatures between 90-94°F, creating a thermoneutral environment that minimizes heat loss or gain when the body is immersed (AzOPT, 2024). Warm water relaxes tense muscles, decreases spasticity, increases blood flow to injured tissues, promotes flexibility, and triggers endorphin release (Helen Hayes Hospital, 2021; Versus Arthritis, n.d.). The warmth helps reduce pain perception and creates a comfortable environment for therapeutic exercise.
Hydrostatic Pressure Reduces Swelling: The pressure exerted by water against the body helps reduce edema and swelling, improves circulation, and enhances the delivery of oxygen and nutrients to healing tissues (Helen Hayes Hospital, 2021). This gentle compression effect can be particularly beneficial for individuals with inflammatory conditions or post-surgical swelling.
Improved Flexibility and Range of Motion: The buoyancy of water reduces the effects of gravity, allowing for increased joint range of motion with less pain (Helen Hayes Hospital, 2021). Movements that may be difficult or impossible on land become achievable in water, gradually restoring functional mobility. The warm water also helps relax muscles that are sore or tight, further enhancing flexibility gains.
Psychological Benefits: The meditative rhythm of swimming, combined with the soothing properties of water, often improves mood, reduces stress and anxiety, and enhances adherence to exercise programs compared to gym-based workouts (Physio Inq, 2022). Many patients find water exercise more enjoyable and relaxing than land-based alternatives, leading to better long-term compliance with their rehabilitation program.
Scientific Evidence Supporting Aquatic Exercise for Back Pain
Numerous peer-reviewed studies have demonstrated the effectiveness of aquatic exercise for chronic back pain management. A systematic review and meta-analysis published in the American Journal of Physical Medicine and Rehabilitation analyzed eight randomized controlled trials involving 331 patients with low back pain (Shi et al., 2018). The results showed statistically significant pain relief (standardized mean difference = -0.65) and improved physical function (standardized mean difference = 0.63) following aquatic exercise interventions. The researchers concluded that aquatic exercise can significantly reduce pain and increase physical function in patients with low back pain, though they noted that further high-quality investigations on a larger scale are needed to confirm these results.
A more recent randomized clinical trial published in JAMA Network Open compared therapeutic aquatic exercise to physical therapy modalities for chronic low back pain over a 12-month follow-up period (Peng et al., 2022). The study found that participants in the therapeutic aquatic exercise group gained significantly greater and more clinically meaningful improvement in disability, pain intensity, quality of life, sleep quality, kinesiophobia, and fear avoidance compared to the physical therapy modalities group. The researchers concluded that therapeutic aquatic exercise is an effective and safe treatment for chronic low back pain, with most participants willing to recommend it to other patients with similar conditions.
An additional systematic review examining the effect of aquatic physical therapy on chronic low back pain included 13 randomized controlled trials and found that aquatic physical therapy could reduce pain intensity, improve quality of life, and enhance disability measures in the short term (PMC, 2022). These consistent findings across multiple studies provide robust evidence supporting the integration of swimming and aquatic exercise into comprehensive back pain treatment protocols.
Recommended Swimming Strokes for Back Health
Not all swimming strokes are equally beneficial for individuals with back pain. Dr. Jimenez and spinal health experts recommend specific strokes that minimize spinal stress while providing optimal therapeutic benefits:
Backstroke: This stroke is widely considered the safest option for individuals with back pain because it maintains a horizontal body position that minimizes pressure on the lower back (Penn Spine & Orthopedic, 2024; NuVasive, 2017). Backstroke promotes proper body alignment, reduces spine stress, and effectively strengthens back muscles in a low-impact environment. The repetitive motion enhances spine flexibility and muscle mobility while engaging core muscles to stabilize the spine. However, backstroke does require stronger abdominal muscles, so individuals should gradually build core strength before relying heavily on this stroke (NuVasive, 2017).
Freestyle (Front Crawl): When performed with proper technique and caution, freestyle can help strengthen muscles and improve cardiovascular fitness (Penn Spine & Orthopedic, 2024). The key is to avoid excessive neck extension when turning to breathe, as jerking movements can lead to neck and lower back injuries (NuVasive, 2017). Swimmers should focus on rotating the entire body when breathing rather than lifting the head out of the water. Proper freestyle technique involves keeping the head in line with the body, looking straight at the bottom of the pool, and rotating shoulders and hips together during the stroke cycle (GWRY MCA, 2022).
Breaststroke: This stroke is often recommended as the best option for those with back pain because it builds muscle tone without overdoing stress on the spine (NuVasive, 2017). The breaststroke allows for controlled breathing without excessive neck rotation and maintains a relatively neutral spine position throughout the stroke cycle. However, individuals should be cautious about excessive lumbar hyperextension during the glide phase.
Strokes to Approach with Caution: The butterfly stroke places significant force on the spine due to the undulating body motion and simultaneous arm pull, making it generally unsuitable for individuals with back pain (Precision Pain Care, n.d.). Some individuals may also find that certain strokes irritate their specific condition, underscoring the importance of consulting with healthcare providers like Dr. Jimenez before beginning a swimming program.
Getting Started: Swimming Exercises for Back Relief
Dr. Jimenez recommends several progressive aquatic exercises that individuals with back pain can incorporate into their rehabilitation program (Jimenez, n.d.-b):
Water Walking: Simply walking around the pool provides the movement the body needs to heal and build muscle without aggravating symptoms (Jimenez, n.d.-b; Senior Lifestyle, 2023). Begin at a slow pace in the shallow end, walking back and forth for 5-10 minutes. Press your heels into the pool floor first and avoid walking on your tiptoes. As your strength and confidence improve, you can increase the duration, speed, and water depth. Water walking burns up to 3.5 times more calories than similar activity on land due to the increased resistance (HydroWorx, 2023).
Water Aerobics: Water aerobics classes or individual routines provide excellent cardiovascular conditioning and help increase mobility and flexibility (Jimenez, n.d.-b). These group classes typically involve rhythmic movements set to music, creating a social and enjoyable exercise environment. The variety of movements in water aerobics works multiple muscle groups and can be easily modified to accommodate different fitness levels and limitations.
