
by Dr Alex Jimenez DC, APRN, FNP-BC, CFMP, IFMCP | Chiropractic, Scoop.it
It�s estimated that 6 � 10 percent of people in the United States have fibromyalgia. This chronic pain disorder impacts millions of men and women of all ages and ethnicities all around the world�but fibromyalgia is decidedly more prevalent in women, as is the case with a number of other pain disorders, such as temperomandibular joint disorder, headache, and irritable bowel syndrome.
Studies in both humans and animals have shown that pain is experienced differently by males and females. In general, females (both animal and human) are more sensitive to experimental pain, and women have more pain-related clinical conditions, including osteoarthritis, rheumatoid arthritis, and fibromyalgia.
In addition, studies have suggested that cultural factors may also play a role. For example, it is generally thought that feeling pain is �okay� or even expected among women, and that an emotional response is socially acceptable. On the other hand, traditional male roles in society dictate stoicism in the face of pain, which in turn may translate to an anxious, rather than a depressive, response to pain.
Studies have shown important gender differences in various clinical characteristics of fibromyalgia. For example, women experience significantly more common fatigue, morning fatigue, all-over hurting, irritable bowel syndrome, total and number of symptoms. Women also typically have significantly more tender points. On the other hand, overall pain severity, global severity, and physical functioning are not significantly different between the sexes, nor are such psychologic factors as anxiety, stress, and depression. The mechanisms of gender differences in fibromyalgia are not fully understood, but (as prominent fibromyalgia researcher Dr. Mohamed Yunus states) they are likely to involve interaction between biology, psychology, and sociocultural factors.
While female hormones (i.e. estrogen and progesterone) are primarily thought of in terms of the role they play in reproduction, they also have be shown to have profound effects on the central nervous system and, consequently, on pain. However, the data are mixed as to what those effects are with regard to pain, especially for estrogen. In general, estrogen is excitatory to the central nervous system�so much so that some with seizure disorders have a worsening of symptoms at the time in their menstrual cycles when estrogen is highest, a condition known as �catamenial seizures.�
Conversely, progesterone inhibits the activity of the central nervous system. The effect of different hormone levels on pain may be then be analogous to their effect on mood: having too much of one or too little of the other can produce a problem. Too much estrogen could spell hyperactivity of pain-related nerves or brain areas, while too little could result in a failure to activate areas of the brain that are part of the natural pain-control system. Part of our problem with understanding the role of hormones is that the science of gender�s effects on the biology of pain is still in its infancy.
Many women also experience variations in pain levels throughout their menstrual cycles. It seems likely, then, that female hormones play a role in pain perception. Some pain conditions vary with the menstrual cycle, for example. Pain thresholds are highest in the follicular phase (low estrogen) and lowest in the luteal phase (high estrogen). Migraine, for instance, is a condition more prevalent in females, which worsens during the menstrual cycle and improves post-menopause. Likewise, migraines often improve during pregnancy.
Data from the recent NFA-sponsored epidemiology survey indicated that 26.5 percent of female respondents (average age 47.3 years) had never had children as compared with the national average of� approximately 18 percent of women aged 40-44 (i.e. at the end of child-bearing years). The reason for the apparently higher statistic among women with fibromyalgia is unclear. It may be due to choices made as a result of living with chronic debilitating pain, or there may be an as-yet undetermined biological connection.
Like other so-called �invisible disorders,� fibromyalgia poses a challenge beyond symptom management to those who are diagnosed with it: the struggle for credibility. It is all too easy for those who have not suffered the pain of fibromyalgia to dismiss it since it offers no visible signs; and it has been, unfortunately, all too easy for healthcare providers to dismiss the symptom descriptions of people with fibromyalgia since there is, for instance, no blood test that can reveal whether or not a person has it. A recent�New York Times�article brought this challenge to the fore with its very headline: �Drug Approved. Is Disease Real?� (Jan. 14, 2008).
Fortunately, research results are demonstrating that fibromyalgia is all too real�and the proof is easy for even the most adamant disbelievers to see. MRIs show differences in the brains of people with fibromyalgia compared to the brains of people who do not have the chronic pain disorder, for instance.
