
MVA’s Recovery and Healing at El Paso Back Clinic
Common Motor Vehicle Accidents in El Paso: Recovery and Healing at El Paso Back Clinic®
Motor vehicle accidents, or MVAs, are a big issue in El Paso. This city sits on the border, with lots of trucks and cars zooming on roads like I-10 and Loop 375. Accidents often result from drivers not paying attention, drinking, or speeding. They can lead to injuries like neck pain or broken bones. At El Paso Back Clinic®, we help people heal from these injuries. Our team, led by Dr. Alexander Jimenez, uses integrative chiropractic care. This mixes spine fixes with massage, exercise, and healthy eating tips. It treats the whole body and mind. In this article, we discuss common crashes in El Paso, the harm they cause, and how our clinic supports recovery. We draw on Dr. Jimenez’s expertise at our locations in El Paso, TX.
El Paso has many crashes each year. Recent data shows thousands of wrecks, with injuries and even deaths. The border sees heavy truck traffic, upping the risks. Dust storms or rain-slick roads. Work zones add hazards. Knowing this helps folks drive safely. At El Paso Back Clinic®, we see many patients from these events. Our care focuses on pain relief and full health.
Common Types of Motor Vehicle Accidents in El Paso
El Paso’s roads mix locals, visitors, and cross-border traffic. This leads to jam-ups and crashes. Here are the key types:
- Distracted Driving Accidents: Phones or snacks pull drivers’ eyes from the road. In El Paso, this sparks many wrecks. Texting hits hard at spots like Mesa and Stanton streets. Texas-wide, it caused over 84,000 crashes in one year.
- Drunk or Impaired Driving: Booze or drugs slow folks down. Crashes spike nights and weekends. It’s a top cause in Texas spots like El Paso. They pop up near fun zones like Cincinnati Avenue.
- Speeding-Related Crashes: Too fast means tough stops. It makes up 30% of Texas wrecks. On I-10 and Loop 375, speed leads to bad hits. Winds make it worse.
- Rear-End Collisions: Cars bump backs from close follows or late brakes. Common on Loop 375 in traffic or near shops like Cielo Vista. Distractions or weather help cause them.
- Intersection Crashes: Red-light runs or no yields cause side smacks. Over half happen at crossings like Montana or Zaragoza. The Spaghetti Bowl adds mess. Stop sign skips are big faults.
- Pedestrian Incidents: Walkers get struck when drivers miss spots or speed. Downtown, schools, or UTEP see many. Poor walks led to many deaths lately.
- Truck Accidents: Border hauls mean big trucks everywhere. Thousands cross yearly. Recent counts show many truck wrecks with injuries. Tired drivers, heavy loads, or blind areas cause them. Spots like I-10, US-54, and Loop 375 are hot.
Pile-ups hit in storms on I-10. Lane changes in builds confuse. Hit-runs occur in town. Stay alert, slow down, and watch out for trucks to avoid.
At El Paso Back Clinic®, we treat folks from all these. Our team knows border traffic woes. We offer care plans for quick heals.
Common Injuries Sustained in Motor Vehicle Accidents
MVAs jolt bodies hard. Sudden moves cause hidden hurts. Here are the usual ones:
- Whiplash: Neck snaps cause pain, stiffness, headaches, and dizziness. Top in rear-ends.
- Neck and Back Sprains: Pulls or tears cause pain and reduced movement. Low back twists.
- Soft Tissue Damage: Bruises, rips in muscles. Swell, stiff. Deep ones last.
- Headaches: From whiplash or bumps. They linger.
- Herniated Discs: Spine pads slip, pinch nerves. Pain shoots.
- Fractures: Breaks from hits. Ribs puncture lungs. Bad ones need ops. Limbs, spine too.
- Traumatic Brain Injuries (TBIs): Head knocks cause mix-ups, forgetfulness, and eye issues. Change lives, cost lots.
Shoulders, knees, and inside bleed too. Burns and scars are possible. Trucks crush more. Walkers break bones, heads. Minor ones spark worry or PTSD.
At our clinic, we spot these early. Dr. Jimenez’s team uses checks to plan care.
How These Injuries Occur
Crashes stop or hit fast. Bodies fly in cars. Belts save, but force hurts. Rear-ends jerk heads, stretch necks for whiplash. Sides twist spines for sprains, disc slips. Heads hit for TBIs. Knees dash-bang for sprains. Moves inflame tissues. Trucks smash small cars, break bones. Walkers fly, land hard. Signs may be delayed, so check soon.
We urge quick visits. Our El Paso spots offer fast help.
Integrative Chiropractic Care at El Paso Back Clinic® for MVA Recovery
Our integrative care treats all of you. We fix spines hands-on, easing pain without pills or cuts first. Mixes old ways with massage, PT, and nutrition. Speeds heal, drops swell. Here’s our approach:
- Spinal Adjustments: Move bones right, cut nerve pinch, up move. Great for whiplash, back.
- Massage Therapy: Loosens muscles, breaks scars. Boosts blood, drops swell in tissues.
- Physical Therapy: Builds strong, flexible. Restores after sprains and breaks.
- Nutritional Support: Food advice; adds fight-swell, up mood.
- Other Therapies: Needle work or disc pull. Ease pain, stress.
We speed recovery, hit the body and feelings. Start in 72 hours, best. Stops long pain. Our functional medicine finds roots.
Insights from Dr. Alexander Jimenez and El Paso Back Clinic®
Dr. Alexander Jimenez, DC, APRN, FNP-BC, has headed El Paso Back Clinic® for 30+ years. He excels in MVA, which includes injuries like whiplash and TBIs. We use functional medicine, nutrition, and rehab. Holistic care heals body and mind from trauma. Cases show fast recovery from car and truck hits. Border traffic brings many to us. Our spots at 11860 Vista Del Sol and 6440 Gateway East offer full care. Call 915-850-0900 for help.
Conclusion
El Paso MVAs from busy roads hurt many. From whiplash to TBIs, harms vary. El Paso Back Clinic® gives natural healing. We cut pain, restore movement. See us after crashes. Safe drives prevent woes. Visit elpasobackclinic.com or call for wellness.
References
A2X Law. (n.d.). El Paso car crash statistics. https://www.a2xlaw.com/el-paso-car-crash-statistics
Abrar and Vergara. (n.d.). El Paso car accident statistics. https://theavlawyer.com/el-paso-car-accident-lawyer/statistics/
Altitude Health. (n.d.). Comprehensive care: Integrating chiropractic, physiotherapy, naturopathy, and more for motor vehicle accident recovery. https://www.altitudehealth.ca/comprehensive-care-integrating-chiropractic-physiotherapy-naturopathy-and-more-for-motor-vehicle-accident-recovery/
Amaro Law Firm. (n.d.). El Paso truck accident lawyer. https://amarolawfirm.com/el-paso-truck-accident-lawyer/
Amanda Demanda Injury Lawyers. (n.d.). What Texas cities have the most car accidents?. https://www.callamandademanda.com/blog/tx-cities-most-accidents/
Arnold & Itkin. (n.d.). El Paso truck accident attorneys. https://www.arnolditkin.com/el-paso-personal-injury/truck-accidents/
Azam Injury Law. (n.d.). El Paso motor vehicle accident lawyer – Free help. https://azaminjurylaw.com/area-we-serve/el-paso/motor-vehicle-accident-lawyer/
Dr. Alexander Jimenez, DC, APRN, FNP-BC, IFMCP, CFMP, ATN ♛. (n.d.). LinkedIn profile. https://www.linkedin.com/in/dralexjimenez/
Harmonson Law Firm. (n.d.). El Paso car accident lawyer. https://www.clarkharmonsonattorney.com/el-paso-tx/car-accident-lawyer/
Harmonson Law Firm. (n.d.). El Paso pedestrian accident attorney. https://www.clarkharmonsonattorney.com/el-paso-tx/pedestrian-accident-lawyer/
Injury Medical Clinic PA. (n.d.). Injury specialists. https://dralexjimenez.com/
Inlet Integrated Health Centre. (n.d.). Common injuries from motor vehicle accidents and how chiropractic, physiotherapy, and kinesiology can help. https://www.inletintegratedhealth.com/post/common-injuries-from-motor-vehicle-accidents-and-how-chiropractic-physiotherapy-and-kinesiology-ca
James Kennedy, P.L.L.C. (n.d.). El Paso rear-end collisions attorneys | Free consultation. https://www.epinjury.com/personal-injury/car-accident-crash-wreck/rear-end-collisions
Labinoti Law Firm. (n.d.). El Paso motor vehicle accident attorney. https://www.labinotilaw.com/office-locations/el-paso/personal-injury/motor-vehicle-accident/
MVAMVP. (n.d.). Why chiropractic care is essential after a motor vehicle accident. https://mvamvp.com/why-chiropractic-care-is-essential-after-a-motor-vehicle-accident/
Nix Patterson, LLP. (n.d.). El Paso car accident lawyers. https://nixlaw.com/el-paso/car-accident-lawyers/
Sodhi, R. (n.d.). What you should know about the role of chiropractic and massage in motor vehicle accident recovery. https://www.alwc.ca/role-of-chiropractic-care-and-massage-for-accident-recovery/
Spectrum Therapy Consultants. (n.d.). Motor vehicle accident injuries. https://spectrumtherapyconsultants.com/physical-therapy-services/motor-vehicle-accident-injuries/
The Neck and Back Clinics. (n.d.). Your first chiropractic appointment after a car accident: What to expect and prepare. https://theneckandbackclinics.com/first-chiropractic-appointment/
The Neck and Back Clinics. (n.d.). What are your chiropractic treatment options after a car accident?. https://theneckandbackclinics.com/what-are-your-chiropractic-treatment-options-after-a-car-accident/
The Russo Firm. (n.d.). Where do most El Paso car accidents occur?. https://therussofirm.com/where-do-most-el-paso-car-accidents-occur/

Mobility Challenges in Mexican and Mexican Americans Explained
Mobility Challenges in Mexican and Mexican American Communities: Insights from El Paso Back Clinic®
At El Paso Back Clinic® in El Paso, TX, we see many patients from Mexican and Mexican American backgrounds facing mobility issues. These problems often stem from tough jobs, health factors like obesity, and aging. Our wellness chiropractic care focuses on pain relief and improved movement. This article discusses common issues such as arthritis and back pain, supported by studies. We’ll explain how our team, including Dr. Alexander Jimenez, DC, APRN, FNP-BC, uses integrative approaches to help. If you’re in El Paso dealing with these, our clinic is here for you.
