Contents
Introduction
Dr. Jimenez, D.C., presents what you need to know about venous insufficiency. Many factors and lifestyle habits cause an effect on our bodies, which can lead to chronic disorders that can impact our musculoskeletal system and potentially lead to pain-like symptoms associated with chronic conditions. In this presentation, we will look at what venous insufficiency is, the symptoms, and how to prevent venous insufficiency from affecting the lower extremities. We mention our patients to certified medical providers that provide available therapy treatments for individuals suffering from chronic conditions associated with Lyme disease. We encourage each patient when it is appropriate by referring them to associated medical providers based on their diagnosis or needs. We understand and accept that education is a marvelous way when asking our providers crucial questions at the patient’s request and acknowledgment. Dr. Alex Jimenez, D.C., uses this information as an educational service. Disclaimer
What Is The Venous System?
Dr. Alex Jimenez, D.C., presents: So we will go over tackling common cardiovascular problems and venous insufficiency. So let’s discuss this common complication in our practices: venous insufficiency and the functional medicine approach. So if you look at venous or blood flow, you look at the heart. The heart will pump blood to the arteries and the arterials, the arteries and arterials will pump to capillary beds, and venules will go to veins. Veins will then move the blood to the subclavian vein, and the lymph ducts will also drain in the subclavian vein.
The subclavian vein will then go into the heart, and in the process, it continues and circulates. The big difference between veins and arteries is that arteries have muscles within them, and the muscles will contract, regulate blood pressure, and help keep the blood flowing. But veins do not have that luxury. Veins will depend on our skeletal muscles around them; if we contract them a lot, we’re helping with circulation. So, being active, moving around, and flexing our muscles will keep the pressure in the superficial system to about 20 to 30. And then, when it starts going to the deeper system with the valves, what happens is that the valves will stop blood from flowing back. So the blood can only go in one direction.
And that is basically to have a healthy venous system. You want to be often exercising, and you want to have that higher venous pressure and flow. So what is the pathophysiology of chronic venous insufficiency? You have incompetent valves, or you can have incompetent valves, you can have thrombosis, and you can have obstruction. And that can lead to elevated venous pressure. High venous pressure can lead to vein dilation, skin changes, and ulceration, but also elevated venous pressure can worsen incompetent valves, thrombosis, and obstruction. And then you get this vicious cycle, and usually, it’s the lower extremities; they get worse and worse. So if you want to look at the contributing factors, look at the functional medicine matrix. Venous insufficiency pathogenesis hits many places on the functional medicine matrix, multiple places we can look at in the lower body extremities.
Venous Insufficiency & Its Signs
Dr. Alex Jimenez, D.C., presents: So what are the clinical manifestations of venous insufficiency? The symptoms are limb itching, heaviness, fatigue, particularly in the legs, pain in the legs, swelling, and tightness. The skin can get dry and become irritated. You might not be dealing with autoimmunity if you have this dry, irritated skin. You might be dealing with venous insufficiency. They can get muscle cramps. So your muscle cramps might not be a magnesium deficiency. Your muscle cramps might be venous insufficiency pain worse when standing or seated with their legs dangling. So when you’re sitting, the legs are dangling, and the pain improves when you elevate your legs and walk. And that actually can differentiate from arterial insufficiency. Remember, you get claudication in peripheral artery disease and arterial insufficiency. That’s when you walk and exert yourself. And because the blood vessels going to the muscles and the legs are tighter because of atherosclerosis, you get pain from walking.