Swimming Laps: Once cleared by your healthcare provider, start swimming laps slowly—perhaps only twice weekly initially (Jimenez, n.d.-b). Different stroke types work various muscles in the hips, chest, and back, providing comprehensive musculoskeletal conditioning. Begin with short distances and gradually increase as your endurance improves. Treading water serves as an excellent way to acclimate your body to aquatic movements and build water confidence before attempting continuous lap swimming.
Leg Lifts and Knee Raises: Standing in waist-deep water, perform leg lifts by raising one leg at a time to the front, side, and back, which helps strengthen leg muscles and improve hip mobility (Blakehurst LCS, 2025). Knee lifts involve raising the knees toward the chest, which targets lower abdominal muscles and improves balance. These exercises can be performed while holding the pool edge for support or free-standing as balance improves.
Arm Circles and Arm Curls: Standing in shoulder-deep water, perform arm circles by moving arms in circular motions to improve shoulder flexibility and strength (Blakehurst LCS, 2025). For arm curls, use foam water weights that create resistance as you push them through the water, building upper body strength without heavy equipment (Senior Lifestyle, 2023).
Torso Twists: Standing in shoulder-deep water, rotate the upper body from side to side to improve flexibility in the spine and core muscles (Blakehurst LCS, 2025). This exercise helps restore rotational mobility that is often limited in individuals with back pain.
Kickboard Exercises: Lean your upper body on a kickboard and focus on kicking movements, which isolate lower body work and strengthen leg muscles (Jimenez, n.d.-b). This exercise allows individuals to work on their kick technique and build leg strength while the kickboard supports the upper body, eliminating stress on the arms and shoulders.
Optimizing Aquatic Exercise Conditions
The therapeutic effectiveness of aquatic exercise depends partly on environmental factors that patients and therapists can optimize:
Water Temperature: Therapeutic pools should maintain temperatures between 90-94°F to achieve thermoneutral conditions that prevent excessive heat loss or gain (AzOPT, 2024). This temperature range promotes muscle relaxation, reduces spasticity, and enhances flexibility. Individuals with different conditions may benefit from slightly adjusted temperatures—for example, those with multiple sclerosis often prefer cooler water (84°F), while individuals with spasticity from spinal cord injuries benefit from warmer temperatures above 86°F (AzOPT, 2024).
Air Temperature: The ambient air temperature should be maintained 3-4 degrees warmer than the pool water (typically 93-94°F when pool water is 90°F) to prevent evaporative cooling when exiting the pool (AzOPT, 2024). This seemingly small detail significantly impacts therapeutic outcomes by maintaining muscle relaxation and preventing the uncomfortable chill that occurs when the air temperature is too low relative to the water temperature.
Water Depth: Different exercises benefit from varying water depths. Shoulder-deep water provides maximum buoyancy support and is ideal for arm exercises and overall conditioning. Waist-deep water allows for greater resistance during leg exercises and walking activities. Patients should work with their healthcare provider or aquatic therapist to determine optimal depths for their specific exercises and condition.
Swimming Equipment and Tools That Enhance the Experience
Proper swimming equipment can make aquatic exercise sessions more enjoyable, effective, and safe (Jimenez, n.d.-b):
Swim Cap: Protects hair from chlorine and other water chemicals while keeping hair from blocking your view during exercise (Jimenez, n.d.-b). Silicone caps provide better protection than latex options and are more comfortable for extended wear.
Goggles: Essential for protecting eyes and enabling clear underwater vision (Jimenez, n.d.-b). Look for comfortable goggles that seal properly without leaking and don’t create excessive pressure around the eye sockets. Anti-fog coatings help maintain visibility throughout your workout.
Sun Protection: When exercising outdoors, use waterproof sunscreen with high SPF to protect against UV exposure (Jimenez, n.d.-b). Consider wearing UV-protective swim shirts or rash guards for additional protection during extended outdoor sessions.
Waterproof Headphones: Allow you to listen to music, podcasts, or audiobooks during solo swimming sessions, making workouts more enjoyable and helping maintain motivation (Jimenez, n.d.-b). Choose models specifically designed for swimming that can withstand water immersion.
Kickboards: Many pools provide kickboards that swimmers can borrow (Jimenez, n.d.-b). These foam boards support the upper body while you focus on lower body kicking movements, isolating leg muscles and building strength. Ergonomic kickboards like the Ray-Board allow for more natural arm, shoulder, and neck posture compared to traditional flat designs, enabling longer and more comfortable kick training sessions (Ray-Board, 2023).
Pull Buoys: These foam flotation devices are placed between the upper thighs (or knees/ankles for advanced training) to help the legs float while you pull with your arms (Jimenez, n.d.-b; Williamstown Open Water Swim Coaching, 2022). Pull buoys are considered essential training equipment for swimmers because they raise the body into the correct swimming position, allow exclusive focus on upper body technique and strength, and enable longer training sessions without leg fatigue. The Taper8 ergonomic pull buoy features a contoured design that prevents slipping and chafing during workouts (Ray-Board, 2023).
Hand Paddles: While not mentioned in Dr. Jimenez’s basic recommendations, swim paddles can increase resistance during arm strokes, building upper body strength. However, these should be introduced gradually and with proper technique to avoid shoulder strain.
Aquatic Weights: Foam dumbbells provide resistance for arm exercises like bicep curls and shoulder presses, offering strength training benefits in the aquatic environment (Senior Lifestyle, 2023).
Important Safety Considerations for Swimming with Back Pain
While swimming offers tremendous benefits, individuals with back pain should observe certain precautions:
Consult Your Healthcare Provider First: Always discuss starting a swimming program with Dr. Jimenez or your healthcare provider before beginning, especially if you have a diagnosed spinal condition, recent injury, or post-surgical status (Jimenez, n.d.-b; Precision Pain Care, n.d.). Your provider can assess whether swimming is appropriate for your specific condition and provide personalized recommendations.
Start Slowly and Progress Gradually: Begin with short sessions (10-15 minutes) and slowly increase duration and intensity as your body adapts (Jimenez, n.d.-b; NuVasive, 2017). Pushing too hard too quickly can exacerbate symptoms or cause new injuries.
