by Dr Alex Jimenez DC, APRN, FNP-BC, CFMP, IFMCP | Chiropractic, Chronic Back Pain, Lower Back Pain
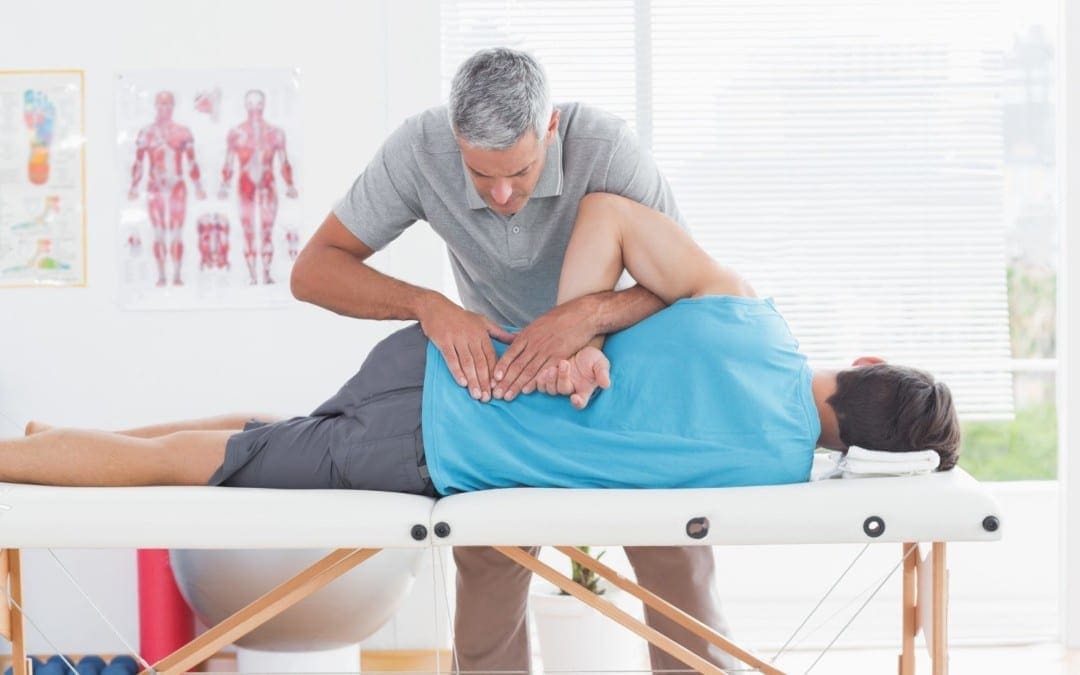
Chiropractors think that good health is decided by way of a healthy nervous system, particularly a healthy spinal column. Sometimes, vertebrae become misaligned and put pressure on the nerves exiting the spinal cord. The misalignment of a vertebra is called a chiropractic subluxation.
Chiropractors use specific methods to return the vertebrae in their proper locations or muster them to allow them to go freely when subluxations happen. These techniques are called spinal manipulations or adjustments. During an adjustment, the vertebra is freed in the misaligned location and returned to the right place in the spinal column. The adjustment permits the entire body to cure and preserve homeostasis once performed.
Chiropractors Are Trained In Many Different Adjustment Techniques
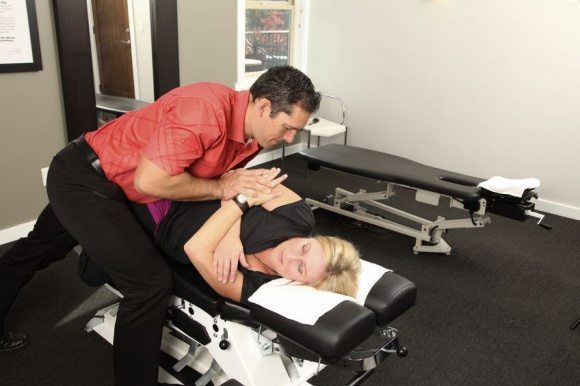
Some are done by hand; some necessitate using specialized instruments. Since each patient is different, your chiropractor will pick the best technique for the state. Nevertheless, don’t hesitate to ask the chiropractor which technique she or he will be doing and the way that it will be achieved.
Common Adjustment Techniques Employed By Chiropractors Are The Following:
- Toggle Drop – this is when the chiropractor presses down firmly on a specific part of the back. Subsequently, using a drive that is precise and rapid, the chiropractor aligns the spine. This really is accomplished to enhance mobility in the vertebral joints.
- Motion Palpation – this hand-on procedure is performed to determine in case your vertebrae are moving freely inside their normal planes of motion.
- Lumbar Spin -the chiropractor positions the patient on her or his side, then implements a thrust that is quick and precise returning it to its proper place.
- Release Work – the chiropractor applies gentle pressure using her or his fingertips to separate the vertebrae.
The chiropractor applies a quick thrust at once the table drops. The dropping of the table allows for a lighter adjustment without the twisting postures that can accompany the manual adaptation.
- Instrument adjustments – of correcting the spinal column frequently the gentlest ways. The patient lies on the table while a string is used by the chiropractor face down – filled activator instrument to do the adjustment. This technique is frequently used to perform adjustments on creatures too.
- Manipulation done under anesthesia (or twilight sedation) – this is performed by a chiropractor certified in this technique in a hospital outpatient setting when you’re unresponsive to traditional adjustments
Keep in mind that before you experience complete relief out of your symptoms you may really need to go back to the chiropractor’s office for additional adjustments.

