Contents
MLS Laser and Chiropractic Care for Back and Joint Pain
Abstract
In this educational post, I walk you through how we integrate modern photobiomodulation (MLS laser therapy) with chiropractic care, manual therapy, and active rehabilitation for spinal and joint pain. You will learn how we set up treatment for low back facet pain, why patient comfort and precise dosing matter, and how we target both the painful site and the connective tissue network to drive better outcomes. I explain energy density (joules per cm²), the Arndt–Schulz dose-response principle, tissue optics, and how pulsed dual-wavelength lasers engage mitochondrial and neuroimmune pathways to reduce pain and enhance recovery. We will also explore how robotic and handheld delivery complement each other, how we schedule acute and chronic care plans, how we combine laser with shockwave, PRP, and movement therapy, and when this approach can delay surgery by improving pain and function. Throughout, I share clinical observations from our El Paso Back Clinic and highlight evidence from leading researchers using rigorous, evidence-based methods. The emphasis is on integrative chiropractic and physical therapy, with medications and hormones kept in the background.
At El Paso Back Clinic, our mission is to merge hands-on chiropractic care, targeted physical therapy, and precision technologies that safely accelerate healing. One modality we employ is MLS laser therapy, a form of photobiomodulation that uses synchronized near-infrared wavelengths to influence cellular energy, microcirculation, and neuroinflammatory signaling. In this post, I reframe a recent procedural walkthrough from my perspective and expand on the physiology, clinical reasoning, and practical protocols we use every day with patients presenting with low back pain, knee osteoarthritis, plantar fasciitis, and other musculoskeletal conditions. The star is not the device; it is the integrated plan that places your spine and movement at the center of care.
Optimizing patient comfort and precision: Why setup matters
- Key concepts:
- Patient positioning
- Direct-to-skin contact when appropriate
- Targeting by symptoms and anatomy
- Stability during unattended robotic delivery
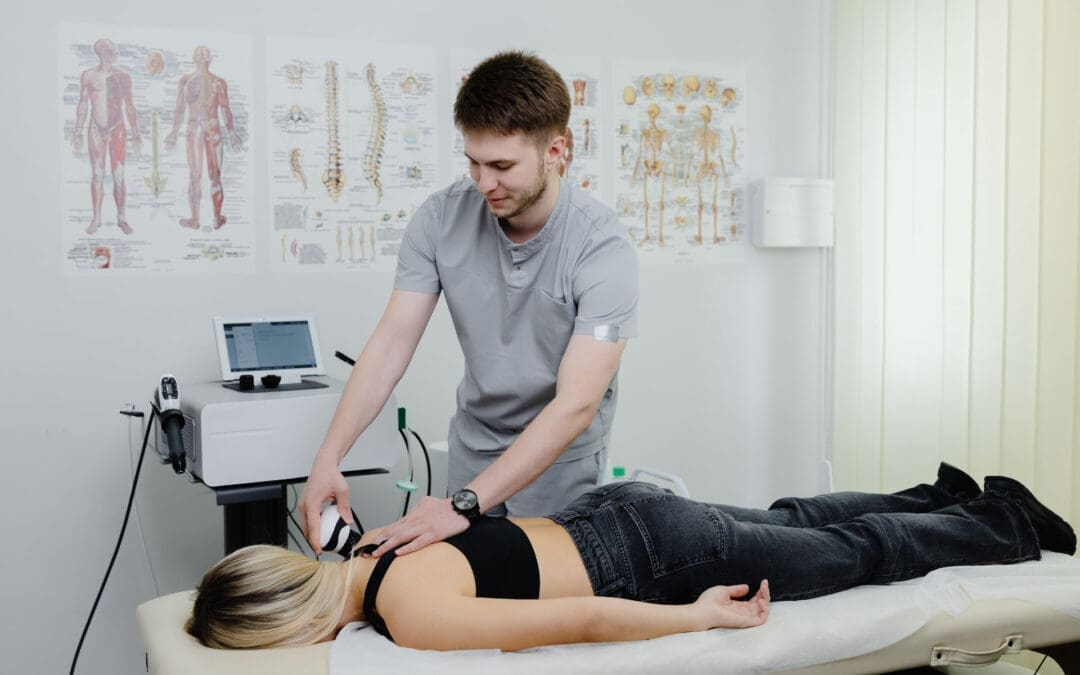
When I set up laser therapy—especially with a robotic head—my first priority is patient comfort and stability. If a patient shifts during an unattended cycle, the beam may drift from the intended target. For lumbar facet-mediated pain at L4–L5, I position the patient comfortably prone, ensure the treatment field is exposed with direct skin access when using a contact handpiece, and confirm the exact region of maximal tenderness and referral (e.g., right-sided zygapophyseal joint pain with proximal radiation).