Listen to Your Body: If pain starts or worsens during swimming, stop the activity and consult your healthcare provider (Precision Pain Care, n.d.). Some discomfort during the first few sessions is normal as muscles adjust to new movements, but sharp pain or significantly increased symptoms indicate the need to modify or discontinue the activity.
Experiment with Different Strokes: Not all strokes work for all conditions (Precision Pain Care, n.d.). If one stroke causes discomfort, try a different one. Some individuals find that only specific strokes are comfortable for their particular back condition.
Consider Taking Lessons: Swimming lessons can teach proper technique, helping your body move through the water more efficiently and reducing the risk of strain or injury (Jimenez, n.d.-b). Learning proper form for breathing, body position, arm strokes, and kicks maximizes therapeutic benefits while minimizing injury risk.
Avoid High-Risk Water Activities: While swimming and water exercises are beneficial, activities like water slides, tube riding, and water skiing may not be appropriate for individuals with back pain due to the jarring forces and unexpected movements involved (Precision Pain Care, n.d.).
Alternative Aquatic Activities: If conventional swimming strokes prove too difficult or painful, consider aqua walking, aquatic physiotherapy, water wellbeing classes, or Good Boost personalized programs that can be tailored to your specific needs and limitations (Swimming.org, 2025).
Integrating Chiropractic Care with Swimming: A Synergistic Approach
The true power of Dr. Jimenez’s treatment philosophy lies in the strategic integration of multiple evidence-based modalities that address different aspects of spinal health. Chiropractic care and swimming complement each other perfectly, creating synergistic effects that exceed the benefits of either approach alone.
How Chiropractic Care Enhances Swimming Effectiveness
Improved Spinal Alignment Optimizes Movement Patterns: When the spine is properly aligned through chiropractic adjustments, the body can move more efficiently through the water (Tradition Health, 2024). Misalignments create compensatory movement patterns that reduce swimming efficiency and can lead to overuse injuries. By correcting these structural imbalances, chiropractic care enables swimmers to utilize proper biomechanics, reducing energy expenditure and improving performance.
Reduced Pain Enables Consistent Exercise: Chronic pain often prevents individuals from maintaining regular exercise routines. Chiropractic adjustments provide pain relief that allows patients to participate consistently in swimming programs (Tradition Health, 2024). This consistency is crucial for achieving therapeutic benefits and long-term improvements in spinal health.
Enhanced Joint Mobility Increases Range of Motion: Chiropractic care improves joint function throughout the body, not just the spine (SCUHS, 2025). Increased shoulder mobility enables better stroke mechanics, enhanced hip flexibility improves kick effectiveness, and improved spinal segmental motion allows for better body rotation during swimming strokes.
Decreased Muscle Tension Facilitates Relaxation: The muscle relaxation that occurs following chiropractic adjustments complements the relaxation benefits of warm water immersion (SCUHS, 2025). Together, these effects create profound neuromuscular relaxation that breaks the pain-spasm-pain cycle common in chronic back conditions.
Neurological Optimization Enhances Coordination: Chiropractic care improves nervous system function, which enhances proprioception (body awareness in space) and neuromuscular coordination (SCUHS, 2025). These improvements translate to better balance in the water, smoother swimming movements, and more efficient muscle recruitment patterns.
How Swimming Enhances Chiropractic Outcomes
Strengthens Muscles That Support Adjustments: One of the challenges in maintaining chiropractic corrections is that weak supporting musculature allows the spine to return to misaligned positions. Swimming builds the deep core stabilizers, back extensors, and hip muscles that hold the spine in proper alignment between chiropractic visits (US Masters Swimming, 2021). This muscular support extends the duration of chiropractic corrections and reduces the frequency of necessary adjustments over time.
Improves Cardiovascular Health for Tissue Healing: Swimming provides cardiovascular conditioning that improves circulation throughout the body (Jimenez, n.d.-b). Enhanced blood flow delivers oxygen and nutrients to injured tissues, accelerates healing, and removes metabolic waste products that contribute to inflammation and pain.
Maintains Mobility Between Chiropractic Visits: Regular swimming prevents the stiffness and decreased range of motion that can develop between chiropractic appointments (Physio Inq, 2022). This maintenance of mobility makes subsequent adjustments easier and more effective.
Promotes Healthy Posture Through Muscle Balance: Swimming engages muscles throughout the body in balanced patterns, helping correct the muscle imbalances that contribute to poor posture (US Masters Swimming, 2021). Stronger core muscles support upright sitting and standing postures, reducing the postural stress that necessitates frequent chiropractic care.
Provides Active Recovery and Regeneration: The low-impact nature of swimming makes it an ideal activity for active recovery following chiropractic adjustments (Dallas Accident & Injury Rehab, 2024). The gentle movement promotes tissue healing without the mechanical stress that could compromise recent adjustments.
A Comprehensive Treatment Protocol
Dr. Jimenez’s integrated treatment approach typically follows this evidence-based protocol:
Phase 1: Assessment and Acute Care (Weeks 1-2)
-
Comprehensive initial consultation, history taking, and physical examination
-
Advanced imaging if clinically indicated (MRI, CT, X-ray)
-
Functional medicine assessment to identify contributing factors
-
Initial chiropractic adjustments to address acute pain and restore basic function
-
Introduction to gentle aquatic activities (water walking, basic stretching)
-
Patient education on proper body mechanics, ergonomics, and self-care strategies
Phase 2: Active Treatment and Rehabilitation (Weeks 3-8)
-
Regular chiropractic adjustments (typically 2-3 times weekly initially, then gradually decreasing)
-
Progressive aquatic exercise program, including swimming strokes and aquatic strengthening
-
Soft tissue therapies (massage, myofascial release) to address muscle imbalances
-
Prescribed therapeutic exercises for home practice
-
Nutritional support and anti-inflammatory dietary recommendations
-
Lifestyle modifications and stress management techniques
Phase 3: Stabilization and Maintenance (Weeks 9-16+)
-
Maintenance chiropractic adjustments (typically every 2-4 weeks)
-
Advanced swimming program with increased duration and intensity
-
Core strengthening and functional training exercises
-
Reassessment and modification of the treatment plan based on progress
-
Transition to long-term wellness and prevention strategies
Phase 4: Wellness and Prevention (Ongoing)
-
Periodic chiropractic wellness visits (monthly or as needed)
-
Continued swimming or aquatic exercise as a lifestyle activity
-
Annual comprehensive functional medicine assessments
-
Proactive care to prevent future episodes and maintain optimal health
The Functional Medicine Difference: Dr. Jimenez’s Holistic Approach
What truly distinguishes Dr. Jimenez’s practice is his integration of functional medicine principles with chiropractic care and physical rehabilitation. As both an Institute for Functional Medicine Certified Practitioner (IFMCP) and Certified Functional Medicine Practitioner (CFMP), Dr. Jimenez evaluates patients comprehensively, addressing physical, nutritional, environmental, psychological, and genetic factors that influence health (Jimenez, n.d.-a).