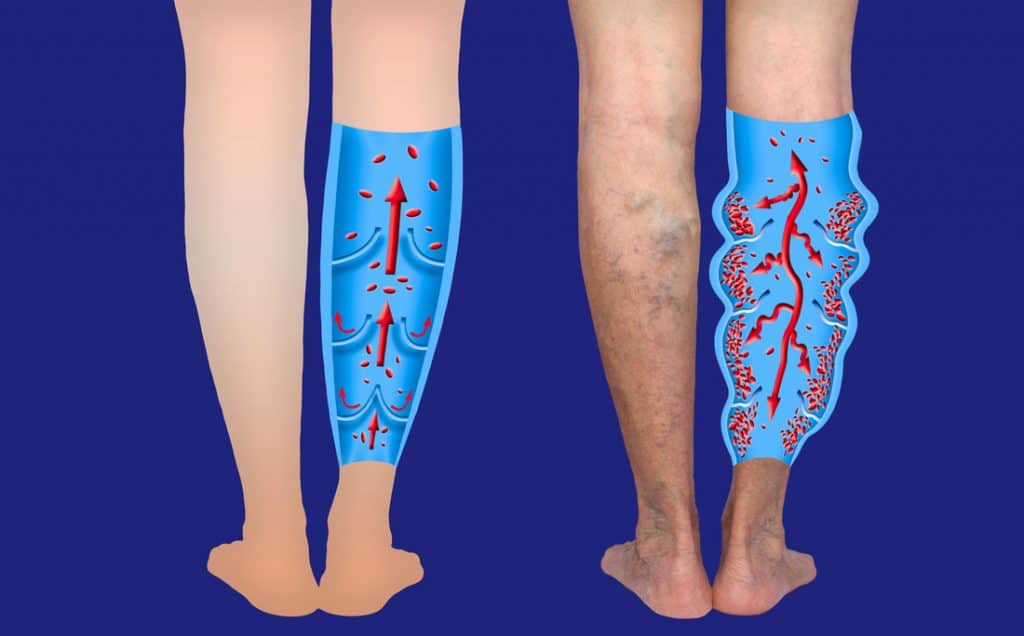
Whereas venous insufficiency is the other side of the system, you walk and start feeling better. Why? Because those muscles are pumping the veins and moving blood through instead of the blood just being stagnant and sitting there. So edema you can get, which is swelling. Stasis dermatitis, which is dermatitis, red and swelling, and inflamed varicose veins, can be seen in this picture. Now the diagnosis is usually made by clinical signs and symptoms. So the clinical signs, what are the signs to look out for? For this part, go to your favorite search engine and look up every one of these symptoms that we mentioned so you know what it looks like. We are sure you’ve seen it before, but remind yourself what these things look like so that it can help you; it can help you when you’re diagnosing and looking at your patients.
Lymphodematosclerosis
Dr. Alex Jimenez, D.C., presents: Suppose a person has varicose veins. You can have lymphodematosclerosis, which is the champagne bottle sign. When you search that, look at that and see how the leg will look like an upside-down champagne bottle. Why? Because there’s a lot of fibrosis and hard tissue, and that tissue is holding that blood. You can’t get much edema, and you can’t get much swelling because it’s so tight, the blood can’t move in there. So look up the champagne bottle, not just the regular one, but look up a champagne bottle or lymphodematosclerosis, and you will remember that image when you see it. Then you will remember that image. You can get ulcerations because there’s decreased blood movement. So you get ulcers, and you can get hyperpigmentation. We see this often when you have a darkened skin color in the lower extremities from the constant fluid or blood leaking.
That’s hemosiderin deposits or iron deposits from popping blood cells. And you can get skin atrophy. So by typing these clinical signs on the internet that correlate with venous insufficiency, you have a good visual of what these things look like. So what is the functional medicine treatment plan? We’re going to look at the risk factors of chronic venous insufficiency, and we’re going to look at the adaptable ones, and based on that, we can give patients recommendations and plans. So obesity works on decreasing fat, sedentary life, being active, checking estrogen and hormone levels, and reducing estrogen and increasing progesterone. If you have to get out of that estrogen dominance, we want to look at those risk factors, see which ones are adjustable, and start working with them.