Common Musculoskeletal Mobility Issues We Treat
Musculoskeletal problems affect your bones, muscles, and joints, making it difficult to move freely. At our clinic, we see these issues often in our community, where many work in demanding fields like farming or construction.
Arthritis, especially in the knees, is a top concern. It causes joint wear-related swelling and pain. In Mexico, about 20-25% of adults aged 40+ have it, with higher rates among women (Villarreal Rizzo et al., 2025). Mexican Americans in the U.S. also face risks, like osteoporosis weakening bones in 16% of women (Wright et al., n.d.). At El Paso Back Clinic®, we help ease this with gentle adjustments and exercises.
Chronic low back pain hits hard, too. It comes from prolonged lifting or standing. In Mexico, it’s the leading cause of disability, with 840.6 cases per 100,000 in 2021 (Clark et al., 2023). Among farmworkers here in Texas, 46.9% report back issues affecting daily life (Weigel et al., 2013). Our chiropractic care targets this to get you moving again.
Work injuries often involve the shoulders, wrists, and legs. Repetitive tasks in jobs cause rotator cuff problems in 19.1% and elbow pain in 20.2% of Latino workers (Mora et al., 2014). Older adults in our area are at risk of frailty due to ongoing pain, leading to reduced mobility (National Institutes of Health, n.d.). Women face more disability in tasks like walking, with arthritis raising risks by 35% over time (Rodriguez et al., 2021).
Here are key facts we see in our patients:
- Arthritis rates: 19.6% for knee issues in Mexicans over 40, up to 24.2% in women (Ciampi de Andrade et al., 2022).
- Back pain: Affects 16.9% of farmworkers from repetitive strain (Mora et al., 2014).
- Craft-related injuries: Neck and knee pain from activities like weaving (Jeanson et al., 2025).
- Disability trends: Physical function declines by 0.18 points per year with arthritis (Rodriguez et al., 2021).
Jobs in agriculture and construction drive these, plus obesity adds joint stress. In our Mexican American patients, higher BMI initially slows strength loss but worsens it later (Davis & Al Snih, 2025). About 83% of Hispanic men are overweight, linked to less activity (Valdez et al., 2019). At El Paso Back Clinic®, we address this with personalized plans.
Neuromusculoskeletal Issues Addressed at Our Clinic
These issues combine nerve problems with muscle and bone pain, leading to numbness or weakness. Our wellness approach helps restore nerve function and reduce discomfort.
Chronic low back pain is common, often due to nerve compression. It’s the main cause of disability in Mexico (Alva Staufert et al., 2021). Knee and foot arthritis affects movement, with 25.5% showing joint changes (Ciampi de Andrade et al., 2022). We treat foot pain from standing jobs, seen in 4.8% of workers (Mora et al., 2014).
Shoulder injuries, such as rotator cuff tears, are associated with overhead work and affect 19.1% (Mora et al., 2014). Elbow issues, or epicondylitis, affected 20.2% due to tool use (Mora et al., 2014). MSDs in Mexico rose 57.3% over 30 years (Clark et al., 2023). Obesity plays a role, with 40% of Hispanic men affected (Valdez et al., 2019).
In border areas like El Paso, women report 29.8% low back and 38.3% upper back pain from factory jobs (Harlow et al., 1999). Older patients walk more slowly due to leg pain (Quiben & Hazuda, 2015).
Common issues we handle:
- Low back pain: Top disability driver, tied to work and weight (Alva Staufert et al., 2021).
- Knee/foot arthritis: More in women, causing stiffness (Ciampi de Andrade et al., 2022).
- Rotator cuff: From arm overuse in construction (Mora et al., 2014).
- Epicondylitis: Elbow strain, common in 20% (Mora et al., 2014).
How El Paso Back Clinic® Helps with Integrative Care
Our clinic combines nurse practitioners (NPs) and chiropractic methods for culturally sensitive help. We focus on pain management and rehab to fit our community’s needs.
NPs at our clinic offer full check-ups that consider culture and history. They suggest diets rich in veggies and yoga for detox and pain relief (Jimenez, 2026a). We team up for whole-body care (Jimenez, 2026b).
Chiropractic adjustments realign the spine to ease nerve compression. For sitting-related back pain, we restore curves and strengthen the core (El Paso Back Pain Clinic, n.d.). Access to this care is key, though Hispanics use it less (Roseen, 2023).
Dr. Alexander Jimenez shares from his experience: Chronic back pain worsens with poor posture, but adjustments and exercises help (Jimenez, n.d.). For sciatica, decompression relieves pressure on nerves, which is common in laborers. Neuropathy gets therapy for tingling (Jimenez, n.d.). He uses functional medicine to tackle stress, diet, and job factors in our Mexican American patients.
We include mindfulness and natural remedies. Cultural factors, such as family support, help recovery, but delays worsen pain (Arthritis Foundation, n.d.). Our NPs create home plans (Pérez-Stable et al., 2003).
Rehab strengthens areas such as the legs and shoulders (Mora et al., 2014). It cuts frailty risks (National Institutes of Health, n.d.). For farmworkers, it reduces disability (Weigel et al., 2013).
Our care benefits:
- Cultural match: Understanding barriers like work migration (Harlow et al., 1999).
- Pain control: Non-surgical adjustments (Jimenez, 2026c).
- Strength building: Targeted exercises (Mora et al., 2014).
- Prevention: Nutrition against obesity (Valdez et al., 2019).
Why Choose El Paso Back Clinic® for Your Mobility Needs
In El Paso, with our diverse community, these issues are common but treatable. Our clinic specializes in wellness chiropractic to help you stay active. Contact us for a consultation with Dr. Jimenez and our team.
References
Arthritis Foundation. (n.d.). Arthritis in the Hispanic community. Arthritis.org.
El Paso Back Pain Clinic. (n.d.). El Paso back pain clinic. ElPasoChiropractorBlog.com.
Jimenez, A. (n.d.). Injury specialists. DrAlexJimenez.com.
Jimenez, A. (2026a). Nurse practitioners and integrative chiropractic detox. ChiroMed.com.
Jimenez, A. (2026b). Relieving back pain from prolonged sitting. ChiroMed.com.
Jimenez, A. (2026c). Advancements in sciatica treatment in 2026. ChiroMed.com.
Pérez-Stable, E. J., et al. (2003). Pain in Hispanic/Latino patients. PubMed.