The Functional Medicine Philosophy
Functional medicine represents a patient-focused healthcare approach that treats the whole person rather than isolated symptoms (Cleveland Clinic, 2025). This model emphasizes:
Root Cause Analysis: Rather than simply managing symptoms, functional medicine seeks to identify and address the underlying causes of health problems (Tradition Health, 2024). For back pain, this might include investigating inflammatory triggers, nutritional deficiencies, hormonal imbalances, gut dysbiosis, toxic exposures, or psychosocial stressors that contribute to chronic pain conditions.
Systems Biology Perspective: The body functions as an interconnected system where disruption in one area affects multiple other systems (Cleveland Clinic, 2025). Functional medicine practitioners recognize that back pain rarely exists in isolation—it often connects to digestive issues, sleep disturbances, hormonal imbalances, immune dysfunction, or psychological stress.
Personalized Treatment Plans: Rather than applying cookie-cutter protocols, functional medicine creates individualized treatment strategies based on each patient’s unique genetic makeup, biochemistry, lifestyle, and environmental factors (Nurse Practitioner Online, 2025).
Prevention and Optimization: Functional medicine extends beyond disease treatment to focus on optimizing health, preventing illness, and promoting long-term vitality (Tradition Health, 2024).
Dual-Scope Practice: Expanding Treatment Options
Dr. Jimenez’s dual licensure as both a Doctor of Chiropractic and a board-certified Family Practice Nurse Practitioner provides unique advantages that single-scope practitioners cannot offer (Academy of Anti-Aging Medicine, 2016):
Comprehensive Diagnostic Capabilities: As an FNP-BC, Dr. Jimenez can order and interpret a full range of laboratory tests, advanced imaging, and diagnostic procedures typically reserved for medical physicians. This expanded diagnostic capacity enables more thorough patient evaluation and earlier identification of complex or systemic conditions that may manifest as back pain.
Holistic Treatment Integration: The dual certification allows seamless integration of conventional medical interventions (when necessary) with chiropractic manipulations and alternative therapies (Tradition Health, 2024). This eliminates the fragmentation that often occurs when patients must see separate providers for different aspects of their care.
Medication Management When Appropriate: While Dr. Jimenez emphasizes natural, non-pharmaceutical approaches, his nurse practitioner license allows him to prescribe medications when clinically indicated for acute pain management, infection treatment, or management of comorbid conditions. This flexibility ensures patients receive appropriate care for their specific needs.
Streamlined Care and Efficiency: Patients benefit from seeing one provider who can address both their physical/structural issues (through chiropractic care) and their medical/systemic concerns (through his nurse practitioner scope). This reduces appointments, minimizes confusion, increases trust, and promotes better engagement in healthcare (University of Iowa College of Nursing, 2024).
Reduced Stigma and Enhanced Patient Empowerment: Patients appreciate the convenience and comfort of receiving comprehensive care in one location from one trusted provider (University of Iowa College of Nursing, 2024). This integrated approach empowers patients with an understanding of how their symptoms interconnect and enables them to take an active role in their healing journeys.
Functional Medicine Assessment and Treatment Components
Dr. Jimenez’s functional medicine evaluations include:
Comprehensive Laboratory Testing: Advanced blood work assessing inflammatory markers, nutrient status, hormone levels, metabolic function, and cardiovascular risk factors. Specialty testing may include food sensitivity panels, comprehensive stool analysis, organic acid testing, toxic metal evaluation, or genetic testing, depending on individual presentation.
Nutritional Assessment and Intervention: Detailed dietary analysis with personalized nutrition recommendations, anti-inflammatory dietary protocols, targeted supplementation to address deficiencies, and education on foods that support musculoskeletal health (Jimenez, n.d.-a). Proper nutrition provides the building blocks for tissue repair, modulates inflammation, and supports optimal body composition.
Lifestyle Modification Counseling: Evaluation of sleep quality and recommendations for sleep optimization, stress assessment with stress management techniques including mindfulness and meditation, physical activity recommendations beyond swimming to support overall health, and ergonomic assessment for work and home environments (Tradition Health, 2024).
Environmental Toxin Evaluation: Assessment of environmental exposures that may contribute to inflammation and chronic pain, recommendations for reducing toxic burden, and support for detoxification pathways.
Gut Health Optimization: Recognition that gut health profoundly impacts inflammation, immune function, and pain perception. Evaluation and treatment of intestinal permeability (“leaky gut”), dysbiosis, and digestive dysfunction (Tradition Health, 2024).
Preventing Future Injuries: Proactive Spine Health Strategies
While addressing current back pain remains the primary focus for most patients initially, long-term success requires proactive strategies to prevent future episodes and maintain optimal spinal health.
Importance of Prevention in Sports Medicine and Daily Life
Prevention represents a cornerstone of both chiropractic philosophy and functional medicine (Advanced Spine & Posture, 2024). For athletes, injury prevention enables consistent training, peak performance, and extended career longevity. For the general population, prevention minimizes disability, reduces healthcare costs, maintains productivity, and preserves quality of life.