Ways To Reduce Venous Insufficiency
Dr. Alex Jimenez, D.C., presents: So you have this person with venous insufficiency. Check on their obesity levels, so you work on lowering their body fat and see if they have a sedentary lifestyle and getting them moving high. Check their hormone levels and see where their estrogen levels are regulated. If you check the IFM hormone module, check it out because it has some really good information on how to balance hormones in a functional medicine way. Make sure that they’re standing for a short period. At least occasionally, have them walk around, and you can have them set a timer. So every so often, every 20, 30 minutes, they walk around to keep their legs and blood flow moving. Work on decreasing smoking. And mentioning these risk factors to the patient can make them aware that this can worsen their venous insufficiency. Other conservative therapies include leg elevation. So have them lay down by putting their legs up to allow gravity to help push the blood down. Compression therapy. So have them wear compression stockings and stasis dermatitis; sometimes, you must use topical dermatologic steroids and some of those agents, which can be helpful there.
You may consider earthing. There was a research study that showed that if you put your feet on the ground outside barefoot, not in the insulated houses, then what can happen is, is the viscosity of your red blood cells will decrease. So the red blood cells will clump less, and you can have better movement and circulation. Pharmacological therapies and supplementations to target venous insufficiency. So what can we do while we’re looking at doing two things? We want the venous tone to be improved. So you want to tighten those veins up. On the arteries, you want to loosen them up. Usually, when an individual has hypertension, we want the veins to tighten those bad boys up so that circulation can happen. And then you want to improve the flow. You want the blood to be able to flow through the veins better.
Supplements For Venous Tone
Dr. Alex Jimenez, D.C., presents: So let’s take a look at the venous tone. This is one of the places where we’re ahead of the game in functional and integrative medicine because if you look at the conventional literature, even up-to-date research, many people are using up-to-date now to see how often they diagnose weak venous tone. So we can take a look at that. But if you look at what you can do for venous tone? It has two supplements. Regarding venous tone and increasing venous tone, two supplements can support the venous system: horse-chestnut seed extract (Escin) and diosmin.
So those are the two things that are mentioned. And we, in functional and integrative medicine, are more prepared to deal with this because we know about pharmacy grade; we learn about giving them a good product that is third-party tested and doesn’t have those toxic fillers and whatnot. The second way of treating venous insufficiency from a medical point of view is by improving venous flow. You want blood viscosity to be thinner. You don’t want the blood not to be as prone to clotting so the blood can flow easier. So here are some agents you can use. You can use aspirin; you can use pentoxifying; you can use nattokinase, which can help lower fibrinogen. Regarding venous insufficiency, it can cause the body to have high fibrinogen. So nattokinase can help lower elevated fibrinogen.
Conclusion
Dr. Alex Jimenez, D.C., presents: If they’re not on aspirin or any blood thinners and have high fibrinogen and venous insufficiency, it might also be a good one to put somebody on omega-3s. We are trying to get their omega-3 levels up, and they are useful when optimizing help with venous flow. You’re going to have people to come and see you, and you’re going to be treating them for other things. And because you’re functional medicine, you’re part of the cool club; what’s going to happen is they’re not even going to tell you about their venous insufficiency, and it’s going to get better just because of the treatments that you’re doing. And it will be epic. And if all else fails, you refer to associated medical specialists to help your patient. So, in conclusion, take care of your veins and look for the signs to prevent venous insufficiency from causing more issues in the lower extremities, and utilize vitamins and supplements to reduce the pain and inflammation in the muscles and joints.
Disclaimer
General Disclaimer, Licenses and Board Certifications *
Professional Scope of Practice *
The information herein on "What You Need To Know About Venous Insufficiency" is not intended to replace a one-on-one relationship with a qualified health care professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional.
Blog Information & Scope Discussions
Welcome to El Paso's Premier Wellness and Injury Care Clinic & Wellness Blog, where Dr. Alex Jimenez, DC, FNP-C, a Multi-State board-certified Family Practice Nurse Practitioner (FNP-BC) and Chiropractor (DC), presents insights on how our multidisciplinary team is dedicated to holistic healing and personalized care. Our practice aligns with evidence-based treatment protocols inspired by integrative medicine principles, similar to those on this site and on our family practice-based chiromed.com site, focusing on naturally restoring health for patients of all ages.