Beating Back Pain from Long Desk Hours at Work
Dr. Alex Jimenez at El Paso Back Clinic®: Beating Back Pain from Long Desk Hours
If your back pain gets worse the longer you sit at your desk, you are not alone. Many people in El Paso face this issue due to long hours spent in sedentary jobs. Sitting for extended periods can put pressure on the spine, tighten muscles, and reduce blood flow, leading to stiffness, aches, and, in some cases, chronic problems (Colorado Pain Care, n.d.). The positive news is that you can take simple steps to reduce the pain and prevent it from worsening. At El Paso Back Clinic® in El Paso, TX, the wellness chiropractic care team, led by Dr. Alex Jimenez, DC, APRN, FNP-BC, focuses on helping people just like you find natural, long-term relief through personalized plans.
Prolonged sitting stresses the lower back by increasing disc pressure by up to 90% compared to standing. It flattens the spine’s natural curve, strains muscles, and creates imbalances (Colorado Pain Care, n.d.). Slouching or leaning forward adds extra load to the neck and upper back. Over time, this can lead to tight hips, weak core muscles, and ongoing discomfort that affects daily life.
At El Paso Back Clinic®, our experts understand these issues caused by sedentary work. They use a holistic approach that combines chiropractic adjustments, functional medicine, and rehab to address root causes like poor posture and muscle imbalances from desk jobs (Jimenez, n.d.-a).
Here are practical changes to start today:
- Move often: Get up every 30 minutes to stand, walk, or shift positions. Short 1-2 minute breaks improve circulation and ease tension (Huntsville Hospital Health System, n.d.; Sydney West Physio, n.d.).
- Use regular breaks: Set a timer for quick walks to get water or to stretch. This habit prevents stiffness from building up throughout the day.
- Add dynamic movement: While sitting, shift weight, uncross legs periodically, or use a footrest to change angles. These small actions keep the spine mobile (Colorado Pain Care, n.d.).
A proper ergonomic setup supports optimal posture and reduces strain.
Follow these key tips:
- Set your chair so that your feet are flat on the floor, your knees are at 90 degrees, and your hips are level with or above your knees.
- Add lumbar support (a small pillow or rolled towel works) to maintain the lower back’s curve.
- Place your screen at eye level to avoid looking down or up too much.
- Keep the keyboard and mouse close so elbows bend at 90 degrees and shoulders stay relaxed.
- Avoid crossing legs for long, as it can tilt the pelvis (Senara Chiropractic & Med Spa, n.d.; Huntsville Hospital Health System, n.d.).
Consider alternating between sitting and standing with a standing desk. Even partial standing reduces spinal pressure.
Stretches help loosen tight spots from sitting, such as the hips, shoulders, and neck.
Try these simple ones:
- Hip flexor stretch: Kneel on one knee, gently push hips forward, and hold 20-30 seconds per side.
- Chest and shoulder opener: Clasp hands behind your back or use a wall to stretch forward.
- Neck tilts: Slowly tilt the head side to side or forward/back; hold for 10-15 seconds.
- Upper back extension: Hands behind head, gently arch upper back (Sydney West Physio, n.d.).
Do them hourly or during breaks for better flexibility.
Strengthening the core supports the spine and improves posture long-term.
Include these:
- Planks: Hold forearm plank 20-30 seconds.
- Cat-camel: On hands and knees, arch and round back slowly.
- Bridges: Lie back, lift hips while squeezing glutes.
- Walking or gentle yoga: Build overall strength (Huntsville Hospital Health System, n.d.; Sydney West Physio, n.d.).
Aim for 20-30 minutes of activity most days.
For lasting relief, professional care targets alignment, mobility, and personalized fixes. At El Paso Back Clinic®, Dr. Alex Jimenez leads a team offering integrated chiropractic care. This includes spinal adjustments to correct misalignments, non-surgical spinal decompression for disc relief, acupuncture, functional medicine for nutrition and stress, and rehab exercises tailored to desk-related issues.
Dr. Jimenez, with dual expertise as a chiropractor and nurse practitioner, emphasizes posture correction, mobility training, and the prevention of sedentary pain through evidence-based methods. The clinic helps restore function without drugs or surgery, focusing on root causes like imbalances from prolonged sitting (Jimenez, n.d.-a; Jimenez, n.d.-b).
Other options in El Paso exist, but El Paso Back Clinic® stands out for its comprehensive wellness approach, advanced diagnostics, and patient-centered plans that go beyond basic adjustments.
If pain includes numbness, tingling, or weakness in the legs, or persists despite changes, seek evaluation to rule out serious conditions (University of Maryland Medical System, n.d.).
Start small: improve movement, setup, and stretches. If needed, contact El Paso Back Clinic® for expert help. Many in El Paso regain comfort and stay active with this care.
References
Colorado Pain Care. (n.d.). Prolonged sitting & back pain. https://coloradopaincare.com/prolonged-sitting-back-pain/
Huntsville Hospital Health System. (n.d.). 7 ways to improve your spine health while working a desk job. https://hh.health/7-ways-to-improve-your-spine-health-while-working-a-desk-job/
Jimenez, A. (n.d.-a). Injury specialists. https://dralexjimenez.com/ (also associated with El Paso Back Clinic® at https://elpasobackclinic.com/)
Jimenez, A. (n.d.-b). Dr. Alexander Jimenez DC, APRN, FNP-BC, IFMCP, CFMP, ATN. LinkedIn. https://www.linkedin.com/in/dralexjimenez/
Senara Chiropractic & Med Spa. (n.d.). Surviving your desk job: Tips to avoid back pain. https://www.experiencesenara.com/physical-therapy-peoria/surviving-your-desk-job-tips-to-avoid-back-pain/
Sydney West Physio. (n.d.). 5 effective tips to reduce back pain from your office job. https://sydneywestphysio.com.au/physiotherapy/5-effective-tips-to-reduce-back-pain-from-your-office-job/
University of Maryland Medical System. (n.d.). Signs & symptoms. https://www.umms.org/health-services/spine/signs-symptoms

Make Your Health Goals Stick in 2026 with Team Care
Make Your Health Goals Stick in 2026: How El Paso Back Clinic’s Integrative Team Supports Real Change

The patient uses a weight machine for injury rehabilitation under the supervision of a doctor of chiropractic and a nurse practitioner.
Most people don’t fail at New Year’s goals because they “don’t want it enough.” They fail because life gets busy, pain flares up, energy crashes, and stress piles on. When your body hurts or feels stiff, even simple plans—like walking more, lifting weights, or sleeping better—can feel harder than they should.
At El Paso Back Clinic, the goal is to make health changes easier to achieve and maintain through a team-based, integrative approach. That means bringing together the strengths of chiropractic care (movement, structure, mobility, and recovery) with the strengths of nurse practitioner care and wellness coaching (nutrition, sleep, stress, and whole-body support). The clinic describes this as a blend of injury care, wellness strategies, mobility programs, and integrated medicine designed to improve function and quality of life. El Paso Back Clinic® • 915-850-0900+2El Paso Back Clinic® • 915-850-0900+2
This kind of care supports common goals like:
-
increasing fitness and mobility
-
managing pain so you can stay active
-
improving energy and sleep
-
lowering stress and improving your stress response
-
building habits that last longer than a few weeks
El Paso Back Clinic’s content and services focus on restoring movement and supporting whole-body wellness—not just “cracking backs.” El Paso Back Clinic® • 915-850-0900+2El Paso Back Clinic® • 915-850-0900+2
What “Integrative” Means at El Paso Back Clinic
“Integrative care” means your plan isn’t built around only one angle. Instead, it connects the pieces that usually get separated:
-
How you move
-
How you recover
-
How you eat
-
How you sleep
-
How you manage stress
-
How do you build habits that fit your real life
El Paso Back Clinic describes integrative chiropractic benefits as going beyond traditional adjustments by combining care approaches that support overall wellness and function. El Paso Back Clinic® • 915-850-0900
Why this matters for resolutions
Many resolutions are difficult to maintain because the plans ignore the real barriers. For example:
-
You want to exercise more—but your back pain spikes.
-
You want to lose weight—but your sleep is poor and your stress is high.
-
You want more energy—but your nutrition is inconsistent, and you’re not recovering.
An integrative plan helps because it aims to reduce the friction that makes healthy habits feel impossible.