Awareness of fibromyalgia has grown dramatically in the general public, the media, and the medical community over the last 10 years, but much work remains to be done.
Those who have been diagnosed with fibromyalgia can do their part by educating their friends, family, colleagues, and supervisors about this chronic pain disorder, the millions of Americans it impacts, the symptoms they strive to manage, and what they require in the way of support from their loved ones.
Sourced through Scoop.it from: www.fmaware.org
Among the wide number of individuals diagnosed with fibromyalgia, women most frequently develop the condition than men. Several research studies have been conducted to attempt to better understand this painful condition. Various studies have concluded that women perceive symptoms of pain different than men, therefore, making them more susceptible to developing fibromyalgia.
For more information, please feel free to ask Dr. Jimenez or contact us at 915-850-0900 .

by Dr Alex Jimenez DC, APRN, FNP-BC, CFMP, IFMCP | Chiropractic, Scoop.it
Learn about living with fibromyalgia and the lifestyle changes that may help you find chronic, widespread pain relief.
Life with fibromyalgia can be a challenge. But you can take steps to proactively manage your health�and your life. Action is empowering.
Your doctor is your most important resource. Work closely with your doctor and talk about which steps might help you find fibromyalgia pain relief. You have options such as lifestyle changes, support groups, and medication.
A healthy and active lifestyle may help you decrease your fibromyalgia symptoms. Studies show that second to medication, the actions most likely to help are light aerobic exercises (such as walking or water exercise to get your heart rate up) and strength training. But always check with your doctor before you start any exercise program.
These tips from the National Fibromyalgia Association may help you get started.
- Start slow. If you’re moving more today than yesterday, that’s progress
- Listen closely to your body. It’s important not to overdo it. Don�t increase your activity too quickly
- Start with just a few minutes of gentle exercise a day. Then work your way up
- Walking is a great form of exercise
- Track your progress. Note the exercise you’re doing and how you feel both during and afterward
- Stretch your muscles before and after exercise
- Post-exercise soreness will decrease over time. But respond to your body’s signals and pace yourself
If you find that you are sleeping poorly, you’re not alone. With fibro, pain and poor sleep happen in a circle. Each worsens the other. Fortunately, there is a lot you can do to help yourself sleep better. The National Fibromyalgia Association, the National Pain Foundation, the National Sleep Foundation, and other expert organizations recommend the following steps to help people sleep:
- Stick to a sleep schedule. If you go to bed at the same time every night, your body will get used to falling asleep at that time. So choose a time and stay with it, even on weekends
- Keep it cool. When a room is too warm, people wake up more often and sleep less deeply. According to the National Sleep Foundation, studies show that you’re likely to sleep better in a room that’s on the cool side. So try turning down the thermostat and/or keeping a fan on hand
- As evening approaches, cut out the caffeine. Caffeine has a wake-up effect that lasts. It’s best to avoid it well before bedtime. That includes not just coffee, but also tea, colas, and/or chocolate
- Avoid alcohol before bed. That �nightcap� may make you sleepy at first. But as your blood alcohol levels drop, it has the opposite effect. You may find yourself wide awake
- Exercise in the afternoon. Afternoon exercise may help you sleep more deeply. But exercising before bedtime can make it harder to fall asleep
- Nap if you need to, but be brief. If you’re so tired that you must take a nap, set the alarm for 20 minutes. Snooze any longer and you may have trouble falling asleep at night
- Make your room a relaxing refuge. Treat yourself to comfortable bedclothes and snuggly pajamas. A white-noise machine or fan may help you fall asleep to a soothing background sound
- Develop a relaxing bedtime routine. Reading helps some people fall asleep. So does listening to soft music. Do whatever works for you. But try to follow the same routine every night to signal your body that it’s time for sleep
So what about your diet? There�s a lot of information on the Internet about �fibromyalgia diets.� But many researchers say there is no perfect eating plan for fibromyalgia relief. Talk to your doctor about what is right for your needs and your lifestyle. Let your doctor know if you have eliminated any foods from your diet. Also, be sure to tell your doctor if you are taking any nutritional supplements. They can possibly interact with any medications you may be taking.