Call Today!

by Dr Alex Jimenez DC, APRN, FNP-BC, CFMP, IFMCP | Chiropractic, Mobility & Flexibility, Power & Strength
I have been travelling through Athens and now Istanbul. My 11 year old is a Percy Jackson nut and has been filling me in with the who’s who of Greek mythology and I am learning Latin words every day. Quite an education!
I looked up the word syndesmosis and the Latin translation is “(New Latin, from Greek sundesmos) bond, ligament, from sundein, meaning to bind together”. As sports injury professionals, we know syndesmosis to be the joint articulation between the tibia and the fibula bones around the ankle. These two bones are �bound’ together with very firm and strong ligaments.
Syndesmosis comes to mind after I saw a girl sprain a syndesmosis at the Archaeological Museum in Istanbul today. This poor girl was preoccupied by the hundreds of cats and kittens running all over the place and did not see the uneven cobblestones on which she placed her foot. At the same time, she turned to change direction. This is a common mechanism of injury for a syndesmosis – a forced dorsiflexion and rotation on a fixed foot.
Rehab Masterclass Issue 140 Of Sports Injury Bulletin
Of all the ankle injuries, injury to the syndesmosis is the biggest pest to sports physios and the like. And unlike simple garden variety ankle sprains that heal quickly, the syndesmosis takes a LONG time to heal properly. If you deal with athletes that are susceptible to syndesmosis sprains, I’m sure you will agree that these are harder injuries to manage because of the severe consequences if done badly.
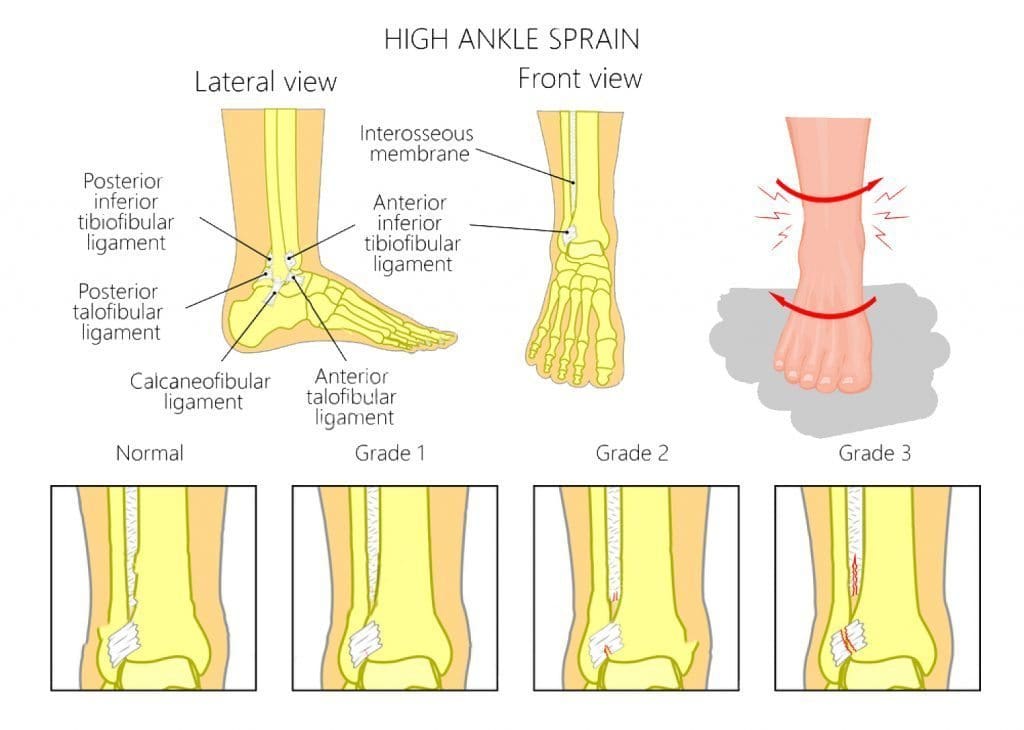
I go into a fair bit of detail in my Sports Injury Bulletin piece about syndesmosis injuries, detailing how they happen, how to identify them and then manage them. What I would like to highlight here are the implications of mismanaging a syndesmosis sprain.
In the current issue of The Journal of Sports and Physical Therapy, a group of Japanese researchers discovered that individuals who had chronic ankle instability (CAI) had a distal fibula that was positioned more lateral compared with healthy individuals with no CAI. In effect, those who had suffered serious syndesmosis injuries in the past and ended up with a wider distance between the fibula and the tibia, suffered more ongoing ankle pain than those without a tibfib separation.