To minimize error, I zero the device’s X and Y axes, center the beam over the primary pain generator, then expand the field to include adjacent connective tissue tracks. This is our clinical multimodal approach: treat the source, the site, and the surrounding soft tissue network. By caring for the paraspinal fascia, intermuscular septa, and periarticular tissues, we respect that pain is rarely a single-point phenomenon. Fascia transmits load and communicates mechanosensory signals; addressing it improves regional glide and reduces nociceptive drive.
Why direct skin contact? Tissue optics favor minimal reflection and refraction losses. Air-skin interfaces reflect more energy, especially at certain angles. When we must avoid contact—such as at post-surgical sites or in cases of allodynia—we employ a non-contact, collimated robotic head positioned at an optimal focal distance, measured with a calibrated ruler.
Robotic plus handheld delivery: Complementary tools
- Robotic head:
- Non-contact, collimated beam; ideal for broad areas, post-surgical sensitivity
- Software auto-recalculates dose time when X-Y field size changes
- Handheld contact piece:
- Tactile feedback for focal trigger points and joint spaces
- Allows dynamic, movement-based application during active care
In practice, I often run both channels simultaneously. The robot delivers a uniform, programmable energy density across a defined area while I probe and treat focal trigger points or facet capsules with the handheld. This mirrors how we layer manual therapy with exercise: a global reset paired with local precision.
Dosing by energy density: The language of photobiomodulation
- Target dose: typically 4–10 joules/cm², depending on condition and depth
- Why density matters more than total joules: tissue dose equals energy per unit area
- Auto-time calibration: changing the field size while maintaining the same J/cm² adjusts the total joules and time automatically
We dose by energy density, not just total energy. For example, a lumbar facet region might be set to 6 J/cm². On a larger field, total joules increase, but the cellular dose per square centimeter remains constant, aligning with literature-supported ranges that optimize photobiomodulation responses without tipping into bioinhibition. This reflects the Arndt–Schulz principle: too little energy yields no change, optimal energy stimulates, and excessive energy can dampen biological activity.
The physiology behind pain relief and tissue recovery
- Mitochondrial activation:
- Photons at near-infrared wavelengths interact with cytochrome c oxidase, improving electron transport and boosting ATP production
- Enhanced ATP supports ion pump function, cytoskeletal remodeling, and protein synthesis required for tissue repair
- Nitric oxide and microcirculation:
- Photo-dissociation of nitric oxide from cytochrome c oxidase and endothelial effects promotes vasodilation and microvascular perfusion, aiding oxygen delivery and metabolite clearance
- Neuroinflammatory modulation:
- Downregulation of pro-inflammatory cytokines and modulation of glial activity reduce peripheral and central sensitization
- Neural effects and immediate analgesia:
- Modulation of small-diameter nociceptive fibers and gate-control mechanisms can provide early symptom relief
- Collagen and connective tissue remodeling:
- Changes in fibroblast activity and collagen organization may improve tendon/ligament structure over time when paired with load-specific rehab
In our clinic, patients sometimes report warmth or a faint tingling, but with synchronized pulsed delivery and short pulse durations, surface heat remains low while energy is effectively absorbed at depth. When tissue temperature stays stable over time, we know we are within the desired window: enough photons to trigger biochemical cascades without superficial overheating.
Why pulsed, dual-wavelength delivery matters
- Wavelength pairing:
- 808 nm: deeper penetration for mitochondrial and vascular effects
- 905 nm: high peak power in short pulses adds neuromodulatory and analgesic benefits while protecting against thermal buildup
- Synchronized pulse trains:
- High peak, short duration pulses deliver energy in “packets,” allowing absorption periods between bursts and reducing superficial heat accumulation
These engineering choices align with clinical goals: delivering energy to deeper targets, such as facet capsules or the posterior knee compartment, while preserving patient comfort.