Learning to cope with fibromyalgia can be a challenge. Good emotional support can help. Try reaching out to family and friends. Talk to your loved ones about how to help give you fibromyalgia support.
It�s also important to work closely with a health care professional who understands your condition.
However, fibromyalgia can be hard to understand. Your friends and family may not always know what you are going through. Even members of the health care system may not be as sensitive as you may wish. Maybe the support you need has been lacking.
There are certain feelings, frustrations, and successes that only someone else with fibromyalgia can identify with. Reach out to others who have walked in your shoes. Let your loved ones and others with fibromyalgia help you along the way.
Support groups exist all over the country, as well as online.
- Support groups can help you connect to others who have the chronic widespread pain of fibromyalgia
- You can also learn more about fibromyalgia
- You can get ideas about ways to manage it and become closer to your friends and family
All of this may help you better manage your fibromyalgia.
Another helpful skill is stress management. Stress plays a big role in how you respond to different situations, both physically and emotionally. Stress can have a significant impact on your ability to do the things that are important to you.
There are many different stress management techniques to try that are easy to learn such as
- Meditation
- Deep breathing
- Visualization exercises
You can also simply allow yourself time each day to relax. That may mean learning how to say no without feeling guilty. But it’s important to stay active and keep to a routine you can manage.
A type of therapy called cognitive behavioral therapy has also been found to be helpful. Studies show it can reduce pain severity and improve function. Cognitive behavioral therapy helps us see how our thoughts affect how we feel and what we do.
Sourced through Scoop.it from: www.fibrocenter.com
Fibromyalgia is a condition which causes widespread symptoms of pain and fatigue and, because there is no known cure for it, living with the painful condition can be difficult. However, certain lifestyle changes, including exercise, sleep and nutritional habits can help manage the symptoms and reduce their effect.
For more information, please feel free to ask Dr. Jimenez or contact us at 915-850-0900 .

by Dr Alex Jimenez DC, APRN, FNP-BC, CFMP, IFMCP | Chiropractic, Scoop.it
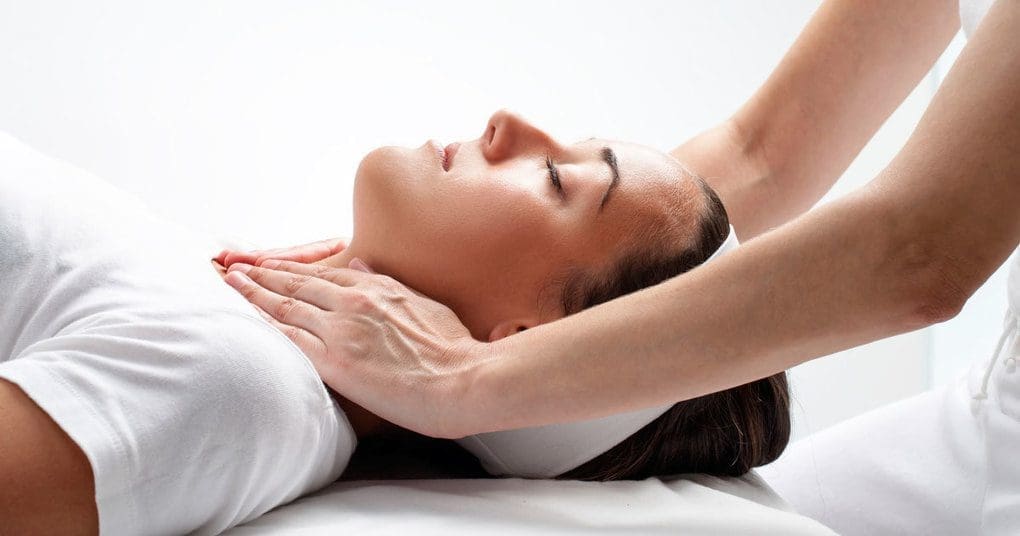
One of the main symptoms of fibromyalgia is sensitivity to touch, but believe it or not, fibromyalgia massage can still be part of your treatment plan.