Research shows that even a 1mm displacement of the talus within the mortise (due to a wider placed fibula) can reduce the contact area in the talocrural joint by 42% (Ramsey and Hamilton 1976). Mismanaged syndesmosis injuries, resulting in an excessive amount of opening, can lead to early onset arthritic changes and chronic ankle instability. The talus bone bounces around in the now wider tibfib articulation.
A Widening Of The Fibula Is Due To One Of The Following:
Poor initial management, whereby the athlete is allowed to weight bear too early and this weight bearing forces the fibula away from the tibia as the syndesmosis ligaments are trying to heal.
The degree of damage is so severe that proper tightening of these ligaments is not possible without surgical intervention such as a screw or similar being placed between the two bones to �force’ them together.
The key for a sports injury practitioner, is to properly identify a regular ankle sprain from a more serious syndesmosis injury. If you get this part wrong and allow the athlete to get back to weight bearing too early, then expect some complaints about a chronically painful ankle some time down the track.

Call Today!
Kobayashi et al (2014). �Fibular malalignment in individuals with chronic ankle instability.’ JOPST. 44(11); pp 841-910.
Ramsey and Hamilton (1976). J Bone and J Surgery Am. 58(3); 356-357.

by Dr Alex Jimenez DC, APRN, FNP-BC, CFMP, IFMCP | Chiropractic, Chronic Back Pain, Migraines, Neck Pain
About Pain Management (Medicine) Specialists
A pain medicine specialist is a medical or osteopathic doctor who treats pain due to disease, ailment, or injury. Many of these doctors are physiatrists or anesthesiologists although called interventional pain management specialists or pain medicine. Pain medicine is a mutlidisciplinary team effort generally affecting specialists in other disciplines, complimentary alternative medicine, along with radiology, psychiatry, psychology, oncology, nursing, physical therapy, and the patient’s primary care physician or other treating doctor.