Chiropractic integration: Adjustments, motor control, and fascia
- Spinal adjustments:
- Restoring joint play at hypomobile segments reduces aberrant mechanoreceptor input and reflex muscle guarding
- Fascial glide and soft-tissue work:
- Instrument-assisted or hands-on release improves shear planes; laser primes fibroblasts and microcirculation for better tissue response
- Neuromotor retraining:
- Laser reduces pain-inhibition, enabling better activation of stabilizers (e.g., multifidus, transversus abdominis)
- We pair laser sessions with graded movement to convert biochemical gains into functional patterns
Laser does not replace chiropractic care; it helps us reach the dose of movement sooner by lowering pain and stiffness that otherwise block progress. For example, after an MLS session over L4–L5 facets and paraspinals, we cue diaphragmatic breathing and segmental stabilization to capitalize on reduced nociception and improved circulation.
Case walk-through: Low back facet pain (L4–L5)
- Assessment:
- Right-sided facet loading pain with limited extension and paraspinal tenderness
- No red flags; neurological exam stable
- Laser setup:
- Patient prone, area exposed; robot field centered over right L4–L5 facet region
- Density: 6 J/cm², field expanded to capture paraspinal fascia and myofascial referral zones
- Handheld: contact sweeps over identified trigger points
- Session length:
- Robot 6–10 minutes, depending on field size; handheld 20–30 seconds per trigger point
- Immediate follow-up:
- Prone press-ups to reassess extension tolerance
- Gentle lumbar stabilization exercises to lock in gains
- Home plan:
- Extension-biased mobility as tolerated, core endurance drills, ergonomic cues
What my patients often notice is not just pain relief within hours but improved ease of movement—the kind of change that allows us to progress from passive care to active loading.
Knee osteoarthritis: Accessing the joint intelligently
- Beam access matters:
- Anterior patella reflects substantial energy; flexing the knee opens the joint space and reduces reflection
- Posterior and medial/lateral approaches improve delivery to synovium and periarticular tissues
- Dosing strategy:
- Target 4–8 J/cm² per compartment; treat multiple compartments in the same session by apportioning field time
- Integration with PT:
- Laser to modulate pain and effusion
- Progressive quadriceps and hip strengthening, gait retraining, and balance work
- Manual therapy for capsular mobility as indicated
While no laser regrows cartilage in advanced bone-on-bone disease, many of our patients experience reduced pain and swelling and better function, which can delay the need for surgery. The goal is to expand the movement envelope required for strength and neuromuscular control.
Acute vs. chronic protocols: Cumulative effects and scheduling
- Acute conditions:
- Six treatments delivered as close to daily as feasible (e.g., Monday–Wednesday–Friday pattern), aiming for rapid symptom control
- Chronic conditions:
- Twelve treatments, ideally within four weeks, to build cumulative neuroimmune and mitochondrial effects
- Why packages:
- Effects are additive; stopping after early relief risks relapse before tissue remodeling and motor reeducation are complete
- Reassessment points:
- After 3–4 sessions: evaluate pain and function
- After 6–12 sessions: progress exercise intensity, reduce passive modalities
Our patients often report noticeable changes 4–6 hours after a session; we encourage them to “test” function later the same day (for example, stair climbing or walk tolerance) to anchor improvements to real-life tasks.
Combining laser with orthobiologics and shockwave
- With PRP:
- Two to three pre-injection laser sessions to improve local perfusion and tissue readiness
- Day-of-injection: protocol tailored to avoid blunting intended inflammatory signaling while supporting analgesia
- Six post-injection sessions to enhance microcirculation and cellular energy during proliferative phases
- With shockwave:
- Laser can reduce pain and prime tissues for mechanical signaling from shockwave
- Sequence depends on goals; we often laser first for analgesia, then apply focused shockwave for mechanotransduction, followed by graded loading
- Rationale:
- Photobiomodulation and mechanotherapy act on complementary pathways—bioenergetics and microcirculation (laser) plus tenocyte activation and neovascular remodeling (shockwave)
Hormonal or medication considerations remain in the background for us; when appropriate, we coordinate with the patient’s prescribing providers to avoid interventions (e.g., routine NSAIDs immediately after PRP) that might dampen desired signaling. Our primary emphasis remains movement-based rehabilitation supported by laser and manual care.