One of the main symptoms of fibromyalgia is extreme sensitivity to touch, so it�s understandable that some people with fibromyalgia avoid getting massages. However, they are missing out on something great.
Massage might seem like the very opposite approach to take for fibromyalgia pain, but the right amount of pressure and manipulation can actually do a lot for your congested muscles and tissues. In reality, massage is a perfect natural remedy for fibromyalgia. Therapeutic kneading will stimulate blood flow, eliminate metabolic waste, and lengthen muscle fibers. The right fibromyalgia massage will work within the limits of your condition to release pockets of tension, and improve your physical wellbeing and quality of life.
Recommended Fibromyalgia Massage
There are many types of therapeutic massage, and the right style for your fibromyalgia pain will respect your muscle sensitivity and particular pain issues. Stick with these massage techniques for the most healing benefits:
- Swedish massage techniques. This classic relaxation technique ��using the hands, arms or mechanical means ��will gently manipulate tense muscles to relieve long-standing tension.
- Myofascial release. Focusing on the connective tissue called fascia, this technique aims to release pressure where the tissues connect to the bones. Muscles will relax and lengthen, leaving more space for the organs to expand.
- Reflexology. A safe and gentle approach that stimulates points on the hands and feet that are believed to be connected to various organs and tissues. This may help to relax certain areas that would be difficult to stimulate directly.
- Cranial-sacral therapy (CST). Using very mild pressure on strategic points at the base of the skull and along the length of the spine, the CST therapist can detect interruptions in the flow of spinal fluid, and improve the balance and function of every muscle area.
Massages to Avoid
The types of massage that are out of the question if you don�t like touch because of sensitivity include:
- Thai massage. It puts you through different poses for an entire hour.
- Reflexology foot massage. Presses on reflexology points that often hurt.
- Barefoot massage. The massage therapist walks on your back while holding onto a supportive rack suspended from the ceiling.
- Rolfing/structural integration. You�ll feel beat up with this one.
Before proceeding with any fibromyalgia massage, be sure to consult a healthcare professional who has properly diagnosed your condition and who has recommended you to follow up with any of the above mentioned therapies. Preventing further aggravation of any type of symptoms is best to promote a healthier lifestyle and improve overall symptoms.
Sourced through Scoop.it from: fibromyalgia.newlifeoutlook.com
While fibromyalgia has been known to cause symptoms of chronic pain, many individuals with the condition avoid massage or other forms of similar treatment to avoid aggravating their symptoms. However, massage therapy performed by a qualified healthcare professional can not only be beneficial, it can help reduce and manage the pain caused by fibromyalgia.
For more information, please feel free to ask Dr. Jimenez or contact us at 915-850-0900 .

by Dr Alex Jimenez DC, APRN, FNP-BC, CFMP, IFMCP | Chiropractic, Scoop.it
Many patients are labeled with fibromyalgia simply because they have chronic soft tissue pain. But it is important, at least for the sake of correctness, that not all chronic soft tissue pain be called fibromyalgia.
In fact, localized or regional pain is often due to myofascial pain syndrome (MPS), a rather common condition which affects certain muscle areas. MPS is often present in the fibromyalgia patient, but not all MPS patients also suffer from fibromyalgia.
MPS generally involves pain in the neck, shoulders, hips, back, jaw and head. This pain is often accompanied by stiffness or tightness. It is important that the doctor listen to the patient to learn where the pain is most intense. And because MPS is not diagnosed with a lab test or x-ray, it is important that the doctor carefully examine the patient.
Trauma is a common cause of MPS, in the form of muscle strain or ligament and tendon sprain; or as a result of chronic trauma due to repetitive work injury, or altered posture due to poor exercise. An example of the former is whiplash from an auto accident. An example of the latter is an individual who works at a computer all day, and subsequently develops MPS involving the muscles of the upper back and shoulders; such individuals often develop tension headaches. Of course, more than one area may be involved, and this can make distinguishing between MPS and fibromyalgia all the more difficult.