Education & Training
After graduating medical school and completing a one-year internship, the physician enters a residency program normally in physical or anesthesiology medicine but sometimes from other fields like psychiatry and neurology. Upon conclusion of a residency program (typically 3 years long), the physician completes a one-year fellowship for advanced training in pain medicine.
Many pain medicine specialists are board certified. The organizations that board certify physiatrists, anesthesiologists, neurologists, and psychiatrists all collaborate to provide the board examination for the subspecialty of Pain Medicine. You can find numerous opportunities for pain management specialists to remain current with medical and technical improvements in pain medicine, such as scientific journals and society meetings.
Targets of Pain Management
The goal of pain medicine is to handle severe or long-term pain by reducing intensity and pain frequency. Besides addressing pain problems, a multidisciplinary pain management program may address your functional goals for activities of day-to-day living. Overall, a pain medicine plan aims to give you a feeling of well-being, increase your level of action (including return to work), and reduce or eliminate your reliance on drugs.
Many Kinds of Pain Treated
Pain medicine specialists treat all sorts of pain. Severe pain is described sharp or as acute and may indicate something is wrong. The pain experienced during dental work is an instance of intense pain. Pain lasting 6 months or longer is defined as chronic. This type of pain varies from mild to serious and is consistent. Spinal arthritis (spondylosis) pain is frequently chronic. A good consequence is produced by uniting different treatments regularly although chronic pain is difficult to handle.
- Degenerative disc disease
- Facet joint pain
- Sciatica
- Cervical and lumbar spinal stenosis
- Spondylolisthesis
- Whiplash
What to Anticipate During an Appointment
Your appointment with a pain or interventional pain management practitioner is much like other doctor visits. Although there are many similarities, the focus is fast managing it, and on your pain, the cause or contributing factors.
Pain medicine physicians execute a physical and neurological examination, and review your medical history paying particular focus on pain history. You may be asked many questions about your pain
- On a scale from zero to 10, with 10 being the worse pain imaginable, speed your pain.
- When did pain start? When pain started, what were you doing?
- Does pain disperse into other regions of the body?
- Is its intensity persistent, or is it worse at different times of night or the day?
- What really helps to alleviate the pain? Why is pain worse?
- What treatments have you ever attempted? What worked? What failed?
- Would you take over the counter drugs, vitamins, or herbal nutritional supplements?
- Does one take prescription medication? If so, what, how much, and how frequently?
Most pain medicine specialists utilize a standardized drawing of the front/back of the body to let you mark where pain is sensed, as well as indicate pain spread and type (eg, light, sharp). You may be asked to complete the form each time you see with the pain physician. The finished drawing helps you to evaluate your treatment progress.
Accurate Analysis Key to Treatment
Pain medicine includes diagnosing origin or the cause of pain. Making the proper identification may include getting an X ray, CT scan, or MRI study to verify the reason for your neck pr back pain. When treating spine-associated pain (which may include arm or leg symptoms), other tests, like discography, bone scans, nerve studies (electromyography, nerve conduction study), and myelography could possibly be performed. The proper analysis is crucial to some favorable treatment plan.
Some spinal ailments and pain treatment requires involvement of other specialists, such as your primary care physician, neurosurgeon, orthopaedic surgeon, and practitioners in radiology, psychiatry, psychology, oncology, nursing, physical therapy, and complimentary alternative medicine. The pain medicine specialist may consult with and/or refer you to a neurosurgeon or orthopaedic spine surgeon to determine if your pain difficulty necessitates back operation.

Call Today!

by Dr Alex Jimenez DC, APRN, FNP-BC, CFMP, IFMCP | Chiropractic, Sciatica
Several lumbar spine (lower back) disorders may cause sciatica. Sciatica is usually referred to as light to severe pain in the left or right leg. Occasionally doctors call a radiculopathy that is sciatica. Radiculopathy is a medical term used to spell out pain, numbness, tingling, and weakness in legs or the arms caused by a nerve root issue. It’s known as a cervical radiculopathy, in the event the nerve difficulty is in the neck. But since sciatica influences the low back, it is called a lumbar.
Pathways To Sciatic Nerve Pain