Bone and postoperative considerations
- Bone healing:
- The evidence base for photobiomodulation in fracture healing exists but varies by device and parameters; in clinical experience, early application within 7–10 days post-fracture may support the inflammatory and early reparative phases. This is commonly considered off-label for certain devices and requires case-by-case judgment and collaboration with the treating orthopedic team
- Post-surgical care:
- Non-contact robotic delivery allows dosing without skin contact when sensitivity is high
- Goals include edema control, pain reduction, and earlier initiation of therapeutic exercise
Dose ceilings and the bioinhibition paradox
- Arndt–Schulz law:
- Insufficient dose yields no effect; optimal dose stimulates; excessive dose may inhibit
- Practical application:
- If more time is desired, we distribute energy across multiple approaches (e.g., anterior-posterior or medial-lateral fields) instead of stacking excessive dose on one spot
- Skin heating as a red flag:
- Significant surface heat suggests wrong wavelength, excessive continuous power, or inadequate pulse spacing
- With synchronized pulsed delivery, tissue temperature should remain relatively stable across time
Why we choose integrative chiropractic first
- Movement is medicine:
- Lasting recovery depends on restoring load tolerance and motor control
- Laser as an enabler:
- By reducing pain and improving microcirculation, the laser allows earlier, higher-quality movement practice
- Manual plus active care:
- Adjustments restore segmental motion; soft-tissue therapy restores glide; exercise cements patterning and strength
Clinical observations from El Paso Back Clinic
- Low back facet syndrome:
- Patients frequently report a “melting” of stiffness within the same day after an MLS session paired with extension-bias exercise; repeated sessions lower baseline pain and improve extension tolerance, allowing us to progress to anti-rotation and hip hinge training
- Knee osteoarthritis:
- Combining posterior-compartment laser dosing with patellar mobilization and quadriceps strengthening reduces pain during sit-to-stand and stair negotiation within two to three weeks; gains consolidate when patients adhere to home-based strength and balance work
- Plantar fasciitis:
- Laser applied to the medial calcaneal region and along the plantar fascia with calf mobility and foot intrinsics training shortens the “first-step” pain window and speeds return to walking programs
- Post-injection care:
- In patients receiving PRP from collaborative providers, pre- and post-injection laser often reduces pain spikes and supports earlier initiation of controlled loading, which in turn improves functional outcomes at 6–12 weeks
Safety, reliability, and patient communication
- Safety profile:
- Proper eyewear, attention to reflective surfaces, and adherence to dosing ranges keep risk low
- Device reliability:
- Modern systems include field service support; routine calibration and training ensure consistent delivery
- Expectations:
- We counsel that pain did not develop in ten minutes and will not vanish in ten; however, many feel better within hours, see consistent improvement after three sessions, and sustain gains with a full plan of care
Putting it all together: A typical plan
- Evaluation:
- History, movement assessment, palpation, neurological screen, and imaging if indicated
- Plan creation:
- Define primary pain generators and movement deficits
- Choose laser parameters (wavelengths, pulsing, J/cm²) and field geometry
- Integrate manual therapy and exercise blocks within each visit
- Visit flow:
- Laser (robotic field + handheld focal points)
- Manual therapy for joint and soft tissue restrictions
- Targeted exercises (mobility, motor control, strength)
- Education and home program
- Progression:
- Increase exercise intensity as pain decreases
- Taper passive modalities
- Reassess goals every 3–4 sessions
Why these techniques work, in plain terms
- Pain is both chemical and mechanical. Laser modifies the chemical environment (reduces inflammatory signaling, increases ATP, improves microcirculation). Chiropractic and rehab address the mechanical side (joint motion, tissue glide, strength, coordination). Combining them tackles the problem from both angles
- The nervous system adapts to pain by inhibiting movement. Rapid analgesia from laser helps unlock motor patterns so we can retrain stability and strength sooner
- Tissues heal under the right load. Once pain is controlled and circulation improved, progressive loading guides collagen alignment and muscle conditioning for durable outcomes
Evidence-based grounding
Photobiomodulation has a growing body of research demonstrating analgesic, anti-inflammatory, and pro-recovery effects in musculoskeletal conditions. Rigorous, modern methodologies—randomized controlled trials, dose–response investigations, and consensus guidelines—support dosing in the 4–10 J/cm² range for many superficial-to-moderate-depth targets and highlight the importance of wavelength, pulse structure, and treatment frequency. Clinical effectiveness is maximized when photobiomodulation is embedded within active rehabilitation rather than used in isolation.