Regular chiropractic care serves as preventive medicine by:
-
Maintaining proper spinal alignment to prevent compensatory problems
-
Identifying and correcting minor dysfunctions before they become painful conditions
-
Strengthening supporting musculature through prescribed exercises
-
Educating patients about proper body mechanics and lifestyle factors
Swimming complements injury prevention by:
-
Building functional strength in muscles that support the spine
-
Maintaining joint mobility and flexibility throughout the musculoskeletal system
-
Providing cardiovascular conditioning that supports overall health
-
Offering a safe exercise option that carries low injury risk
Key Injury Prevention Strategies
Maintain Regular Chiropractic Care: Even after acute symptoms resolve, periodic chiropractic visits help maintain spinal alignment and catch minor problems before they become significant (Medical Wellness Group, 2023). Many patients find that monthly or quarterly maintenance adjustments prevent the recurrence of back pain episodes.
Continue Swimming as a Lifestyle Activity: Rather than viewing swimming as temporary physical therapy, embrace it as a lifelong fitness activity (Physio Inq, 2022). Regular swimming (2-3 times weekly) maintains strength, flexibility, and cardiovascular fitness, which protect against future back problems.
Practice Proper Ergonomics: Optimize workstation setup with appropriate chair height, monitor position, keyboard placement, and desk arrangement (Sleigh Family Chiropractic, 2024). When standing for extended periods, use anti-fatigue mats and alternate weight between feet. Practice proper lifting mechanics by bending at the knees rather than the waist and holding objects close to the body.
Strengthen Core Muscles: Beyond swimming, incorporate land-based core strengthening exercises, including planks, bird dogs, dead bugs, and bridges (Advanced Spine & Posture, 2024). Strong abdominal and back muscles provide essential support for the spine and reduce injury risk.
Maintain Healthy Body Weight: Excess body weight increases mechanical stress on the spine, particularly the lumbar region. Dr. Jimenez’s functional medicine approach addresses weight management through comprehensive nutrition, metabolic optimization, and sustainable lifestyle modifications rather than restrictive dieting.
Stay Active Throughout the Day: Prolonged sitting represents one of the most significant risk factors for back pain (The Disease of Sitting, n.d.). Take frequent breaks to stand, stretch, and move. Consider a standing desk or treadmill desk for part of the workday. Use walking meetings when possible and take stairs instead of elevators.
Address Psychosocial Factors: Chronic stress, anxiety, and depression contribute to muscle tension, poor posture, and pain perception. Incorporate stress management techniques such as meditation, deep breathing, yoga, or counseling. Adequate sleep (7-9 hours nightly) proves essential for tissue repair and pain management.
Avoid Smoking: Tobacco use impairs circulation, reduces oxygen delivery to tissues, accelerates disc degeneration, and interferes with healing. Smoking cessation should be prioritized for anyone with back pain or spinal conditions.
Wear Supportive Footwear: Poor footwear creates abnormal gait patterns that stress the spine. Choose shoes with appropriate arch support and cushioning. Avoid wearing high heels for extended periods.
Special Populations: Tailoring Treatment Approaches
Dr. Jimenez’s comprehensive practice serves diverse patient populations, each requiring individualized treatment modifications:
Athletes and Active Individuals
Athletes face unique challenges, including high training volumes, sport-specific movement patterns that create repetitive stress, and pressure to return to competition quickly following injury (Advanced Spine & Posture, 2024). Dr. Jimenez’s sports medicine expertise enables him to provide:
-
Injury screening and biomechanical assessments to identify risk factors
-
Sport-specific rehabilitation protocols that maintain conditioning while allowing healing
-
Performance optimization through spinal alignment and functional movement training
-
Rapid recovery interventions, including chiropractic adjustments, soft tissue therapy, and aquatic rehabilitation
Older Adults and Seniors
Aging brings changes, including decreased bone density, reduced muscle mass, diminished flexibility, slower healing, and increased prevalence of degenerative conditions (HydroWorx, 2023). Aquatic exercise proves particularly beneficial for older adults because:
-
Buoyancy supports movement and reduces fall risk
-
Warm water relieves arthritis pain and stiffness
-
Resistance training builds muscle and bone strength without heavy weights
-
Social group classes combat isolation and enhance adherence
Dr. Jimenez modifies chiropractic techniques for older patients, using gentler adjustments, avoiding contraindicated procedures in osteoporotic patients, and coordinating care with other healthcare providers managing age-related conditions.
Post-Surgical Patients
Following spinal surgery, patients require carefully progressive rehabilitation (Sutton Place PT, 2024). Aquatic therapy often represents the first rehabilitation step because:
-
Buoyancy reduces stress on healing surgical sites
-
Warm water promotes circulation and tissue healing
-
Graded progression from non-weight-bearing to full weight-bearing activities occurs naturally by adjusting water depth
-
Pain is better controlled in the aquatic environment
Dr. Jimenez collaborates with surgical specialists to coordinate post-operative care, ensuring patients receive appropriate rehabilitation at each healing stage.
Pregnant and Postpartum Women
Pregnancy creates significant biomechanical changes, including increased lumbar lordosis, anterior pelvic tilt, joint laxity from relaxin hormone, and weight gain concentrated anteriorly (Jimenez, n.d.-a). These changes frequently cause back pain. Chiropractic care and swimming offer safe, effective treatment options during pregnancy and facilitate postpartum recovery.
Occupational Injury Patients
Workers’ compensation and occupational injury cases require meticulous documentation, coordinated care with employers and case managers, and functional capacity evaluations (Jimenez, n.d.-a). Dr. Jimenez’s comprehensive approach addresses not only the injury itself but also ergonomic factors, workplace modifications, and safe return-to-work protocols.
The Business of Healing: Making Care Accessible and Convenient
Dr. Jimenez recognizes that healthcare should be accessible to everyone, not just those with comprehensive insurance coverage or significant financial resources. His El Paso clinics operate on principles of convenience, affordability, and transparency (Jimenez, n.d.-a):
Multiple Convenient Locations: Three El Paso facilities (East Side Main Clinic, Central Rehabilitation Center, and North East Rehabilitation & Fitness Center) provide convenient access regardless of where patients live or work.
Flexible Payment Options: Rather than forcing patients to navigate complex insurance billing, copays, deductibles, or declined reimbursements, the practice offers straightforward pricing and payment plans. This transparency eliminates financial surprises and makes regular care affordable.