Five sets of matched nerve roots in the lumbar spine combine to generate the sciatic nerve. Beginning at the rear of the pelvis (sacrum), the sciatic nerve runs in the trunk, under the buttock, and down through the hip region into each leg. Nerve roots aren’t “solitary” structures but are part of the entire body’s entire nervous system capable of transmitting pain and sensation to different parts of the body. Radiculopathy happens when compression of a nerve root from a disc rupture (herniated disc) or bone spur (osteophyte) happens in the lumbar spine prior to it joining the sciatic nerve.
What Causes Sciatic Nerve Compression?
Several spinal ailments can cause spinal nerve compression and sciatica or lumbar radiculopathy.
- spondylolisthesis
- Injury
- piriformis syndrome
- spinal tumors
Common Sciatica Cause #1: Lumbar Bulging Disc or Herniated Disc
A bulging disk is also called a contained disc illness. What this means is the gel-like center (nucleus pulposus) remains “included” within the tire-like outer wall (annulus fibrosus) of the disk.
A herniated disc happens when the nucleus breaks through the annulus fibrosus. It is called a “non-controlled” disk disorder. Whether a disc bulges or herniates, disk stuff compress delicate nerve tissue and cause sciatica and can press against an adjacent nerve root.
The effects of a herniated disc are worse. In both instances, nerve compression and irritation cause inflammation and pain, muscle weakness, tingling, and often ultimately causing extremity numbness.
Common Sciatica Cause #2: Lumbar Spinal Stenosis
Spinal stenosis is a nerve compression illness most frequently affecting older adults. Leg pain similar to sciatica may happen as an effect of lumbar spinal stenosis. The pain is generally positional, frequently brought on by actions like standing or walking and relieved by sitting down.
Spinal nerve roots branch outward through passageways in the spinal cord called neural foramina comprised of bone and ligaments. Between each group of vertebral bodies, located on the left and right sides, is a foramen. Nerve roots pass through these openings and extend outward to innervate other portions of the body. The term foraminal stenosis can be used when these passageways become clogged causing nerve compression or narrow.
Common Sciatica Cause #3: Spondylolisthesis
Spondylolisthesis is a disorder that almost all commonly influences the lumbar spine. It’s distinguished by one vertebra slipping forwards over an adjacent vertebra. When a vertebra slips and is displaced, spinal nerve root compression happens and frequently causes sciatic leg pain. Spondylolisthesis is categorized as developmental (located at birth, grows during childhood) or got from spinal degeneration, trauma or physical stress (eg, lifting weights).
Common Sciatica Cause #4: Trauma
Examples include motor vehicle accidents, falling down, football and other sports. The impact may injure the nerves or, sometimes, the nerves may compress.
Piriformis syndrome is named after the piriformis muscle and the pain caused when the sciatic nerve is irritated by the muscle. The piriformis muscle and the thighbone is found in the lower part of the spine, connect, and aids in hip rotation. The sciatic nerve runs beneath the piriformis muscle. Piriformis syndrome grows when muscle spasms develop in the piriformis muscle thereby compressing the sciatic nerve. It may be challenging to diagnose and treat because of the shortage of x ray or magnetic resonance imaging (MRI) findings.
Common Sciatica Cause #5: Piriformis Syndrome
Piriformis syndrome is named after the piriformis muscle when the muscle irritates the sciatic nerve and the pain caused. The piriformis muscle and the thighbone is located in the low part of the backbone, connect, and aids in hip rotation. When muscle spasms develop in the piriformis muscle thus compressing the sciatic nerve, piriformis syndrome develops. It can be hard to diagnose and treat due to the lack of x-ray or magnetic resonance imaging (MRI) findings.
Common Sciatica Cause #6: Spinal Tumours
Spinal tumors are abnormal growths which are either benign or cancerous (malignant). Fortunately, spinal tumors are uncommon. But when a spinal tumor develops in the lumbar region, there’s a risk for sciatica to grow as a result of nerve compression.
Call your doctor should you imagine you have sciatica. The very first step toward relieving pain is a proper diagnosis.