If you are considering care at El Paso Back Clinic, our team will assess your unique presentation and craft an integrative plan that prioritizes spinal mechanics, movement, and function—leveraging laser therapy where it adds value and always keeping the emphasis on your long-term resilience.
References
- Bjordal, J. M., Johnson, M. I., Iversen, V., Aimbire, F., & Lopes-Martins, R. A. B. (2006). Low-level laser therapy in acute pain: A systematic review of possible mechanisms of action and clinical effects. Photomedicine and Laser Surgery, 24(2), 158–168.
- Chung, H., Dai, T., Sharma, S. K., Huang, Y. Y., Carroll, J. D., & Hamblin, M. R. (2012). The nuts and bolts of low-level laser (light) therapy. Annals of Biomedical Engineering, 40(2), 516–533.
- Glazov, G., Yelland, M., & Emery, J. (2016). Low-level laser therapy for chronic non-specific low back pain: A meta-analysis of randomised controlled trials. Acupuncture in Medicine, 34(5), 328–341.
- Hamblin, M. R. (2016). Mechanisms and applications of the anti-inflammatory effects of photobiomodulation. AIMS Biophysics, 3(3), 337–361.
- Hamblin, M. R., & Demidova, T. N. (2006). Mechanisms of low level light therapy. In Proceedings of SPIE 6140, Mechanisms for Low-Light Therapy (pp. 1–12).
- Hashmi, J. T., Huang, Y.-Y., Osmani, B. Z., Sharma, S. K., Naeser, M. A., & Hamblin, M. R. (2010). Role of low-level laser therapy in neurorehabilitation. PM&R, 2(12 Suppl 2), S292–S305.
- Huang, Z., Ma, J., Chen, J., Shen, B., Pei, F., & Kraus, V. B. (2015). The effectiveness of low-level laser therapy for nonspecific chronic low back pain: A systematic review and meta-analysis. Arthritis Research & Therapy, 17, 360.
- Karu, T. (1999). Primary and secondary mechanisms of action of visible to near-IR radiation on cells. Journal of Photochemistry and Photobiology B: Biology, 49(1), 1–17.
- Stausholm, M. B., Naterstad, I. F., Joensen, J., & Lopes-Martins, R. A. B. (2019). Efficacy of low-level laser therapy on pain and disability in knee osteoarthritis: A systematic review and meta-analysis of randomized placebo-controlled trials. BMJ Open, 9(10), e031142.
- World Association for Laser Therapy. (2010). Recommended treatment dosages for Low Level Laser Therapy.
General Disclaimer, Licenses and Board Certifications *
Professional Scope of Practice *
The information herein on "MLS Laser and Chiropractic Care: A New Approach" is not intended to replace a one-on-one relationship with a qualified health care professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional.
Blog Information & Scope Discussions
Welcome to El Paso's Premier Wellness and Injury Care Clinic & Wellness Blog, where Dr. Alex Jimenez, DC, FNP-C, a Multi-State board-certified Family Practice Nurse Practitioner (FNP-BC) and Chiropractor (DC), presents insights on how our multidisciplinary team is dedicated to holistic healing and personalized care. Our practice aligns with evidence-based treatment protocols inspired by integrative medicine principles, similar to those on this site and on our family practice-based chiromed.com site, focusing on naturally restoring health for patients of all ages.
Our areas of multidisciplinary practice include Wellness & Nutrition, Chronic Pain, Personal Injury, Auto Accident Care, Work Injuries, Back Injury, Low Back Pain, Neck Pain, Migraine Headaches, Sports Injuries, Severe Sciatica, Scoliosis, Complex Herniated Discs, Fibromyalgia, Chronic Pain, Complex Injuries, Stress Management, Functional Medicine Treatments, and in-scope care protocols.
Our information scope is multidisciplinary, focusing on musculoskeletal and physical medicine; wellness; contributing etiological viscerosomatic disturbances within clinical presentations; associated somato-visceral reflex clinical dynamics; subluxation complexes; sensitive health issues; and functional medicine articles, topics, and discussions.