Insurance Compatibility: For patients who prefer to use insurance benefits, the practice works with most insurance carriers to maximize coverage.
Virtual Health Coaching: Telehealth options extend care to patients who cannot easily travel to the clinic, those who need more frequent check-ins between appointments, or individuals seeking lifestyle coaching and wellness support.
No Insurance Hassles: Patients can receive high-quality care without dealing with insurance paperwork, pre-authorizations, or claims denials. This direct-pay model often proves more affordable than traditional insurance-based care when considering deductibles and copays.
Patient Success Stories: Real Results from Integrated Care
While individual results vary, many patients experience transformative improvements through Dr. Jimenez’s integrated chiropractic and aquatic exercise approach:
“After years of chronic lower back pain that limited my ability to work and enjoy activities with my family, I found Dr. Jimenez’s clinic. His comprehensive evaluation identified several factors contributing to my pain that previous doctors had missed. Through regular chiropractic adjustments combined with a swimming program, I’ve regained my quality of life. I’m now pain-free most days and have the energy to keep up with my grandchildren.” – Patient testimonial (Jimenez, n.d.-a)
“As a competitive athlete, I was devastated when back pain threatened to end my season. Dr. Jimenez’s sports medicine expertise and dual-scope practice allowed him to provide comprehensive care that addressed both my immediate pain and the underlying biomechanical issues. The aquatic rehabilitation program enabled me to maintain cardiovascular fitness while healing. I returned to competition ahead of schedule and performed better than before the injury.” – Athlete patient (Jimenez, n.d.-a)
The Injury Medical Chiropractic and Functional Medicine Clinic has successfully treated thousands of El Paso residents over more than two decades, earning recognition as El Paso’s top chiropractic and wellness provider (Jimenez, n.d.-a).
Conclusion: Taking Control of Your Spinal Health Journey
Chronic back pain need not be a life sentence of disability, medication dependence, or surgical intervention. The synergistic combination of evidence-based chiropractic care and therapeutic aquatic exercise offers a powerful, natural approach to spinal health that addresses both structural alignment and functional capacity. By incorporating functional medicine principles that identify and treat root causes rather than merely suppressing symptoms, this comprehensive approach delivers lasting results that extend far beyond temporary pain relief.
Dr. Alexander Jimenez’s unique qualifications—combining expertise as a board-certified Family Practice Nurse Practitioner, Doctor of Chiropractic, and Institute for Functional Medicine Certified Practitioner—position him to deliver truly integrative care that bridges conventional and alternative medicine. His use of advanced imaging and diagnostic evaluations to clinically associate patient injuries with underlying pathology ensures accurate diagnosis and appropriate treatment. His dual-scope practice eliminates the fragmentation that plagues modern healthcare, providing patients with comprehensive evaluation and treatment under one roof.
The integration of swimming and aquatic exercise amplifies the benefits of chiropractic adjustments by building the muscular support necessary to maintain spinal corrections. It improves cardiovascular health, accelerates healing, maintains mobility between chiropractic visits, and provides a sustainable, enjoyable form of exercise that patients continue long-term. The unique properties of water—including buoyancy that reduces spinal compression, resistance that builds functional strength, warmth that promotes relaxation and healing, and hydrostatic pressure that reduces inflammation—create an ideal environment for musculoskeletal rehabilitation.
Whether you’re currently suffering from acute back pain following an injury, managing chronic spinal conditions that have persisted for years, recovering from spinal surgery, seeking to optimize athletic performance, or simply wanting to maintain your spinal health and prevent future problems, the comprehensive approach pioneered by Dr. Jimenez offers evidence-based solutions tailored to your unique needs, goals, and circumstances.
Taking the Next Step
If you’re ready to break free from the limitations of chronic back pain and experience the transformative benefits of integrated chiropractic and aquatic therapy, consider the following steps:
-
Schedule a Consultation: Contact Injury Medical Chiropractic and Functional Medicine Clinic at one of their three El Paso locations to schedule a comprehensive initial evaluation with Dr. Jimenez.
-
Prepare for Your Appointment: Gather relevant medical records, imaging reports, and medication lists, and complete any intake paperwork provided by the clinic. Prepare to discuss your health history, current symptoms, previous treatments, and health goals.
-
Commit to the Process: Healing takes time and requires active participation. Be prepared to attend regular appointments, complete prescribed exercises, make recommended lifestyle modifications, and practice self-care strategies between visits.
-
Start Swimming: Even before your initial chiropractic appointment, you can begin gentle water walking or aquatic exercises (after consulting your current healthcare provider). Find a local pool, invest in basic equipment like goggles and a swim cap, and start experiencing the therapeutic benefits of aquatic exercise.
-
Embrace a Wellness Mindset: Shift from a reactive “sick care” mentality to a proactive wellness approach. View chiropractic care and swimming not as temporary fixes but as lifelong practices that support optimal health and vitality.
-
Stay Educated: Continue learning about spinal health, functional medicine, and natural healing approaches. Dr. Jimenez’s extensive online resources, including articles, videos, and educational materials at https://dralexjimenez.com/, provide valuable information to support your healing journey.
-
Be Patient and Persistent: Some patients experience immediate relief, while others require several weeks or months of consistent care before achieving significant improvements. Trust the process, communicate openly with Dr. Jimenez about your progress, and remain committed to your treatment plan.
A Commitment to Your Health
Dr. Jimenez’s practice philosophy centers on one fundamental principle: “I assure you, I will only accept the best for you” (Jimenez, n.d.-a). This commitment drives every aspect of care delivered at Injury Medical Chiropractic and Functional Medicine Clinic, from thorough initial evaluations to personalized treatment plans, from cutting-edge diagnostic technology to compassionate, patient-centered care delivery.
The clinic’s mission extends beyond symptom relief to helping patients live fulfilled lives with more energy, positive attitudes, better sleep, less pain, proper body weight, and the knowledge to maintain these improvements long-term. Through the integration of chiropractic adjustments, aquatic exercise, functional medicine, and lifestyle optimization, this holistic approach empowers patients to take control of their health and thrive in El Paso’s vibrant community.