Call Today!

by Dr Alex Jimenez DC, APRN, FNP-BC, CFMP, IFMCP | Diets, Nutrition, Wellness
When most people think of injury or inflammation, they think of a sprained ankle or injured low back due to acute trauma.
However, inflammation is a far more serious health issue.
In fact, it can be said that inflammation is the root of all disease.
One may not even notice the immediate affects of chronic inflammation, but it can be there, particularly if you don�t eat properly or exercise constantly.
That�s because inflammation is actually the body�s natural response to stress�be it physical, dietary,� environmental and/or even emotional. Once your body starts to become inflamed, it places you at risk for everything from weight gain, allergies, migraines, and susceptibilities to more serious illnesses such as heart disease, stroke, gout, diabetes, Alzheimer�s disease and even cancer.
Even the healthiest among us will have some type of inflammation�if you live in today�s fast and toxin-filled world, you have inflammation. The real question is what do you plan to do about it?
Where Does Inflammation Start?
The process of inflammation actually begins in your gut!
People tend to overlook their digestive system as a source of disease, but it makes sense when you consider that our guts are home to about 70 percent of our immune system and where 80 percent or more of our IgA cells (immune cells) live.
Where inflammation comes in is when the permeability of this organ starts to vary depending on different chemicals and conditions.
This, in turn, allows things like toxins, viruses, and bacteria, even undigested food, to enter your bloodstream through the larger holes in this lining. This condition, known as a leaky gut syndrome (LGS), is key to inflammation and where things can start going downhill�fast.
Constant damage to your intestinal lining from the leaky gut syndrome eventually will destroy the essential microvilli � tiny projections that exist in, on, and around the cells in your intestine and help with absorption and secretion.
When damaged the microvilli are unable to process and utilize the necessary nutrients and enzymes for digestion, which means your digestion eventually becomes disabled. When this happens, your body essentially sends out an alarm and starts an attack on the foreign bodies, such as the undigested food particles or viruses, yeast, etc.
And as part of this response, it becomes inflamed, causing allergic reactions and eventually other symptoms (diseases).
Common Inflammation Triggers
More and more, research is linking food to disease. We know that certain foods are clearly not healthy, while others have shown to promote healing.
But there are also some foods�mainly the majority of those that make up the standard American diet�that can be considered �inflammatory foods.�
Today, there are food additives in basically anything that isn�t organic. And now, we are starting to realize that even some foods that would otherwise seem �natural� can also be triggers.
These inflammatory triggers include such things as refined sugar, chemical additives, GMOs, artificial dyes and anything processed. All of these essentially trigger inflammation in your gut and can lead to devastating health issues.
The Biggest Cause Of Inflammation
Food and chemicals are not the only triggers.
Stress is also one of the biggest causes of inflammation.
Probably one of the reasons we don�t always link stress to disease is that it takes time for it to wreak havoc on our bodies. But anyone who has been under long-term stress will tell you that is can be deadly.
Eventually, your body starts to give out and break down. But now that you know this, you can limit the damage by recognizing the 14 most common signs of inflammation before they get out of hand.
14 Warning Signs Of Inflammation
1. Chronic fatigue
2. Acne
3. Food cravings
4. Binge eating
5. Unexplainable weight gain (not associated with eating more)
6. Bloating
7. Water retention
8. Diarrhea or constipation
9. High blood pressure
10. Irritable bowel syndrome (IBS)
11. Joint pain
12. Stiffness
How To Treat Inflammation Naturally
Diet is the most important stuff to look at when addressing inflammation. Before the invasion of drugs to treat everything imaginable, the food was considered medicine.
Hippocrates said, �Let food be thy medicine and medicine be thy food.� These are words to live by, literally.
The only caution is that the food must be fresh, unprocessed and as natural as possible. The type of food you eat also determines the types of microbes that will grow and live in your gut.
Good microbes are necessary for proper digestion and absorption of the vitamins, minerals, and nutrients in your food. Processed foods are the main cause of inflammation, so you will need to start by eliminating all of these from your diet.
Refined sugar and wheat are also big contributors. And if you have food sensitivities, which is highly likely if you have inflammation, foods such as gluten, and cow�s milk can trigger further inflammation.
A diet based on fresh, mostly raw vegetables, salads, good sources of protein, such as eggs, seafood, organic or grass-fed meat and poultry, as well as healthy fats that include omega-3 fats, fresh fruit and plenty of nuts and seeds (again raw is better) and plenty of probiotics, is what is going to heal inflammation for good. As a good rule of thumb, try to avoid any food that comes pre-packaged.
There are also many foods that have been shown to be especially good for fighting inflammation. Choosing as many of these as possible will help to speed the healing process.
Proven Anti-Inflammatory Foods:
- Fruits
- Vegetables
- Whole and cracked grains
- Beans and legumes
- Healthy fats (organic coconut oil, cold pressed olive oil
- Flaxseed and hempseed
- Fish and seafood
- Mushrooms
- Grass-fed lean meats, organic cheese and yogurt
- Spices (turmeric, ginger, curry, garlic, chili peppers, cinnamon, etc.)
- Probiotics and fermented foods (kefir, kombucha, sauerkraut, yogurt)
Inflammatory Foods To Avoid Completely:
- Processed foods
- Certain dairy
- Processed meats
- Refined sugars
- Trans fats
- Gluten
- Soda
- Lard
- Caffeine
- Alcohol
Other Tips
Drink plenty of filtered water as water helps flush toxins out of your body and keeps you hydrated. Try to reduce, if not eliminate all stressors in your life as much as possible. Make sure to get regular exercise and try things like meditation, aromatherapy, massage, and soothing music to relax your mind and body. And above all else, get enough sleep!
Bonus Recipe
The #1 Anti-inflammatory� smoothie
Ingredients:
- 1/2 cup frozen pineapple or mango
- 1 banana
- 1 cup coconut milk
- 1 teaspoon chia seeds
- 1/2 teaspoon ginger
- � teaspoon turmeric powder
- 1 teaspoon maca root powder (optional)