The Team Approach: Chiropractor + Nurse Practitioner Mindset
Many clinics talk about how chiropractic care supports goals such as mobility, stress reduction, better sleep, and improved performance. gotcore.net+2Freedom Chiropractic+2
At El Paso Back Clinic, that support is often strongest when chiropractic care is paired with whole-person planning.
The chiropractor’s lane: move better with less strain
Chiropractic care commonly focuses on:
-
joint motion and spinal mechanics
-
posture and movement habits
-
mobility and flexibility
-
recovery support when you start working out again
-
helping reduce strain patterns that keep pain looping
The descriptions of services at El Paso Back Clinic emphasize spine-focused care and the restoration of function for back and musculoskeletal concerns. El Paso Back Clinic® • 915-850-0900+1
The NP/wellness lane: build a plan that supports your body from the inside out
A nurse practitioner and wellness-minded team approach can support:
-
nutrition planning that fits your schedule
-
sleep improvement routines
-
stress management strategies
-
health screening and medical risk review when appropriate
-
coaching that makes change more realistic to sustain
This matches the habit-focused guidance many health organizations recommend: set realistic goals, build routines, and avoid extreme “all at once” changes. Prism Health North Texas
Dr. Alexander Jimenez’s clinical observations (El Paso context)
Dr. Alexander Jimenez (DC, APRN, FNP-BC) frequently describes a dual-scope approach that connects biomechanics (how you move) with broader health planning (nutrition, functional assessments, and recovery strategies). His published clinic content also highlights the use of assessments and, when needed, imaging and integrated care planning to support recovery and function. LinkedIn+3El Paso, TX Doctor Of Chiropractic+3El Paso, TX Doctor Of Chiropractic+3
Why Resolutions Often Fail (And How an Integrative Plan Fixes That)
Here are common “resolution killers” and what a coordinated plan can do differently:
-
Too much, too fast → Start with small steps and progress safely. Prism Health North Texas+1
-
Pain blocks movement → Address mobility limits and movement mechanics so activity feels doable. National Spine & Pain Centers+1
-
Low energy → Improve sleep, nutrition consistency, and recovery structure. gotcore.net+1
-
Stress overload → Add stress skills and routines that calm the system and support follow-through. NIH News in Health+1
-
No accountability → Regular check-ins and plan adjustments keep you from quitting after a setback. drmmalone.com+1
A key idea in habit-based care is that early wins create a “positive feedback loop”—you feel better, so it becomes easier to keep going. drmmalone.com
1) Increase Fitness and Mobility (Without Getting Injured)
If your goal is to work out more, the priority is often moving well enough to train consistently.
Many chiropractic resources emphasize mobility, flexibility, and injury prevention as people increase activity at the start of the year. 5280 Balanced Health Center+2Freedom Chiropractic+2
El Paso Back Clinic also emphasizes flexibility, mobility, and agility programs to improve ability and quality of life. El Paso Back Clinic® • 915-850-0900
A simple evidence-based target
For general health, adults are commonly advised to aim for 150 minutes of moderate activity per week, plus 2 days of muscle-strengthening activities. CDC+1
That can be split into smaller chunks—like 30 minutes, 5 days a week.
What the integrative plan can look like
-
Assess mobility limits (hips, spine, shoulders) and address movement friction
-
Build a realistic weekly schedule
-
Progress intensity slowly, so you don’t crash or flare
Easy “start small” movement ideas:
-
10–20 minute walk after meals
-
2 strength sessions per week (basic full-body)
-
5-minute mobility routine daily
Progression rules that keep people consistent:
-
Add time before you add intensity
-
Keep at least 1–2 recovery days weekly
-
Measure consistency, not perfection
2) Manage Pain So You Can Stay Active
Pain goals often work better when you focus on function—not “zero pain tomorrow.” A pain-focused plan might aim to reduce flare-ups and increase what you can do safely. National Spine & Pain Centers
El Paso Back Clinic positions its care around helping people with frustrating injuries and chronic pain syndromes improve mobility and function. El Paso Back Clinic® • 915-850-0900
Practical pain goals that tend to stick
-
“Walk 20 minutes, 4 days/week without a flare.”
-
“Lift twice/week with pain staying under a 3–4/10.”
-
“Sleep through the night most nights.”
How integrative care helps pain goals
-
Chiropractic care can focus on mechanics, mobility, and movement habits that contribute to repeated strain. El Paso Back Clinic® • 915-850-0900+1
-
NP-style wellness support can focus on sleep, stress, consistency in nutrition, and pacing habits that support recovery. Prism Health North Texas+1
Helpful pacing ideas (simple but powerful):
-
Use shorter workouts more often
-
Stop just before your “flare threshold”
-
Build capacity gradually rather than “weekend warrior” bursts
3) Boost Energy the Smart Way
Energy is not just “motivation.” If you’re tired, your plan needs better recovery.
Many chiropractic sources link better sleep and reduced tension with feeling more capable and consistent over time. gotcore.net+1
El Paso Back Clinic also describes a wellness-focused approach aimed at improving energy, sleep, and overall function. El Paso Back Clinic® • 915-850-0900
Common energy drains
-
inconsistent sleep schedule
-
high stress with no recovery routine
-
skipping meals, then crashing
-
pushing too hard without rest
Energy supports that don’t require perfection:
-
consistent bedtime “window” (same 60–90 minutes nightly)
-
protein-forward breakfast 3–5 days/week
-
short walks for circulation and stress relief
-
mobility routine before bed
4) “Boost Immunity” by Strengthening the Basics
It’s common to hear people say they want to “boost immunity.” A safe and practical way to think about this is:
You can support overall wellness by improving sleep, physical activity, and stress management—foundations that matter for health.
-
Regular physical activity is widely recommended for health. CDC
-
Mindfulness-based approaches have evidence supporting their effectiveness for stress, sleep, and pain management. NIH News in Health
So instead of chasing extreme detoxes or perfect diets, an integrative plan often focuses on steady basics:
-
sleep routine
-
movement most days
-
nutrition consistency
-
stress skills
That’s the kind of “quiet consistency” that makes resolutions last.
5) Lower Stress and Improve Stress Response
Stress shows up in the body: tight shoulders, headaches, jaw tension, shallow breathing, gut tension, and poor sleep.
Mindfulness-based treatments have evidence supporting reduced anxiety/depression symptoms and improved sleep, and may help people cope with pain. NIH News in Health
Many chiropractic sources also connect care with stress reduction and better sleep as part of overall wellness. gotcore.net+1
Simple “stress reset” tools (easy to repeat)
-
4–6 slow breaths with longer exhales
-
5–10 minute walk outdoors
-
Gentle mobility work for neck/hips
-
Short mindfulness practice (1–3 minutes) NIH News in Health
A key point: stress plans work best when they are small enough to do daily. It’s important to avoid making big, dramatic changes once a week.
Habit Design: The Real Key to Long-Lasting Change
If you only rely on motivation, you’ll struggle. If you build habits, you’ll progress even during busy weeks.
Health habit coaching often emphasizes:
-
realistic goals
-
repeatable routines
-
tracking small wins
-
adjusting instead of quitting Prism Health North Texas+1
A simple habit framework that works
-
Pick one main goal (fitness OR pain, energy, OR stress)
-
Add two support habits
-
Track consistency weekly
-
Adjust every 2–4 weeks
Examples of “support habits”:
-
protein at breakfast
-
20-minute walk 4x/week
-
5 minutes of mobility daily
-
bedtime routine 5 nights/week
A Simple 4-Week Plan (El Paso Back Clinic Style: Practical, Not Perfect)
This is a general example you can personalize with your provider team.
Week 1: Reduce friction
-
Identify mobility limits and pain triggers
-
Set one realistic activity goal
-
Begin a simple nutrition and sleep routine
Week 2: Build consistency
-
Add a second strength or mobility day
-
Keep intensity moderate
-
Track sleep and energy patterns
Week 3: Progress carefully
-
Increase walking time or training volume slightly
-
Add a stress routine you can repeat
-
Adjust the plan based on how your body responds
Week 4: Lock in your system
-
Keep what’s working
-
Simplify what isn’t
-
Create a “busy week version,” so you don’t fall off
This approach fits the clinic’s overall theme of improving function through mobility, recovery, and whole-person planning. El Paso Back Clinic® • 915-850-0900+1
When to Get Checked Right Away
If you have severe or unusual symptoms, don’t “push through.” Seek urgent medical care for red flags like:
-
chest pain, severe shortness of breath, fainting
-
sudden weakness, facial droop, confusion
-
loss of bowel/bladder control
-
fever with severe spine pain
-
major trauma with worsening symptoms
Bottom Line: Your Best Results Come From a Whole Plan
At El Paso Back Clinic, an integrative model supports real-life resolutions by combining:
-
mobility and movement support (so activity is easier) El Paso Back Clinic® • 915-850-0900+1
-
wellness and lifestyle coaching (so change is sustainable) Prism Health North Texas
-
stress and sleep support (so recovery improves) NIH News in Health
-
a coordinated approach reflected in Dr. Jimenez’s dual-scope clinical framework (structure + whole-person care) El Paso, TX Doctor Of Chiropractic+2El Paso, TX Doctor Of Chiropractic+2
You don’t need a perfect year. You need a plan that helps you move better, recover better, and repeat the basics long enough to see real change.