Your journey to optimal spinal health and freedom from back pain begins with a single decision—the decision to seek comprehensive, evidence-based care that treats you as a whole person rather than a collection of symptoms. Whether you’re an athlete seeking peak performance, a worker sidelined by occupational injury, a senior wanting to maintain independence and mobility, or anyone in between, Dr. Jimenez and his dedicated team are ready to guide you toward lasting healing and wellness.
Important Disclaimer and Serious Note to Readers
This blog post is intended for educational and informational purposes only and should be taken seriously as a resource for understanding spinal health, chiropractic care, and aquatic exercise. The information presented herein does not constitute medical advice, diagnosis, or treatment recommendations for any specific individual. Every person’s health situation is unique, and what works for one patient may not be appropriate for another.
Before beginning any new exercise program, including swimming or aquatic therapy, or pursuing chiropractic treatment, you must consult with a qualified healthcare provider who can evaluate your specific condition, medical history, contraindications, and individual needs. Certain spinal conditions, acute injuries, post-surgical states, cardiovascular problems, pregnancy complications, or other medical issues may contraindicate swimming, chiropractic adjustments, or specific therapeutic interventions.
Do not disregard, avoid, or delay obtaining professional medical advice because of information you have read in this blog post. If you experience severe back pain, radiating pain into the extremities, bowel or bladder dysfunction, unexplained weight loss, fever, or other concerning symptoms, seek immediate medical evaluation to rule out serious underlying conditions requiring urgent intervention.
The testimonials and success stories referenced in this post represent individual experiences and do not guarantee similar results for all patients. Treatment outcomes depend on numerous factors, including diagnosis accuracy, condition severity, patient compliance, overall health status, and individual healing capacity.
Dr. Alexander Jimenez’s practice operates in accordance with state licensing requirements, scope of practice regulations, and professional standards of care. Patients should verify that any healthcare provider they consult maintains current licensure, appropriate credentials, and professional liability insurance.
Swimming and aquatic exercise carry inherent risks, including drowning, slipping, cardiovascular events, and injury. Never swim alone, always follow pool safety rules, know your limitations, and stop any activity that causes significant pain or distress.
This blog post references clinical research studies to support the efficacy of chiropractic care and aquatic exercise. While this research provides evidence for these approaches, readers should understand that all medical interventions carry potential risks and benefits that must be individually assessed.
By reading this blog post, you acknowledge that you understand these limitations and will consult appropriate healthcare professionals before making any decisions regarding your health care. The author, Dr. Alexander Jimenez, Injury Medical Chiropractic and Functional Medicine Clinic, and any associated parties assume no liability for actions taken based on information presented in this post.
Your health and safety remain paramount. Please take this information seriously and use it as a starting point for informed discussions with your healthcare providers.
References
- Academy of Anti-Aging Medicine. (2016). Dr. Alex Jimenez, DC, APRN, FNP-BC, CFMP, IFMCP. Retrieved from https://www.a4m.com/alex-jimenez-injury-medical-amp-chiropractic-clinic-el-paso-tx.html
- Advanced Spine & Posture. (2024). Corrective exercises for spinal health. Retrieved from https://advancedspineandposture.com/blog/corrective-exercises-for-spinal-health/
- Advanced Spine & Posture. (2024). Sports injuries treated with chiropractic care. Retrieved from https://advancedspineandposture.com/blog/sports-injuries-treated-with-chiropractic-care/
- American Association of Neurological Surgeons. (2024). Anatomy of the spine and peripheral nervous system. Retrieved from https://www.aans.org/patients/conditions-treatments/anatomy-of-the-spine-and-peripheral-nervous-system/
- AzOPT. (2024). Optimizing aquatic therapy: The critical role of air and water temperature. Retrieved from https://azopt.net/air-and-water-temperature-for-aquatic-therapy/
- Blakehurst LCS. (2025). 11 simple water exercises for seniors. Retrieved from https://blakehurstlcs.com/blog/water-exercises-for-seniors/
- Cleveland Clinic. (2025). Integrative medicine: What is it, types, risks & benefits. Retrieved from https://my.clevelandclinic.org/health/treatments/21683-integrative-medicine
- Cityview Chiropractor. (2025). 10 best benefits of chiropractic care for back pain. Retrieved from https://cityviewchiropractor.com/10-best-benefits-of-chiropractic-care-for-back-pain/
- Dallas Accident & Injury Rehab. (2024). Proven chiropractic methods for sports injury rehabilitation. Retrieved from https://dallasaccidentandinjuryrehab.com/proven-chiropractic-methods-for-sports-injury-rehabilitation/
- Doc Moss. (2024). The benefits of chiropractic care for chronic pain management. Retrieved from https://docmoss.com/the-benefits-of-chiropractic-care-for-chronic-pain-management/
- Duke Health. (2025). Should you see a chiropractor for back pain? Retrieved from https://www.dukehealth.org/blog/should-you-see-chiropractor-back-pain
- Great Lakes Medical Imaging. (2025). Can advanced imaging help detect hidden causes of chronic back pain. Retrieved from https://www.glmi.com/blog/can-advanced-imaging-help-detect-hidden-causes-of-chronic-back-pain
- GWRY MCA. (2022). Freestyle swimming technique: Tips for beginners. Retrieved from https://gwrymca.org/blog/freestyle-swimming-technique-tips-for-beginners
- Helen Hayes Hospital. (2021). The benefits of aquatic therapy. Retrieved from https://helenhayeshospital.org/the-benefits-of-aquatic-therapy/