Call Today!

by Dr Alex Jimenez DC, APRN, FNP-BC, CFMP, IFMCP | Chiropractic, Integrative Functional Wellness, Integrative Medicine, Wellness
More Americans are looking beyond Western medicine to help relieve their back, neck, and spinal joint pain, including osteoarthritis of the backbone. In this specific article, we discuss Complementary and Alternative Medicine (CAM), which is also called Complementary and Integrative Medicine.
Interchangeable Terms
When an option (not mainstream) practice is combined with standard (mainstream) medicine, it�s called �complemental� or �integrative� health care. It�s called �alternative.� when it�s used in place of traditional medicine Nevertheless, these terms are frequently used interchangeably.
Complementary Alternative/Integrative Treatments
Although treatments might be combined you will find five general types of CAM therapies.
1. Alternative Medical Systems
Naturopathic or naturopathy medical care may include water therapy, massage, and herbal drugs.
2. Head-Body Techniques
Head-body techniques may help a patient with back or neck pain to utilize their head to change or restrain their symptoms in a way that is positive, therefore reducing pain.
3. Biologically-Based Therapies
Biologically-based treatments feature nature-based substances such as botanicals and dietary supplements to ease pain. Natural substances contain ginseng, ginkgo, fish oil, or Echinacea and could be obtainable in different kinds, including a tea, aromatherapy oils, syrup, powder, pill, or capsule.
4. Body-Based Practices
Body-established practices include different types of massage, body alignment techniques, osteopathic manipulation and chiropractic.
5. Energy Therapies
Energy therapies unblock energy fields or may help shift. Qi gong (eg, breathing techniques), Reiki (eg, stress reduction/relaxation), and magnets are treatments based on transferring energy.
Is Alternative, Complementary Or Integrative Therapy Right For You?
To assist you decide, look at the next points.
- If insurance coverage is essential to you, be sure to consult your health insurance provider before you select a CAM treatment to make certain the professional is insured.
- Learn as much as you can about the alternate treatment you’re enthusiastic about.
- Take into account that although a complementary alternative treatment may be popular, that doesn�t make it correct for you personally.
- Unlike mainstream medical care and procedures, some (if not most) alternative therapies are not scientifically validated by clinical trials and/or research studies. The amount of human players is frequently little, while there may be studies supporting a particular practice.
- Simply because a material is natural doesn�t mean it can�t damage you, cause illness or allergic reaction, or a serious interaction with a drug. For instance, blood pressure can be raised by ginseng.
- Always tell your treating physician about all of the herbs, vitamins and nutritional supplements (in any kind) that you take, particularly if you’re scheduled to get a neck or back process (eg, spinal injection, operation).
- Select your alternative therapy professional with all precisely the same attention and concern you would for pain management specialist or a back surgery.