References
Centers for Disease Control and Prevention. (2025, December 4). Adding physical activity as an adult. CDC. CDC
Centers for Disease Control and Prevention. (2023, December 20). Adult activity: An overview. CDC. CDC
El Paso Back Clinic. (n.d.). Blog | El Paso Back Clinic. El Paso Back Clinic® • 915-850-0900
El Paso Back Clinic. (n.d.). About us. El Paso Back Clinic® • 915-850-0900
El Paso Back Clinic. (n.d.). Spine care. El Paso Back Clinic® • 915-850-0900
El Paso Back Clinic. (2019). Back pain specialist | El Paso, TX. El Paso Back Clinic® • 915-850-0900
El Paso Back Clinic. (2025). Integrative chiropractic care benefits in El Paso. El Paso Back Clinic® • 915-850-0900
Freedom Chiropractic. (2024, December 15). How chiropractic care supports your New Year’s resolutions in 2025. Freedom Chiropractic
Grovetown Chiropractic. (2023, May 17). Four New Year’s resolutions a chiropractor can help with. Grovetown Chiropractic
Malone, M. (2025). Why health habits beat resolutions—and how chiropractic helps. drmmalone.com
National Institutes of Health. (2021, June). Mindfulness for your health. NIH News in Health. NIH News in Health
Prism Health North Texas. (2025, December 9). Health-related 2026 New Year’s resolutions that actually stick. Prism Health North Texas
TreatingPain.com. (2023, December 4). Practical New Year’s resolutions to manage pain. National Spine & Pain Centers
River of Life Chiropractic. (2025, January 9). New year, new you: How chiropractic care supports your health goals in 2025. Website
CORE Health Centers. (2024, December 31). 5 benefits of chiropractic care for the new year. gotcore.net
5280 Balanced Health Center. (2025). Why chiropractic care should be part of your New Year’s resolutions. 5280 Balanced Health Center
Jimenez, A. (n.d.). Dr. Alex Jimenez, chiropractor and injury recovery. DrAlexJimenez.com. El Paso, TX Doctor Of Chiropractic
Jimenez, A. (n.d.). Safe chiropractic care in El Paso: What to expect. DrAlexJimenez.com. El Paso, TX Doctor Of Chiropractic
Jimenez, A. (n.d.). Personalized chiropractic nutrition counseling strategies. DrAlexJimenez.com. El Paso, TX Doctor Of Chiropractic
Jimenez, A. (n.d.). Dr. Alex Jimenez (website). El Paso, TX Doctor Of Chiropractic
Jimenez, A. (n.d.). Dr. Alexander Jimenez LinkedIn profile. LinkedIn

Faster Recovery After Spine Surgery Strategies
Faster Recovery After Spine Surgery: Enhanced Surgical Recovery (ESR) Programs at El Paso Back Clinic® in El Paso, TX
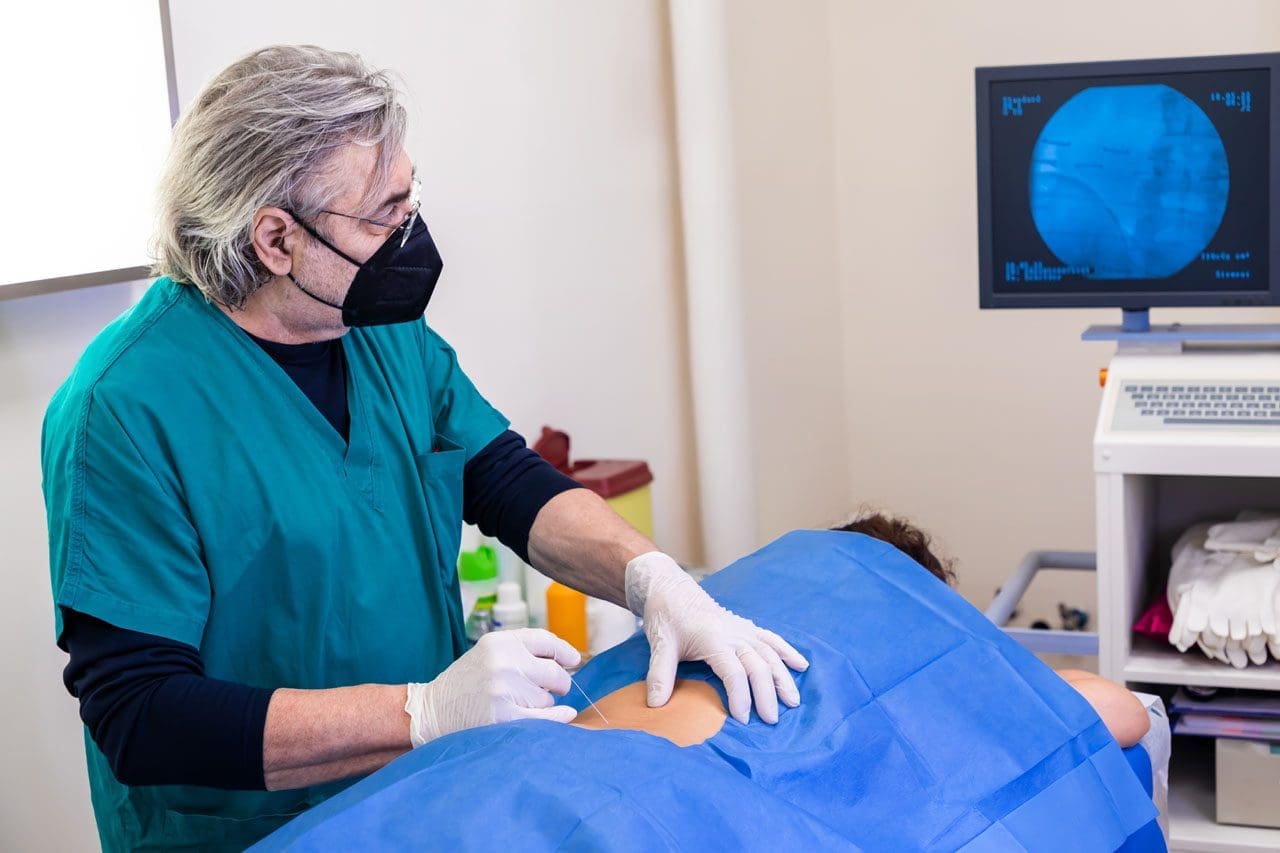
The doctor administers a local anesthetic into the patient’s affected area, using ultrasound to visualize the spine’s anatomical components.
Spine surgery can help treat serious back problems, such as pain from injuries, disc issues, or aging. At El Paso Back Clinic® in El Paso, TX, we focus on helping patients recover faster and more safely through modern methods. Enhanced Surgical Recovery (ESR), also called Enhanced Recovery After Surgery (ERAS), is a team-based plan that reduces the need for strong pain medications, shortens hospital stays, and lowers the risk of readmission. Led by Dr. Alexander Jimenez, DC, APRN, FNP-BC, our clinic combines chiropractic care, nurse practitioner expertise, and new tools to support healing. This article explains the main parts of ESR for spine surgery, how it cuts opioid use, shortens hospital stays, and reduces readmissions. We also cover the big roles of integrative chiropractic care and nurse practitioners, plus exciting new tech like virtual reality (VR) for building strength after surgery.
Many people in El Paso face back pain from work, accidents, or daily life. Surgery may be necessary, but traditional methods can make recovery challenging. ESR improves this process by planning care before, during, and after the operation. It uses simple steps, such as teaching patients, eating better, and moving early. Studies show these measures can cut opioid use a lot and help people go home sooner (Dagal et al., 2023). At El Paso Back Clinic®, we work with surgeons to add non-drug options for even better results.