- HydroWorx. (2023). Benefits of aquatic exercises & aerobics for seniors. Retrieved from https://www.hydroworx.com/research-education/additional-resources/aquatic-exercises-for-seniors/
- International Chiropractors Association. (n.d.). Consultation, history and examination. Retrieved from https://chiro.org/documentation/DISCONTINUED/ICA_INITIAL%20EXAM.pdf
- Jimenez, A. (n.d.-a). El Paso, TX family practice nurse practitioner and chiropractor. Retrieved from https://dralexjimenez.com/
- Jimenez, A. (n.d.-b). Starting swimming exercises for back health: EP chiropractic. Retrieved from https://dralexjimenez.com/starting-swimming-exercises-for-back-health-ep-chiropractic/
- Kenhub. (2023). Musculoskeletal system: Anatomy and functions. Retrieved from https://www.kenhub.com/en/library/anatomy/the-musculoskeletal-system
- KMC University. (2024). Examination should be driven by history. Retrieved from https://kmcuniversity.com/examination-should-be-driven-history-1/
- Medical Wellness Group. (2023). The benefits of chiropractic care for back pain: A comprehensive guide. Retrieved from https://medicalwellnessgroup.org/the-benefits-of-chiropractic-care-for-back-pain-a-comprehensive-guide/
- National Spine Health Foundation. (2024). The spine: Anatomy and function. Retrieved from https://spinehealth.org/article/spine-anatomy/
- Nurse Practitioner Online. (2025). Why choose a functional medicine nurse practitioner (FMNP). Retrieved from https://www.nursepractitioneronline.com/specialties/functional-medicine-nurse-practitioner/
- NuVasive. (2017). Swim your way to back pain relief. Retrieved from https://www.nuvasive.com/swim-way-back-pain-relief/
- Penn Spine & Orthopedic. (2024). Swimming for back pain. Retrieved from https://pennspineandortho.com/back-pain/swimming-for-back-pain/
- Peng, M. S., Wang, R., Wang, Y. Z., Chen, C. C., Wang, J., Liu, X. C., … & Chen, P. J. (2022). Efficacy of therapeutic aquatic exercise vs physical therapy modalities for patients with chronic low back pain: A randomized clinical trial. JAMA Network Open, 5(1), e2142069. doi:10.1001/jamanetworkopen.2021.42069
- Physio Inq. (2022). Swimming for lower back pain: The research. Retrieved from https://www.physioinq.com.au/blog/swimming-for-lower-back-pain-the-research
- PMC. (2022). Effect of aquatic physical therapy on chronic low back pain. Retrieved from https://pmc.ncbi.nlm.nih.gov/articles/PMC9717486/
- Precision Pain Care. (n.d.). Swimming to help you manage your pain. Retrieved from https://precisionpaincare.org/swimming_backpain.html
- Ray-Board. (2023). The most comfortable swim kickboard you will ever use. Retrieved from https://ray-board.com
- Recovery Chiro Med. (2024). Full body chiropractic adjustment for back pain relief: What you need to know. Retrieved from https://recoverychiromed.com/full-body-chiropractic-adjustment-for-back-pain-relief-what-you-need-to-know/
- SCUHS. (2025). Top 10 benefits of going to a chiropractor for pain relief. Retrieved from https://www.scuhs.edu/dc-article/top-10-benefits-of-going-to-a-chiropractor/
- Senior Lifestyle. (2023). 5 simple and fun water aerobics exercises for seniors. Retrieved from https://www.seniorlifestyle.com/resources/blog/5-best-water-aerobics-exercises-seniors/
- Shi, Z., Zhou, H., Lu, L., Pan, B., Wei, Z., Yao, X., … & Feng, S. (2018). Aquatic exercises in the treatment of low back pain: A systematic review of the literature and meta-analysis of eight studies. American Journal of Physical Medicine & Rehabilitation, 97(2), 116-122. doi:10.1097/PHM.0000000000000801
- Sleigh Family Chiropractic. (2024). Chiropractic adjustments for better posture: Benefits & techniques. Retrieved from https://sleighfamilychiropractic.com/how-chiropractic-adjustments-enhance-posture-and-improve-spinal/
- Spine Diagnostic. (2025). Advanced diagnostic tools: MRI, CT & fluoroscopy in diagnosing spinal pain. Retrieved from https://spinediagnostic.com/advanced-diagnostic-tools-mri-ct-fluoroscopy-in-diagnosing-spinal-pain/
- Spine-health. (2017). Spinal discs. Retrieved from https://www.spine-health.com/conditions/spine-anatomy/spinal-discs
- Spine. MD. (2022). Swimming for back pain: What you need to know. Retrieved from https://www.spine.md/insights/articles/swimming-for-back-pain/
- Sutton Place PT. (2024). How aquatic therapy can help you rehab from spinal surgery. Retrieved from https://www.suttonplacept.com/blog/How-Aquatic-Therapy-Can-Help-You-Rehab-from-Spinal-Surgery
- Swimming.org. (2025). Musculoskeletal conditions and swimming. Retrieved from https://www.swimming.org/justswim/musculoskeletal-conditions-swimming/
- Texas Spine & Sports Therapy Center. (2025). The connection between posture and chronic pain. Retrieved from https://texasspineandsportstherapy.com/the-connection-between-posture-and-chronic-pain/
- Tigard Chiropractic Auto Injury. (2024). Chiropractic care in integrated health: Bridging traditional and alternative medicine. Retrieved from https://www.tigardchiropracticautoinjury.com/blog/chiropractic-care-in-integrated-health-bridging-traditional-and-alternative-medicine
- Tradition Health. (2024). How functional medicine powerfully complements chiropractic care for holistic health. Retrieved from https://traditionhealth.com/2024/08/16/how-functional-medicine-complements-chiropractic-care-for-holistic-health/
- University of Iowa College of Nursing. (2024). Leadership for an innovative practice role: The dually certified nurse practitioner. Retrieved from https://nursing.uiowa.edu/news/2024/01/dually-certified
- US Masters Swimming. (2021). 3 reasons why swimming is great for musculoskeletal strength. Retrieved from https://www.usms.org/fitness-and-training/articles-and-videos/articles/3-reasons-why-swimming-is-great-for-musculoskeletal-strength
- Versus Arthritis. (n.d.). Hydrotherapy: Benefits and how it can help. Retrieved from https://versusarthritis.org/about-arthritis/treatments/therapies/hydrotherapy/
- Williamstown Open Water Swim Coaching. (2022). Should I use swim training equipment like flippers, paddles, pull buoys, boards, etc.. Retrieved from https://williamstownopenwaterswimcoaching.com/2022/01/31/should-i-use-swim-training-equipment-like-flippers-paddles-pull-buoys-boards-etc/