Call Today!
Sources:
Rosenzweig S. Overview of Complementary and Alternative Medicine. Merck Manual. Consumer Version.� www.merckmanuals.com/home/special-subjects/complementary-and-alternative-medicine-cam/overview-of-complementary-and-alternative-medicine.
National Center for Complementary and Integrative Health (NCCIH). Complementary, Alternative, or Integrative Health: What�s In a Name? March 2015. https://nccih.nih.gov/health/integrative-health.

by Dr Alex Jimenez DC, APRN, FNP-BC, CFMP, IFMCP | Chiropractic, Chronic Back Pain, Migraines, Neck Pain
You get up with it. You go to sleep with it. An incredible number of men and women live with chronic back or neck pain every day. What’s chronic pain? It is technically defined as pain that lasts for 12 weeks or more�even after pain isn’t any longer acute (short-term, serious pain) or the injury has healed.
Accurate Analysis
Getting an exact identification of the reason for neck pain or your back is vital to the outcome of your treatment plan. Depending on the severity and cause of your pain that is chronic, you might need to find out different specialists in addition to your own primary care physician�pain medicine specialist, orthopaedic spine surgeon, neurosurgeon, physiatrist, rheumatologist, physical therapist among others. Over time your chronic pain need to be reevaluated, and may transform, which might affect the way it is handled.
Your chronic back or neck pain treatment generally features a variety of treatments to maximize results that are great. A number of the treatments your doctor prescribes and recommends may include:
Physical Therapy:
Extending and strengthening muscles is vital in the treatment of neck pain or chronic back.
Chiropractic Care:
Depending on your own diagnosis, chiropractic care may be recommended by your doctor. Studies have demonstrated that two weeks of day-to-day exploitation by a chiropractor can result in considerable progress in a few patients with persistent low back pain and referred leg pain.

Medicines:
There are lots of different prescription medications to take care of neuropathic pain, inflammation, muscle spasms, and pain. Additionally, you will find drugs to treat conditions that often accompany chronic pain, including drugs that will help you sleep, alleviate depression, and reduce nervousness.
Processes:
Your doctor may recommend a spinal cord stimulator, spinal injections, drug heart, or spine surgery. You can get a second opinion, in the event you might be uncertain about the treatment plan recommended.
Coping skills:
Never underestimate the power of your head. Your mood and mental perspective can greatly make an impact on your level of pain. Talk with a trained specialist to understand relaxation and coping skills.
Complementary Treatments:
Many physicians recommend acupuncture and other types of traditional Chinese medicine. Speak to your doctor about these choices.
A couple of words about …. age, fitness, body weight
You probably involve some control over body weight and your level of fitness, although you can�t stop aging or its effects. While you can�t stop the clock on the cellular changes that are recognized to accompany aging�such as loss of muscle mass and bone density �you can take little steps today to build a more stronger�you tomorrow.
It�s understood that patients with chronic back or neck pain may not feel like being active, going to the gym and even adhering to a home exercise program. Yet, being active can help chronic pain because during exercise your body releases endorphins�your body�s natural painkiller.
Moreover, by teaming up together with and/or your physician physical therapist you can start to build abdominal muscles that are strong �essential to your own body�s center strength which helps support your back.
Did you know that by simply losing even 5 to 10 pounds you can reduce back pain? It�s true. Carrying around extra weight translates to added stress to the low back that may exacerbate pain.
Conclusion
In many instances, aggressive and early treatment of chronic back or neck pain can make a life-changing difference. But remember that knowledge is power: Be certain you comprehend your alternatives before deciding which route to take.

Call Today!