What Is Enhanced Surgical Recovery (ESR)?
ESR is a proven plan to make surgery recovery easier and quicker. It started in other surgeries, but now helps a lot with spine operations, such as fusions or disc repairs. The idea is to lower body stress and speed natural healing. Instead of staying in bed and taking many pain pills, patients move soon and use gentler pain control.
Key parts of ESR include:
- Team Approach — Doctors, nurses, chiropractors, and therapists all work together.
- Step-by-Step Care — Planning starts before surgery and continues at home.
- Personal Plans — Care fits each person’s health needs.
Research shows ESR helps with many spine issues, from small fixes to big ones (Zaed et al., 2023). Reviews find that most programs use around 12 key steps, such as better pain management and early walking (Berk et al., 2025).
Main Components of ESR for Spine Surgery
ESR has steps before, during, and after surgery to make things smoother.
Before Surgery (Pre-Op)
Getting ready early helps avoid problems.
- Teaching Patients: Learn what to expect, how to manage pain, and why moving matters. This lowers worry and helps follow the plan (Zaed et al., 2023).
- Better Nutrition: Check for low energy or anemia. Eat protein and carbs to build strength. Nutritious food helps healing (Soffin et al., 2022).
- Pain Prep: Start gentle meds like acetaminophen. Quit smoking to lower risks (American Association of Nurse Anesthesiology, n.d.).
- Prehab Exercises: Build strength with walks or stretches.
These make surgery safer.
During Surgery (Intra-Op)
The team uses ways to protect the body.
- Better Anesthesia: Short drugs to wake up fast. Add non-opioid options (Dagal et al., 2023).
- Careful Fluids: Just the right amount to avoid issues.
- Small Cuts: Less muscle damage for quicker recovery (Dietz et al., 2019).
- Pain Blocks: Numb the area for hours after.
Patients feel better right away.
After Surgery (Post-Op)
Focus on rapid healing.
- Early Walking: Get up soon and walk daily (Zaed et al., 2023).
- Mixed Pain Control: Use non-opioids, ice, and movement.
- Quick Eating: Start foods and drinks early.
- Checks for Safety: Watch for clots or other issues.
These steps lower risks.
How ESR Reduces Opioid Use
Strong pain drugs like opioids help, but can lead to problems like addiction. ESR cuts its use by at least half (Dagal et al., 2023). At El Paso Back Clinic®, we add chiropractic methods for even less need.
- Mixed Pain Options: Non-opioids first, like NSAIDs and nerve meds. Some programs use almost no IV opioids (HCA Healthcare, n.d.).
- Teaching Non-Drug Ways: Ice, breathing, and adjustments.
- Blocks and Early Move: Numb areas and walk to ease pain.
In fusions, opioids dropped considerably without worse pain (Dagal et al., 2023). This helps avoid side effects and promotes natural healing.
Shortening Hospital Stays with ESR
Long hospital time raises costs and risks. ESR cuts stay by 1-2 days (HCA Healthcare Today, 2022).
- Early Movement: Prevents issues and builds strength.
- Fast Nutrition: Energy for recovery.
- Good Pain Control: Less bedtime.
- Team Reviews: Go home when ready.
One example shows noticeable shortened stays (Dagal et al., 2023). Patients heal better at home.
Lowering Readmission Rates
Going back to the hospital is tough. ESR lowers this risk (HCA Healthcare Today, 2022).
- Home Care Teaching: Know warning signs.
- Follow-Ups: Calls from our team at El Paso Back Clinic®.
- Fewer Problems: Better prep means fewer infections.
- Full Care: Controls swelling early.
Fewer complications overall (Berk et al., 2025).
Integrative Chiropractic Care at El Paso Back Clinic®
Chiropractic care fits perfectly with ESR. At our clinic, Dr. Jimenez uses hands-on adjustments to align and relieve symptoms.
- Before Surgery: Improve posture and movement.
- Pain Without Drugs: Soft tissue work eases tension.
- After Surgery: Reduce scar tissue and build mobility (New York City Spine, n.d.).
- Nerve Help: Better signals for less pain.
We complement therapy for smoother recovery (Active Health Center, n.d.).
Role of Nurse Practitioners
Nurse practitioners (NPs) like Dr. Jimenez coordinate care.
- Team Links: Connect everyone.
- Teaching and Meds: Focus on safe, non-opioid options.
- Tracking Progress: Adjust plans.
NPs help stick to ESR paths (American Association of Nurse Anesthesiology, n.d.).
New Tech: Virtual Reality (VR) for Recovery
VR uses games and guides to make rehab more enjoyable. It helps spine patients build strength.
- Fun Exercises: Improves engagement and movement.
- Less Pain Feel: Distraction helps.
- Strength Gains: Tailored for muscles and focus.
- Home Options: Practice alone.
Recent studies show VR speeds recovery after spine issues, like in cervical cases or general neurorehab (Bolton et al., 2025; various 2025 trials).
Insights from Dr. Alexander Jimenez at El Paso Back Clinic®
Dr. Alexander Jimenez, DC, APRN, FNP-BC, leads El Paso Back Clinic® with dual expertise in chiropractic and nursing. He uses team care for pain management and rehab after injuries or surgery. His plans include adjustments, nutrition, and integrative methods for better mobility without heavy drugs. He stresses whole-body healing for lasting results (Dr. Alex Jimenez, n.d.; LinkedIn, n.d.).
Conclusion
ESR programs accelerate spine surgery recovery and make it safer. With education, nutrition, movement, and team support, they reduce opioids, shorten stays, and lower readmissions. At El Paso Back Clinic® in El Paso, TX, we add chiropractic care and NP guidance for full support. New VR tech adds exciting ways to build strength. If facing spine surgery, ask about ESR and our integrative options. Contact us at 915-850-0900 for help.
References
Active Health Center. (n.d.). Rehabilitation after surgery: Integrating chiropractic care into recovery. https://activehealthcenter.com/rehabilitation-after-surgery-integrating-chiropractic-care-into-recovery/
American Association of Nurse Anesthesiology. (n.d.). Enhanced recovery after surgery. https://www.aana.com/practice/clinical-practice/clinical-practice-resources/enhanced-recovery-after-surgery/
Berk, M., et al. (2025). Enhanced recovery after surgery (ERAS) in spine surgery: A systematic review and meta-analysis. https://pmc.ncbi.nlm.nih.gov/articles/PMC12592135/
Bolton, W.S., et al. (2025). Recovr reality – Recover after injury or surgery to the brain and spinal cord with virtual Reality: ideal stage 2a clinical feasibility study. https://jneuroengrehab.biomedcentral.com/articles/10.1186/s12984-024-01499-3
Dagal, A., et al. (2023). Adoption of enhanced surgical recovery (ESR) protocol for lumbar fusion decreases in-hospital postoperative opioid consumption. https://pmc.ncbi.nlm.nih.gov/articles/PMC10189339/
Dietz, N., et al. (2019). Enhanced recovery after surgery (ERAS) protocols: Time to change practice?. https://www.medrxiv.org/content/10.1101/2020.08.16.20175943v1.full
Dr. Alex Jimenez. (n.d.). El Paso, TX, doctor of chiropractic. https://dralexjimenez.com/
HCA Healthcare. (n.d.). With ESR, our patients report…. https://www.hcadam.com/api/public/content/f42a4095a6f9451baa991b5a56cad568?v=4786eda4&download=true
HCA Healthcare Today. (2022). HCA Healthcare’s innovative approach to surgical recovery. https://hcahealthcaretoday.com/2022/12/13/hca-healthcares-innovative-approach-to-surgical-recovery-promotes-better-outcomes-decreased-opioid-usage-and-faster-recovery-times-for-patients/
LinkedIn. (n.d.). Dr. Alexander Jimenez, DC, APRN, FNP-BC. https://www.linkedin.com/in/dralexjimenez/
New York City Spine. (n.d.). How a chiropractor can aid spinal fusion recovery. https://newyorkcityspine.com/how-a-chiropractor-can-aid-spinal-fusion-recovery/
Soffin, E. M., et al. (2022). Enhanced recovery after surgery (ERAS) protocol in spine surgery. https://pmc.ncbi.nlm.nih.gov/articles/PMC9293758/
Zaed, I., et al. (2023). Enhanced recovery after surgery (ERAS) protocols for spine surgery – review of literature. https://pmc.ncbi.nlm.nih.gov/articles/PMC10156499/

Telemedicine Sciatica Management: Expert Care Online
How Telemedicine Can Assist in the Management of Sciatica (with Integrative Chiropractic Care)
A man at home consults a chiropractor via telemedicine for back pain and sciatica.