MPS can occur with a variety of medical problems, including spinal disc disease, or inflammatory illnesses. And like fibromyalgia, MPS symptoms can be made worse due to stress, depression, anxiety, fatigue and vitamin deficiencies, to name a few.
It is important for the doctor to identify all other illnesses in an individual patient so that therapy can be most effective and accurate.
As there is no cure for fibromyalgia, so there is no cure for MPS. The goals of treatment should obviously include pain relief and improvement/restoration of mobility and functionality. It is important to identify any other accompanying conditions, and give treatment to these also. Perhaps most importantly, the patient needs to be educated on how to best manage chronic pain, so that life can be lived as normally as possible.
The key differences between these two chronic pain syndromes:
1. MPS has more localized or regional pain versus the diffuse pain of fibromyalgia.
2. MPS patients have “trigger points” which can cause pain at a distant location when pressed, whereas fibromyalgia patients suffer from “tender points”.
3. MPS has a better prognosis, as the pain often resolves with treatment or the rectification of the offending stimulus (such as the ergonomically incorrect office desk); the pain of fibromyalgia has a much higher chance of being chronic.
Unfortunately, many individuals are misdiagnosed with either myofascial pain syndrome or fibromyalgia. Therefore, it’s absolutely essential for the individual experiencing widespread symptoms of pain and fatigue, to seek professional help and follow through with the proper assessments to determine which of these two similar conditions, the individual has developed, in order to properly treat them.
Sourced through Scoop.it from: www.psychologytoday.com
Many people are diagnosed with fibromyalgia after reporting symptoms of chronic pain, however, it’s safe to say that not all widespread pain could indicate the presence of this painful condition. In fact, myofascial pain syndrome is another condition, frequently misdiagnosed as fibromyalgia.
For more information, please feel free to ask Dr. Jimenez or contact us at 915-850-0900 .

by Dr Alex Jimenez DC, APRN, FNP-BC, CFMP, IFMCP | Chiropractic, Scoop.it
Fibromyalgia symptoms like numbness, tingling, and pain can be tied to your environment. Learn how pain can be affected by reactions to light, sound, or smell.
Sensitivity to environmental stimulation, including bright lights, loud noises, and even certain smells, can make living with fibromyalgia particularly challenging. You might wake up each morning wondering what new trigger may exacerbate your fibromyalgia symptoms.
“I deal with everything on a day-to-day basis,” says Stephanie Parker of Dover, Del., who believes her symptoms are consistent with fibromyalgia but has not yet been formally diagnosed. The symptoms keep her from participating in daily family activities, such as watching her kids’ ballgames in the afternoons.
Tina Pringle, who was diagnosed 16 years ago with fibromyalgia, says that her fibromyalgia symptoms have been overwhelming at times. “The symptoms all merge together, and because of the fatigue and brain fog, everything becomes a maze of sheer confusion,” explains Pringle.
This heightened sensitivity may be difficult for you to understand, much less explain to friends and family members who see no outward problem. The uncomfortable and painful sensations of fibromyalgia may be part of your brain’s unusual way of processing pain, suggests fibromyalgia researcher Benjamin Natelson, MD, a neurology professor at the Albert Einstein College of Medicine in New York City and author of Your Symptoms Are Real: What to Do When Your Doctor Says Nothing Is Wrong.
According to a study published in the Archives of Physical Medicine and Rehabilitation�that compared and analyzed reports from women with rheumatoid arthritis, women with fibromyalgia, and women without a pain syndrome, those with fibromyalgia were much more likely to report intense, unpleasant responses to sounds, smells, tastes, and tactile sensations.
Another study, published in the journal Pain Research and Treatment,suggests that changes in brain chemistry among people with fibromyalgia may be linked to sensitivity to stimuli such as sound and smell. Imaging studies have provided visual depictions of this altered response to sensations. In some respects, the brains of people with fibromyalgia may be hyper-responsive to even the possibility of pain or discomfort, Dr. Natelson says.
Researchers have also tested tissue samples and found elevated levels of inflammatory markers in the skin of people with fibromyalgia � which may be linked to hypersensitivity to touch. Touch sensitivity is real for people like Pringle, who says that there are times when even holding hands with her partner is too painful to bear. Clothes that are too tight, massages, and even light touches all ratchet up her pain and stress. To make matters worse, Pringle says she occasionally even flinches involuntarily when touched by others, which can be hurtful to those around her.