We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and licensure jurisdiction. We use functional health & wellness protocols to treat and support care for musculoskeletal injuries or disorders.
Our videos, posts, topics, and insights address clinical matters and issues that directly or indirectly relate to our clinical scope of practice.
Our office has made a reasonable effort to provide supportive citations and has identified relevant research studies that support our posts. We provide copies of supporting research studies upon request to regulatory boards and the public.
We understand that we cover matters that require an additional explanation of how they may assist in a particular care plan or treatment protocol; therefore, to discuss the subject matter above further, please feel free to ask Dr. Alex Jimenez, DC, APRN, FNP-BC, or contact us at 915-850-0900.
We are here to help you and your family.
Blessings
Dr. Alex Jimenez, DC, MSACP, APRN, FNP-BC*, CCST, IFMCP, CFMP, ATN
email: [email protected]
Multidisciplinary Licensing & Board Certifications:
Licensed as a Doctor of Chiropractic (DC) in Texas & New Mexico*
Texas DC License #: TX5807, Verified: TX5807
New Mexico DC License #: NM-DC2182, Verified: NM-DC2182
Multi-State Advanced Practice Registered Nurse (APRN*) in Texas & Multi-States
Multi-state Compact APRN License by Endorsement (42 States)
Texas APRN License #: 1191402, Verified: 1191402 *
Florida APRN License #: 11043890, Verified: APRN11043890 *
Colorado License #: C-APN.0105610-C-NP, Verified: C-APN.0105610-C-NP
New York License #: N25929, Verified N25929
License Verification Link: Nursys License Verifier
* Prescriptive Authority Authorized
ANCC FNP-BC: Board Certified Nurse Practitioner*
Compact Status: Multi-State License: Authorized to Practice in 40 States*
Graduate with Honors: ICHS: MSN-FNP (Family Nurse Practitioner Program)
Degree Granted. Master's in Family Practice MSN Diploma (Cum Laude)
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
(Board Certified: Family Practice Nurse Practitioner—Multistate)*
(Licensed Nurse Practitioner & Chiropractor - Multistate)*
Clinical Director
Digital Business Card
Dr. Maria Cardenas, MD
(Board Certified: Internal Medicine)
(Licensed Medical Doctor)
Medical Director, Clinical Director & Collaborative Physician
NPI # 1164426749
MD License #: J2933
Licenses and Board Certifications:
MD: Medical Doctor
DC: Doctor of Chiropractic
APRNP: Advanced Practice Registered Nurse
FNP-BC: Family Practice Specialization (Multi-State Board Certified)
RN: Registered Nurse (Multi-State Compact License)
CFMP: Certified Functional Medicine Provider
MSN-FNP: Master of Science in Family Practice Medicine
MSACP: Master of Science in Advanced Clinical Practice
IFMCP: Institute of Functional Medicine
CCST: Certified Chiropractic Spinal Trauma
ATN: Advanced Translational Neutrogenomics
Memberships & Associations:
TCA: Texas Chiropractic Association: Member ID: 104311
AANP: American Association of Nurse Practitioners: Member ID: 2198960
ANA: American Nurse Association: Member ID: 06458222 (District TX01)
TNA: Texas Nurse Association: Member ID: 06458222
NPI: 1205907805
| Primary Taxonomy | Selected Taxonomy | State | License Number |
|---|---|---|---|
| No | 111N00000X - Chiropractor | NM | DC2182 |
| Yes | 111N00000X - Chiropractor | TX | DC5807 |
| Yes | 363LF0000X - Nurse Practitioner - Family | TX | 1191402 |
| Yes | 363LF0000X - Nurse Practitioner - Family | FL | 11043890 |
| Yes | 363LF0000X - Nurse Practitioner - Family | CO | C-APN.0105610-C-NP |
| Yes | 363LF0000X - Nurse Practitioner - Family | NY | N25929 |
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
(Board Certified: Family Practice Nurse Practitioner—Multistate)*
(Licensed Nurse Practitioner & Chiropractor - Multistate)*
Clinical Director
Digital Business Card
Dr. Maria Cardenas, MD
(Board Certified: Internal Medicine)*
(Licensed Medical Doctor)*
Medical Director, Clinical Director & Collaborative Physician
NPI # 1164426749
MD License #: J2933