Our areas of multidisciplinary practice include Wellness & Nutrition, Chronic Pain, Personal Injury, Auto Accident Care, Work Injuries, Back Injury, Low Back Pain, Neck Pain, Migraine Headaches, Sports Injuries, Severe Sciatica, Scoliosis, Complex Herniated Discs, Fibromyalgia, Complex Injuries, Stress Management, Functional Medicine Treatments, and in-scope care protocols.
Our information scope is multidisciplinary, focusing on musculoskeletal and physical medicine, wellness, contributing etiological viscerosomatic disturbances within clinical presentations, associated somato-visceral reflex clinical dynamics, subluxation complexes, sensitive health issues, and functional medicine articles, topics, and discussions.
We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for musculoskeletal injuries or disorders.
Our videos, posts, topics, and insights address clinical matters and issues that are directly or indirectly related to our clinical scope of practice.
Our office has made a reasonable effort to provide supportive citations and has identified relevant research studies that support our posts. We provide copies of supporting research studies upon request to regulatory boards and the public.
We understand that we cover matters that require an additional explanation of how they may assist in a particular care plan or treatment protocol; therefore, to discuss the subject matter above further, please feel free to ask Dr. Alex Jimenez, DC, APRN, FNP-BC, or contact us at 915-850-0900.
We are here to help you and your family.
Blessings
Dr. Alex Jimenez, DC, MSACP, APRN, FNP-BC*, CCST, IFMCP, CFMP, ATN
email: [email protected]
Multidisciplinary Licensing & Board Certifications:
Licensed as a Doctor of Chiropractic (DC) in Texas & New Mexico*
Texas DC License #: TX5807, Verified: TX5807
New Mexico DC License #: NM-DC2182, Verified: NM-DC2182
Multi-State Advanced Practice Registered Nurse (APRN*) in Texas & Multi-States
Multi-state Compact APRN License by Endorsement (42 States)
Texas APRN License #: 1191402, Verified: 1191402 *
Florida APRN License #: 11043890, Verified: APRN11043890 *
Colorado License #: C-APN.0105610-C-NP, Verified: C-APN.0105610-C-NP
New York License #: N25929, Verified N25929
License Verification Link: Nursys License Verifier
* Prescriptive Authority Authorized
ANCC FNP-BC: Board Certified Nurse Practitioner*
Compact Status: Multi-State License: Authorized to Practice in 40 States*
Graduate with Honors: ICHS: MSN-FNP (Family Nurse Practitioner Program)
Degree Granted. Master's in Family Practice MSN Diploma (Cum Laude)
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
My Digital Business Card
Licenses and Board Certifications:
DC: Doctor of Chiropractic
APRNP: Advanced Practice Registered Nurse
FNP-BC: Family Practice Specialization (Multi-State Board Certified)
RN: Registered Nurse (Multi-State Compact License)
CFMP: Certified Functional Medicine Provider
MSN-FNP: Master of Science in Family Practice Medicine
MSACP: Master of Science in Advanced Clinical Practice
IFMCP: Institute of Functional Medicine
CCST: Certified Chiropractic Spinal Trauma
ATN: Advanced Translational Neutrogenomics
Memberships & Associations:
TCA: Texas Chiropractic Association: Member ID: 104311
AANP: American Association of Nurse Practitioners: Member ID: 2198960
ANA: American Nurse Association: Member ID: 06458222 (District TX01)
TNA: Texas Nurse Association: Member ID: 06458222
NPI: 1205907805
| Primary Taxonomy | Selected Taxonomy | State | License Number |
|---|---|---|---|
| No | 111N00000X - Chiropractor | NM | DC2182 |
| Yes | 111N00000X - Chiropractor | TX | DC5807 |
| Yes | 363LF0000X - Nurse Practitioner - Family | TX | 1191402 |
| Yes | 363LF0000X - Nurse Practitioner - Family | FL | 11043890 |
| Yes | 363LF0000X - Nurse Practitioner - Family | CO | C-APN.0105610-C-NP |
| Yes | 363LF0000X - Nurse Practitioner - Family | NY | N25929 |
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
My Digital Business Card