Sciatica can make even simple tasks—like getting out of bed, sitting at a desk, or driving—feel almost impossible. When pain shoots down your leg or feels like burning, stabbing, or tingling, the idea of driving across town to sit in a waiting room can be overwhelming.
Telemedicine offers a way to get expert help for sciatica without leaving home. Telemedicine can significantly improve the quality of life for many individuals experiencing limited mobility or frequent flare-ups of pain. Spine specialists and integrative chiropractic teams now use secure video visits to evaluate symptoms, design treatment plans, and follow patients through recovery. UT Southwestern Medical Center+1
Dr. Alexander Jimenez, DC, APRN, FNP-BC, is a dual-licensed chiropractor and nurse practitioner in El Paso, Texas. His integrative model combines medical decision-making (such as imaging and prescriptions) with chiropractic and functional medicine. This blended approach fits perfectly with telemedicine because it allows him to assess nerve pain, guide movement, and adjust treatment plans over time—even when the patient is at home. El Paso, TX Doctor Of Chiropractic
What Is Sciatica?
Sciatica is not a disease by itself. It is a pattern of symptoms caused by irritation or compression of the sciatic nerve. This nerve starts in the lower back, runs through the hips and buttocks, and travels down each leg.
Common symptoms include:
-
Sharp or burning pain in the lower back, buttocks, and legs
-
Numbness, tingling, or “pins and needles” in the leg or foot
-
Weakness when trying to stand, walk, or lift the leg
-
Pain that worsens with sitting, coughing, or bending
Sciatica is usually caused by:
-
Herniated or bulging discs pressing on a nerve root
-
Spinal stenosis (narrowing of the spinal canal)
-
Degenerative disc disease
-
Muscle or joint dysfunction in the pelvis and lower back
-
Less commonly, tumors, infections, or serious conditions
Because sciatica can have many causes, proper evaluation and treatment planning are very important—this is where telemedicine can help you start sooner and stay on track.
What Is Telemedicine and How Does It Work for Back and Nerve Pain?
Telemedicine (also called telehealth) is health care delivered via secure video or phone rather than an in-person visit. You use a smartphone, tablet, or computer to speak with your provider, similar to a video call with family or friends.
Clinics that treat spine and nerve problems have made telemedicine a core part of their care model. They use it for first visits, follow-ups, second opinions, and surgical planning, especially for conditions like back pain, neck pain, and sciatica. UT Southwestern Medical Center+1
During a typical telemedicine visit for sciatica, your provider can:
-
Ask detailed questions about your pain pattern
-
Watch how you move on camera
-
Guide simple movement and strength tests
-
Review MRI, X-ray, or CT results
-
Explain treatment options, including chiropractic, physical therapy, injections, or surgery if needed
Many clinics report that they can accurately diagnose spine issues through video visits and that most telemedicine-based surgical plans do not require major changes after in-person exams. UT Southwestern Medical Center
Why Telemedicine Is Especially Helpful for Sciatica
People with sciatica often have trouble sitting, driving, or walking long distances. Telemedicine meets them where they are—literally.
Key benefits for sciatica patients
-
Less travel and less pain getting to care
-
No long car rides or sitting in waiting rooms
-
Easier for patients who have mobility issues or rely on others for transportation Southeast Texas Spine+1
-
-
Faster access to evaluation and treatment
-
Many clinics can schedule telemedicine visits sooner than in-person visits
-
You can start treatment earlier instead of waiting weeks to be seen
-
-
Better continuity of care
-
Telemedicine makes it easier to attend follow-ups, especially during long recovery plans
-
Providers can adjust medications, exercises, and activity limits in real time Southeast Texas Spine+1
-
-
Home-based evaluation of your real environment
-
Your provider can see your work setup, couch, bed, or home office
-
They can give specific advice on posture, ergonomics, and movement at home tigardchiropracticautoinjury.com+1
-
For many patients, this means less time in cars and clinics and more time actually healing.
How Telemedicine Helps Diagnose Sciatica
Telemedicine does not replace all in-person care, but it is surprisingly powerful for diagnostic work, especially when combined with imaging.
A telemedicine evaluation for sciatica often includes:
-
Detailed history
-
When the pain started
-
Where it travels (buttock, thigh, calf, foot)
-
What makes it better or worse (sitting, walking, bending)
-
Past injuries, surgeries, or chronic conditions Southeast Texas Spine+1
-
-
Guided home exam
-
Simple range-of-motion tests
-
Straight-leg raise or seated leg raise while on camera
-
Heel and toe walking to assess nerve strength
-
Balance and gait observation
-
-
Imaging and tests
-
Your nurse practitioner or physician can order MRI, X-rays, or CT scans when needed
-
They may also recommend nerve tests (EMG/NCS) through in-person referrals
-
Spine centers and orthopedic clinics report that telemedicine visits can help determine when conservative care is sufficient and when urgent in-person care or surgery is needed. UT Southwestern Medical Center+1
Integrative Chiropractic Telemedicine for Sciatica
Integrative chiropractic telemedicine combines:
-
Medical care—history, diagnosis, imaging orders, prescriptions, and referrals
-
Chiropractic care—movement analysis, spinal and pelvic mechanics, and guided home-based therapies
Dr. Jimenez’s dual-scope role as a chiropractor and nurse practitioner is a strong example of this model. In his practice, he uses telemedicine to:
-
Review MRI and other imaging results with patients
-
Coordinate conservative care (chiropractic, physical therapy, massage, acupuncture, and functional medicine)
-
Monitor nerve symptoms and red flags that require fast in-person intervention
-
Work with attorneys and adjusters in personal-injury cases while keeping patient care at the center El Paso, TX Doctor Of Chiropractic
What an integrative telemedicine visit may look like
During a virtual visit with an integrative chiropractor and NP:
-
The NP side of the provider:
-
Reviews your medical history and medications
-
Screens for red flags (such as severe weakness, fever, or loss of bladder/bowel control)
-
Orders imaging when needed
-
Manages medications (anti-inflammatories, muscle relaxers, short-term pain medications if appropriate) Everlywell+1
-
-
The chiropractic side of the provider:
-
Analyzes your posture and movement on camera
-
Looks for patterns of dysfunction in the lower back, pelvis, and hips
-
Guides you through gentle tests and movements
-
Designs a home exercise and stretching plan
-
Educates you about ergonomics, sleep positions, and movement habits
-
Even without hands-on adjustments, chiropractic expertise is used to understand mechanics and guide safe self-care at home. Evolve Chiropractic+2HealthCentral+2
Telemedicine and Medication Management for Sciatica
Telemedicine is also useful for medication oversight and pain management. Virtual pain management services can:
-
Review current medications and supplements
-
Start or adjust anti-inflammatory drugs, muscle relaxers, or nerve pain medications when appropriate
-
Help taper short-term medications to avoid long-term dependence
-
Coordinate with other therapies like physical therapy and chiropractic care Everlywell+1
This is important because the goal is not just to reduce pain for a few days but to manage it safely while addressing the underlying cause.
Guided Home Exercises and Self-Care for Sciatica via Telemedicine
A large part of sciatica management involves what you do every day at home. Telemedicine allows your integrative provider to coach you in real time.
Types of exercises a provider may guide over video
Always follow your own provider’s instructions. The list below is for education, not a personal prescription.
-
Gentle nerve glides and stretches
-
Seated or lying hamstring stretches
-
Gentle sciatic nerve gliding movements
-
Piriformis stretches (for deep hip muscles) HealthCentral+1
-
-
Core and hip stability
-
Pelvic tilts
-
Bridge exercises
-
Clamshells for hip stabilizers
-
-
Posture and movement training
-
How to bend and lift with less spinal strain
-
How to change positions often instead of sitting for hours
-
Strategies for standing desks and micro-breaks for office workers tigardchiropracticautoinjury.com+2tigardchiropracticautoinjury.com+2
-
An integrative chiropractor, such as Dr. Jimenez, will often blend chiropractic reasoning (how joints and muscles are moving) with physical therapy-style exercise progressions to build strength and reduce nerve irritation over time. Integrative Medical of DFW+1
Telemedicine and Physical Therapy for Sciatica
Physical therapy is a key part of long-term sciatica care. Telemedicine makes it easier for your team to coordinate and supervise this care.