Sourced through Scoop.it from: www.everydayhealth.com
Widespread pain and fatigue are well-known symptoms associated with fibromyalgia, however, recent studies have concluded that an individual’s symptoms can also be tied to their environment, including reactions to light, sound or smell. Sensory overload can be an additional symptom to fibromyalgia.
For more information, please feel free to ask Dr. Jimenez or contact us at 915-850-0900 .
by Dr Alex Jimenez DC, APRN, FNP-BC, CFMP, IFMCP | Chiropractic, Scoop.it
Some patients fear that chiropractic care for fibromyalgia may aggravate pain. But it is both safe and proven to reduce pain from fibromyalgia.
Chiropractic Care for Fibromyalgia: Does It Work?
Many fibromyalgia patients seek natural treatment for fibromyalgia, and chiropractic care is one of the most frequently considered, especially for pain management and to improve the range of motion of joints.
This form of medicine is based on the principle that the body has the ability to self-heal and recover from a disease. The nervous system runs between the spine and carries messages from the brain to every cell of the body.
When the vertebrae are restricted, locked or misaligned there will be pressure on the nerves and symptoms will occur. For this reason, a chiropractor will perform �adjustments� using gentle pressure, stretching or certain high velocity thrusts to bring the vertebrae to optimal position and restore health.
Research Studies on Chiropractic Care for Fibromyalgia
A study conducted in a chiropractic clinic in Canada revealed that 30�chiropractic treatments can improve pain by up to 77 percent, the quality of sleep by 63 percent and decrease fatigue by almost 75 percent. Positive findings had been recorded in a small, preliminary study (also performed in Canada) with documented improvements in joint mobility pain intensity while using various chiropractic techniques such as spinal manipulation, stretching and soft tissue therapy.
A review of several research studies, including eight systematic reviews and three meta-analyses that assessed the benefits of alternative medicine for fibromyalgia was published in 2009 in the Journal of Manipulative Physiology and Therapeutics. According to this systematic review, there is some evidence that spinal manipulation, diet and vitamins can help manage fibromyalgia, although more scientific evidence supported the use of exercise, psychotherapy massage, acupuncture and spa therapy (hydro therapy) for this condition.
Special Considerations
Some people may fear fibromyalgia chiropractic adjustments may trigger�the pain. Overall, this form of therapy has a good safety profile and patients receiving adjustments are satisfied with the results.
In some cases, adjustments may cause aggravation of the symptoms (including pain) for a brief period of time.
If you experience pain or any other symptoms after chiropractic adjustments, talk to the doctor to possibly change the therapy (these adjustments can be performed in several ways, some being gentler than others).
If you don�t achieve symptom improvement following the recommended set of treatments, you may need to change or add other modalities (some chiropractors are also trained in acupuncture, naturopathy or homeopathy).
You should not seek spinal manipulation if you suffer from osteoporosis, spinal cord compression, inflammatory arthritis (i.e. lupus, rheumatoid arthritis). If you have cancer, you should also talk to your MD first before using chiropractic care.
Otherwise, if you are looking to better control fibromyalgia symptoms, it�s worth considering this form of therapy. In addition, try to improve your lifestyle; eat a healthy, balanced diet, exercise regularly and practice stress management techniques.
Sourced through Scoop.it from: fibromyalgia.newlifeoutlook.com
Chiropractic care is alternative, treatment option for various types of injuries or conditions. It’s been long used to help individuals find relief from their symptoms and recent studies have concluded, chiropractic treatment can be beneficial towards treating people with fibromyalgia, a widespread chronic pain condition.
For more information, please feel free to ask Dr. Jimenez or contact us at 915-850-0900�.

by Dr Alex Jimenez DC, APRN, FNP-BC, CFMP, IFMCP | Chiropractic
Fibromyalgia, a chronic disease that causes pain and swelling in more than a dozen points all over the body, affects as many as 5 million people. Because doctors are still unsure of the cause of fibromyalgia, treatment can be frustrating (and often a process of trial and error).