An NP–chiropractor team can:
-
Refer you to in-person physical therapy when you need hands-on manual work
-
Work with therapists to align goals: pain reduction, nerve mobility, strength, and posture
-
Review PT progress notes with you by video
-
Add or modify home exercises between in-person therapy visits
Modern integrative clinics describe physical therapy as treatment focused on your goals, your function, and your time—whether you are recovering from an acute episode of sciatica or managing long-term spine issues. Integrative Medical of DFW+1
Telemedicine for Office Workers and Remote Workers with Sciatica
Many people with sciatica sit for long periods at desks or work remotely at kitchen tables, couches, or beds. Poor ergonomics can worsen nerve pain.
Telemedicine allows providers to see your real work setup and give specific advice.
They may help you:
-
Adjust chair height, screen level, and keyboard position
-
Use lumbar support, cushions, or footrests
-
Create a schedule for movement breaks
-
Learn simple stretches you can do between meetings tigardchiropracticautoinjury.com+1
Chiropractic-based telemedicine visits for office workers often focus on spinal alignment, hip position, and load sharing between joints — even if the provider cannot physically adjust the spine during the visit, they can teach you how to move better and reduce pressure on the sciatic nerve. tigardchiropracticautoinjury.com+1
How to Prepare for a Telemedicine Visit for Sciatica
Preparing well can make your telemedicine visit smoother and more helpful.
Before your appointment
-
Check your technology
-
Test your camera, microphone, and internet connection
-
Charge your device and have a backup (like a phone) ready
-
-
Choose your space
-
Find a quiet, private room
-
Make sure you have enough room to stand, walk, and lie down if needed
-
-
Gather information
-
List your current medications and supplements
-
Have your medical history and imaging reports handy
-
Write down your main questions and goals for the visit Southeast Texas Spine+1
-
During the visit
-
Wear clothes you can move in (shorts, leggings, and a T-shirt)
-
Use a stable surface (wall, chair, or counter) for balance if you need to do standing tests
-
Be honest about your pain, function, and fears—this helps your provider design a realistic plan
Many spine clinics provide telemedicine checklists so patients feel confident and ready for their virtual appointment. Southeast Texas Spine+1
Limitations of Telemedicine in Sciatica Care
Telemedicine is powerful, but it is not the answer for every situation.
Telemedicine cannot:
-
Replace emergency care for severe symptoms
-
Perform hands-on spinal adjustments, manual therapy, or injections
-
Completely substitute in-person care when surgery or complex procedures are needed
Red-flag symptoms requiring urgent in-person evaluation or ER care
If you have any of the following, seek emergency or same-day in-person care:
-
Loss of bladder or bowel control
-
Numbness in the groin or “saddle area”
-
Sudden, severe weakness in the leg or foot
-
Fever with severe back pain
-
History of cancer, major trauma, or infection with new, intense back pain
In an integrative practice like Dr. Jimenez’s, telemedicine is used alongside in-person visits. The goal is to decide:
-
What can safely be managed at home
-
What needs an in-person evaluation
-
When to involve surgeons, neurologists, or pain specialists
How an Integrative Chiropractor–NP Team Follows You Over Time
Sciatica often improves, but it can also come and go. Long-term success usually requires ongoing guidance. Telemedicine makes this easier to maintain.
Follow-up telemedicine visits may include:
-
Reviewing pain levels, function, and activity
-
Adjusting exercise intensity or adding new movements
-
Fine-tuning posture and ergonomics as your work or home situation changes
-
Checking for side effects or problems with medications
-
Discussing lifestyle factors such as sleep, stress, and weight management Southeast Texas Spine+2apollospineandpain.com+2
Dr. Jimenez’s clinical experience shows that when patients feel seen and supported—through regular check-ins, education, and coordinated care—they are more likely to stay consistent with their home program and achieve better long-term outcomes. El Paso, TX Doctor Of Chiropractic+1
Practical Tips for Getting the Most from Telemedicine for Sciatica
Here are some simple strategies to make telemedicine work for you:
-
Treat the visit like an in-person appointment
-
Show up on time and minimize distractions
-
Have a notebook handy for instructions
-
-
Be specific about your goals
-
“I want to sit for 30 minutes without pain”
-
“I want to walk around the block again”
-
Clear goals help your provider design better plans
-
-
Use photos or videos
-
Take a short video of how you walk or how you get out of a chair during painful times
-
Share this with your provider if their platform allows
-
-
Stay consistent with home exercises
-
Put reminders in your phone
-
Tie exercises to habits (after brushing teeth, after lunch, etc.)
-
-
Ask for a written or emailed summary
-
Many clinics send a visit summary through the patient portal
-
This can include your diagnosis, exercise plan, and red-flag symptoms
-
The Future: Telemedicine, Sciatica, and Integrative Care
Telemedicine is no longer just an emergency backup plan—it is a core part of modern spine and pain care. Spine centers, pain clinics, and integrative practices across the country use telemedicine to: UT Southwestern Medical Center+2NJ Spine & Orthopedic+2
-
Speed up diagnosis and treatment
-
Improve convenience for patients in pain
-
Coordinate care between specialists, therapists, and primary providers
-
Support long-term recovery with flexible follow-ups
For people with sciatica, this means you can:
-
Get expert guidance without leaving your home
-
Partner with an integrative chiropractor and nurse practitioner who can see both the nerve problem and the whole person
-
Combine remote consultations, at-home exercises, and lifestyle changes into a comprehensive plan
Under the care of a dual-licensed provider like Dr. Alexander Jimenez, telemedicine becomes more than a video call. It becomes a bridge between medical science, chiropractic biomechanics, and day-to-day life—helping you move from intense nerve pain toward safer movement, better function, and long-term relief. El Paso, TX Doctor Of Chiropractic+2Evolve Chiropractic+2
References
UT Southwestern Medical Center. (2025, November 19). Virtual visits, real pain relief: Telemedicine brings convenient care for back issues. https://utswmed.org/medblog/telemedicine-for-back-and-spine-issues/
The Spine Institute of Southeast Texas. (n.d.). How does telemedicine work? https://www.southeasttexasspine.com/blog/how-does-telemedicine-work
The Spine Institute of Southeast Texas. (n.d.). How can telemedicine work to help treat my sciatica? https://www.southeasttexasspine.com/blog/how-can-telemedicine-work-to-help-treat-my-sciatica
The Spine Institute of Southeast Texas. (n.d.). 6 benefits of telemedicine. https://www.southeasttexasspine.com/blog/6-benefits-of-telemedicine
The Spine Institute of Southeast Texas. (n.d.). How to prepare for your telemedicine appointment. https://www.southeasttexasspine.com/blog/how-to-prepare-for-your-telemedicine-appointment
Everlywell. (n.d.). How telemedicine pain management works. https://www.everlywell.com/blog/virtual-care/telemedicine-pain-management/
NJ Spine & Orthopedic. (n.d.). What is telemedicine and can it work for back pain? https://www.njspineandortho.com/what-is-telemedicine-and-can-it-work-for-back-pain/
Apollo Spine & Joint. (n.d.). Enhance pain management with telemedicine. https://www.apollospineandpain.com/enhance-pain-management-with-telemedicine
Tigard Chiropractic & Auto Injury. (n.d.). Sciatica solutions: How chiropractic care can help office professionals find relief. https://www.tigardchiropracticautoinjury.com/blog/sciatica-solutions-how-chiropractic-care-can-help-office-professionals-find-relief
Tigard Chiropractic & Auto Injury. (n.d.). Dealing with pain from working remotely. https://www.tigardchiropracticautoinjury.com/blog/dealing-with-pain-from-working-remotely
Evolve Chiropractic. (n.d.). When sciatica strikes: How chiropractic care can provide relief. https://myevolvechiropractor.com/when-sciatica-strikes-how-chiropractic-care-can-provide-relief/
HealthCentral. (n.d.). Chiropractor for sciatica: Causes, symptoms, & diagnosis. https://www.healthcentral.com/condition/sciatica/chiropractic-treatment-sciatica
Integrative Medical of DFW. (n.d.). Physical therapy: Treatment focused on your goals. https://www.integrativemedical.com/physical-therapy
Jimenez, A. (n.d.). El Paso, TX chiropractor Dr. Alex Jimenez DC | Personal injury specialist. https://dralexjimenez.com/