�Fibromyalgia symptoms are only about 30% amenable to current pharmaceutical strategies on the market,� says Kathleen Holton, PhD, MPH, lead author of Potential Dietary Links in Central Sensitization in Fibromyalgia.
That�s why many patients are taking matters into their own hands and experimenting with alternative treatments, including dietary changes. Forty-two percent of fibro patients reported that symptoms worsened after eating certain foods, and though much of the research is in its preliminary phases, there�s some evidence that simple diet tweaks may ease fibro pain.
Read on to get 5 food rules for fibromyalgia patients (just be sure to consult your doctor before drastically changing your diet).
Load up on vitamin D
Many adults are deficient in vitamin D�to begin with, but this sunshine vitamin can be vital to fibro patients. “Vitamin D deficiency can mimic some of the symptoms of fibromyalgia. All patients should be screened for deficiency,” says Holton. Studies show that vitamin D deficiencies can cause bone and muscle pain, and upping levels of this hard-to-get vitamin may help. A 2008 study found that pain patients with low levels ofvitamin D required almost double the dose of painkillers as those with adequate levels. Holton recommends taking a supplement, especially during the wintertime.
Avoid additives
Common food additives, like monosodium glutamate (MSG) and aspartame, can act as excitotoxin molecules, a chemical group that has the ability to activate neurons that increase sensitivity to pain. Anecdotally, easing off these additives can help, and one very small study of four patients found that eliminating MSG and aspartame resulted in a reduction of fibromyalgia symptoms. The research is far from definitive, but it may be worth trying if you notice your symptoms worsen after Chinese takeout or too many diet drinks.
Say yes to fish
Omega-3 fatty acids, found in fatty fish, like salmon, walnuts, and flaxseed, are known to reduce inflammation and help prevent cardiovascular diseases. However, their soreness-reducing traits may also help pain patients. A 2007 study found that after just 3 months of supplementing omega-3 fatty acids, symptoms such as morning stiffness and painful, tender joints decreased. Though this study did not include fibromyalgia patients (it included rheumatoid arthritis (RA), irritable bowel syndrome (IBD), and dysmenorrheal patients), the results show promise. Fibro patients often have co-morbidities such as IBD and RA, so omega-3s may benefit them as well. Try adding salmon or walnuts to your diet, or, if you don�t like those foods, try adding flaxseeds to your cereal or oatmeal.
Nix the caffeine
Because sleeplessness is commonly associated with fibro, it may be tempting to fuel up on coffee to get through the day. This, however, may be a mistake. “Some patients use caffeine to compensate for not sleeping well, which can lead to a circular problem where the �solution� of taking caffeine to stay awake is actually causing the problem of not sleeping at night,” says Holton. Caffeine can set you up for a crash and, if sipped later in the day, may disrupt sleep schedules. Holton recommends antioxidant-packed decaffeinated green tea as a healthier alternative.
Veg out
Some researchers speculate that oxidative stress may be a cause of fibro symptoms. Oxidative stress occurs when the body doesn�t produce enough antioxidants to battle cell-damaging free radicals in the body. Most fruits and veggies are packed with important antioxidants, like vitamins A, C, and E, which fight free radicals to keep your body normalized. Certain studies also show a raw, vegan diet can improve symptoms, but that�s difficult for most people to follow. If you do choose to eat meat, though, opt for a small portion of grass-fed beef. “It is an excellent source of iron and vitamin B12, both nutrients which are extremely important in keeping your pain-processing nervous system healthy,” says Holton.
Sourced through Scoop.it from: www.prevention.com
Fibromyalgia can cause symptoms of pain and discomfort along with fatigue and concentration issues. Living with the condition can be difficult, however, there are many alternative treatment options, such as chiropractic, which can help people with the condition, find relief from their symptoms. In addition, following a balanced diet and the proper nutrition can help speed up the process of relief.
For more information, please feel free to ask Dr. Jimenez or contact us at 915-850-0900 .�















