Contents
Evidence-Based Integrative Chiropractic Care for Hip Impingement and Hypermobility in Dancers: Ultrasound-Guided PRP, Rehabilitation, and Stability Strategies
Abstract
In this educational post, I present a comprehensive, step-by-step look at how integrative chiropractic care and targeted physical therapy support dancers with hip impingement, instability, and hypermobility. Using a real-world case of a young dancer with end-range pain and clicking, I explain the role of high-concentration platelet-rich plasma (PRP) delivered under ultrasound guidance to the intra-articular hip, and anchor it within a modern, multimodal care plan: precise manual therapy, neuromuscular control training, kinetic chain strengthening, and load-management strategies. I discuss why hip joints tolerate low-volume biologic injections, how labral irritation differs from labral tears, and why stabilizing the capsule, labrum, and deep rotators is essential for long-term outcomes. Throughout, I synthesize the latest evidence from leading researchers while sharing observations from my clinical practice at El Paso Back Clinic to help athletes return to pain-free performance with durable stability.
Introduction: Framing Hip Impingement and Hypermobility in Dancers
As Dr. Alexander Jimenez, DC, APRN, FNP-BC, CFMP, IFMCP, ATN, CCST, I routinely evaluate dancers and artistic athletes who present with hip impingement, hypermobility, end-range pain, and mechanical clicking. These individuals often possess an extraordinary range of motion, but their joint stability and neuromuscular control can lag behind their flexibility. In this post, I will:
- Clarify the anatomy and pathophysiology of femoroacetabular impingement (FAI), hip instability, and labral irritation.
- Explain why careful, low-volume PRP can be helpful in certain intra-articular hip cases and how ultrasound guidance improves accuracy and safety.
- Detail how integrative chiropractic care and physical therapy anchor recovery through manual therapy, corrective exercise, motor control retraining, and graded load management.
- Present a clear, staged plan for returning a dancer to durable performance while protecting the labrum and capsule.
Clinical Context: A Dancer with Hip Impingement and Hypermobility
The case involves a young dancer with hip impingement, clicking, and pain at end range. She has a history of hypermobility—meaning her passive tissue elasticity and joint laxity are high, but her dynamic control may be insufficient under load or at extreme positions. Ultrasound imaging shows the femoral head centrally, the acetabulum superior-lateral, and the triangular acetabular labrum hugging the joint margin. We have identified irritation and instability without a large labral tear.
Why this matters: Dancers often drive the hip into extremes of flexion, abduction, and external rotation. In FAI, bony morphology (cam or pincer) plus capsulolabral stress can irritate the labrum and capsule. In hypermobile athletes, the capsule may be lax, and repetitive end-range positions can produce shearing and clicking. The labrum acts as a suction seal and stabilizer; when irritated, it can become symptomatic even without a discrete tear.
Key Pathophysiology: Stability, Labrum, and the Capsule
- The acetabular labrum increases the depth of the socket and contributes to joint pressurization—maintaining a negative intra-articular pressure for a “seal” that stabilizes the hip during rotational movements (Nepple et al., 2015).
- The capsule (with ligaments like the iliofemoral ligament) provides passive restraint, especially in extension and external rotation. Hyperlaxity or micro-failure of capsular fibers can allow excessive translation, increasing labral stress (Domb et al., 2013).
- The deep hip rotators (quadratus femoris, gemelli, obturator internus/externus) and gluteus medius/minimus provide dynamic stability, controlling femoral head position during motion. Weakness or delayed activation can lead to excessive femoral internal rotation and adduction, increasing anterosuperior labral load (Lewis & Sahrmann, 2006).
- In FAI, altered bony contours cause abnormal contact between the femoral head-neck junction and the acetabular rim, particularly in flexion with internal rotation. Dancers with hypermobility may paradoxically experience impingement because lax passive structures permit unsafe end-range positioning.
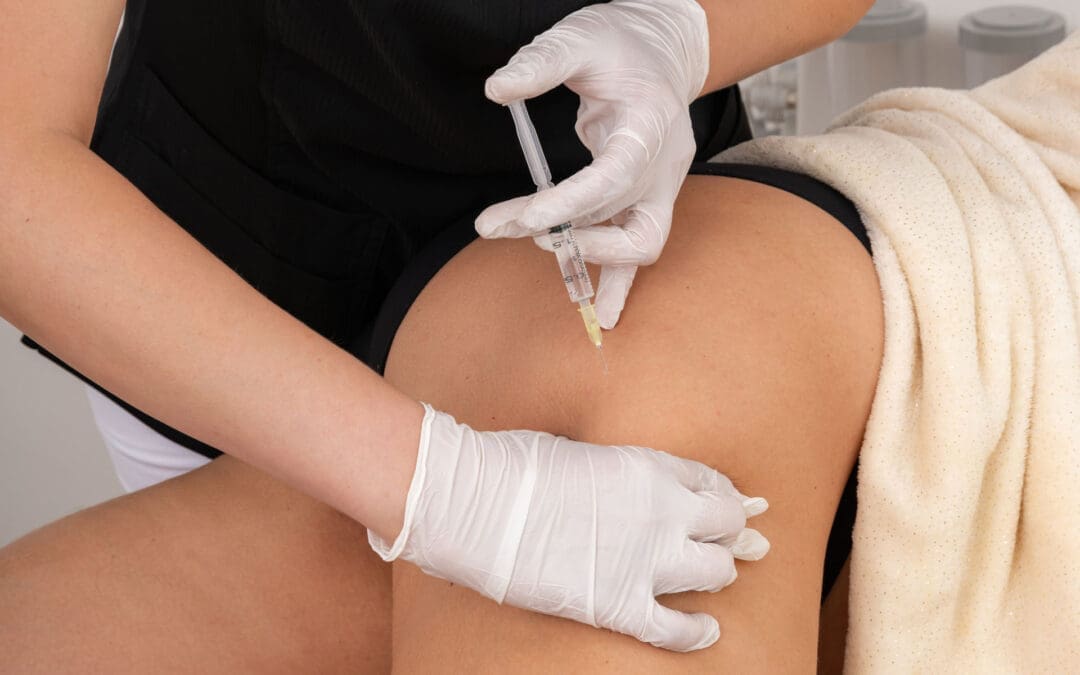
Ultrasound-Guided PRP: Rationale, Technique, and Safety
For this dancer, we delivered a high-concentration PRP solution into the intra-articular space under ultrasound guidance. We used approximately 4 cc of concentrated PRP plus 2 cc of plasma protein concentrate to limit volume while maintaining bioactive content. Hips tolerate less injection volume than knees due to smaller capsular capacity and pressure sensitivity.
Why PRP in this setting:
- Biologic modulation: PRP contains growth factors (e.g., PDGF, TGF-β, VEGF) that may promote healing responses, reduce synovial inflammation, and support matrix homeostasis in the labrum and capsule (Mautner et al., 2015; Fitzpatrick et al., 2017).
- Symptom relief and function: Evidence suggests PRP can reduce pain and improve function in certain chronic tendinopathies and intra-articular conditions; in hips, results are mixed but promising in selected patients, especially when combined with a structured rehab plan (Smith, 2016).
- Stability support: For irritative labral conditions without large tears, PRP may help calm the joint environment, enabling focused rehabilitation on motor control without persistent synovial irritation.
Technique principles emphasized in the procedure:
- Use ultrasound to identify the femoral head, acetabulum, and labrum while avoiding neurovascular structures, such as the femoral artery, medially.
- Maintain visualization of the needle at all times to confirm intra-articular positioning. If injection becomes painful and resistant, reassess to ensure you are not in soft tissue.
- Employ an appropriate needle gauge (e.g., 23-gauge with PRP admixture; 21-gauge for more viscous concentrates) and thoroughly purge air to avoid echogenic artifacts and ensure smooth delivery.
- Limit volume to protect capsular compliance and avoid pressure pain; hips typically do not tolerate large volumes well.
Importantly, PRP is an adjunct—not a stand-alone fix. The outcomes depend heavily on the quality of post-injection rehabilitation focused on stability and movement control.
Integrative Chiropractic Care: Building the Foundation for Hip Stability
At El Paso Back Clinic, our integrative approach blends chiropractic precision with physical therapy and sports rehabilitation. The goals are to:
- Restore optimal joint centration and reduce aberrant motion.
- Enhance neuromuscular control of the pelvis and hip through targeted activation.
- Address regional interdependence—how spine, pelvis, foot, and thorax mechanics influence the hip.
Clinical observations from my practice:
- Dancers with hypermobility often present with rib cage flare, anterior pelvic tilt, and lumbar extension bias. This pattern increases anterior hip joint load and narrows the clearance for hip flexion, exacerbating impingement.
- Correcting breathing mechanics and pelvic positioning reduces hip flexor tone, improves diaphragmatic control, and normalizes intra-abdominal pressure, which stabilizes the lumbopelvic complex.
Manual Therapy: When, Why, and How
Manual therapy in hypermobile hips requires finesse: the aim is not to “loosen” lax joints but to normalize soft-tissue tone, improve joint mechanics, and facilitate motor learning.
- Soft-tissue release for overactive muscles (iliopsoas, TFL, adductors): Reduces anterior shear and internal rotation bias, allowing the deep rotators to engage effectively. We use instrument-assisted techniques and targeted myofascial release to reduce nociceptive drive and guarding (Littlewood et al., 2013).
- Joint mobilization: Low-amplitude, directional-specific mobilizations to improve posterior glide during flexion and enhance congruency without overstressing the capsule. In hypermobility, we avoid high-velocity thrusts directed at already lax segments and prioritize stabilization-oriented mobilizations (Kaltenborn, 2003).
- Pelvic and lumbar adjustments: When segmental restrictions in the SI joint or lumbar spine increase compensatory hip motion, gentle, well-placed adjustments can restore symmetry. We carefully monitor for hypermobility and follow adjustments with stability drills to lock in motor control.
Why this matters physiologically:
- Reducing myofascial tone can decrease abnormal compressive loads and nociceptive input, thereby improving the motor recruitment of stabilizers.
- Improving arthrokinematics supports the labral seal by encouraging even femoral head loading rather than asymmetric rim stress.
Neuromuscular Control: Teaching the Hip to Stabilize
Rehabilitation for dancers hinges on motor control, not just strength. Our plan typically includes:
- Deep rotator activation: Quadratus femoris and obturators provide transverse plane control, limiting excessive femoral internal rotation during flexion. Drills: prone hip external rotation isometrics, sidelying ER pulses with minimal ROM, and short-lever resisted ER in neutral. Rationale: These muscles act as local stabilizers, centering the femoral head and decreasing labral shear (Lewis & Sahrmann, 2006).
- Gluteus medius/minimus re-education: These muscles resist pelvic drop and control frontal plane motion. Drills: lateral band walks with a neutral pelvis, isometric wall abductions emphasizing trunk stacking. Rationale: Better pelvis-on-femur control reduces end-range compensation and impingement mechanics (Semciw et al., 2013).
- Adductor co-contraction: Balanced adductor activation with gluteals improves pelvic stability in turnout positions common in dance. Rationale: Adductors contribute to hip joint compression and stability when coordinated properly; imbalance leads to anterior shear.
- Core sequencing and breathing: Diaphragm-first breathing with lateral rib expansion, followed by gentle pelvic floor and deep abdominal engagement. Rationale: Appropriate intra-abdominal pressure and rib-pelvis alignment stabilize the lumbopelvic complex, reducing hip overuse.
Programming details:
- Early-phase isometrics minimize joint shear while enhancing proprioception.
- Progress to short-range controlled articular rotations (CARs) in pain-free arcs to improve capsulolabral nutrition and synovial flow without end-range irritation.
- Integrate perturbation training (elastic band pulls, multi-planar micro-perturbations) to build reflexive co-contraction.
Load Management: Protecting the Labrum While Building Resilience
We work closely with dancers and coaches to calibrate training loads:
- Volume and intensity caps post-PRP: Initially reduce deep flexion and turnout volume; avoid prolonged end-range splits and extreme external rotation while the joint environment normalizes.
- Temporal spacing of rehearsals: Micro-dosing technique works across the week rather than clustering high-intensity sessions. Rationale: Cartilage and labral tissue require time to recover; high-frequency end-range exposure elevates synovial irritation.
- Landing mechanics: Soft landings with a neutral pelvis and stacked rib cage; reduce knee valgus and excessive hip internal rotation during jumps. Rationale: Limits combined shear-compression forces on the anterosuperior labrum.
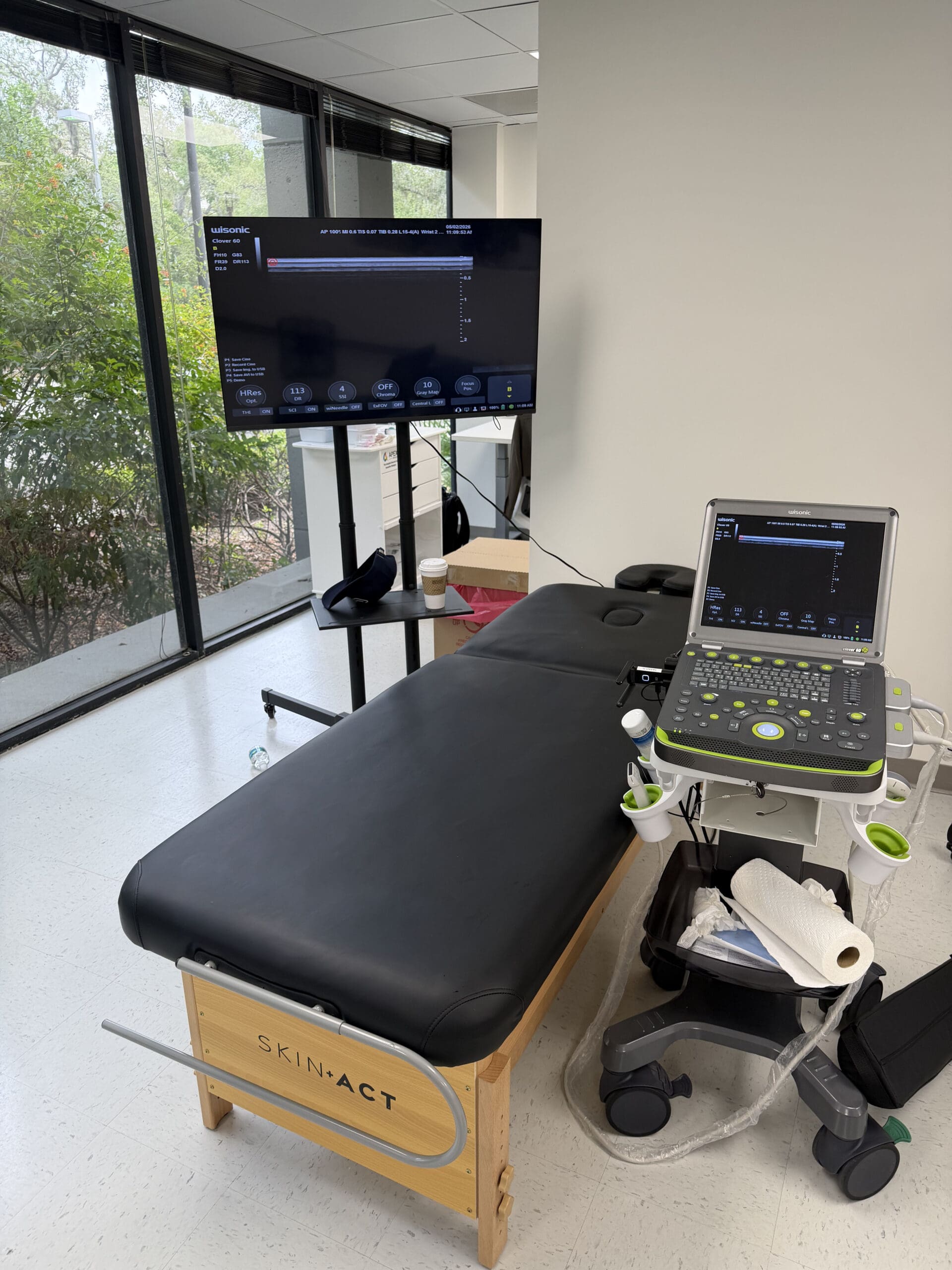
Ultrasound Guidance: Visualizing Safety and Accuracy
In the procedure, we identified the femoral artery medially to avoid vascular puncture, then positioned the ultrasound to obtain a crisp, perpendicular view of the femoral head and joint space. As the needle advanced, we maintained visualization to confirm intra-articular placement. If injection caused disproportionate pain and resistance, we reassessed needle location to avoid extra-articular soft-tissue expansion.
Why ultrasound:
- Real-time visualization improves accuracy of intra-articular delivery and reduces complications.
- Dynamic scanning lets us confirm landmarks and adjust needle angle to achieve the safest trajectory.
- For the hips, where depth and proximity to adjacent neurovascular structures increase risk, ultrasound offers a high-safety profile.
Rehabilitation Timeline: From PRP to Performance
While exact timelines vary, our structured approach commonly follows these phases:
Phase 1: Acute modulation (Weeks 0–2)
- Goals: Calm irritation, protect the labrum, initiate motor control.
- Actions: Relative rest from extremes; isometric deep rotator and gluteal activation; diaphragmatic breathing; gentle posterior chain mobility; low-load blood flow restriction (BFR) as appropriate to maintain conditioning while minimizing joint stress (Hughes et al., 2017).
- Rationale: Minimize synovial irritation post-PRP; build a foundation for stability.
Phase 2: Controlled mobility and strength (Weeks 2–6)
- Goals: Restore controlled ROM, increase strength without compromising stability.
- Actions: Short-range CARs, band-resisted ER/abduction, controlled hinge patterns, foot tripod training to improve lower-chain mechanics.
- Rationale: Gradual load promotes collagen remodeling and neuromuscular integration.
Phase 3: Dynamic control and return-to-technique (Weeks 6–12)
- Goals: Build tolerance to dance-specific positions.
- Actions: Turnout drills with strict pelvic control, landing pattern coaching, tempo progressions for leaps, proprioceptive perturbations.
- Rationale: Bridge clinic gains to stage performance, ensuring capacity before exposure to extremes.
Phase 4: Performance and resilience (Month 3+)
- Goals: Full return, prevention.
- Actions: Periodized training, recovery monitoring, ongoing stability conditioning, occasional technique tune-ups.
- Rationale: Maintain the labral seal and capsular integrity under real-world demands.
Integrative Chiropractic and Physical Therapy Synergy
Our emphasis at El Paso Back Clinic is the synergy of manual care and movement retraining:
- Chiropractic care targets alignment and segmental mobility that influence hip mechanics—especially in the lumbopelvic region. We emphasize precision adjustments when necessary, followed by stabilization drills to retain improved mechanics.
- Physical therapy builds durable control and strength in the hip girdle through progressive overload, task-specific cues, and feedback-rich training environments.
- Education ensures that athletes understand how habits such as deep lumbar extension and anterior pelvic tilt can compromise hip space. We coach sustainable alignment strategies for practice and performance.
Clinical Pearls from My Practice
- In hypermobile dancers, prioritize strength and control over flexibility. A more passive range is rarely the answer; better control of the existing range is.
- Pain during injection that is sharp and pressure-resistant often indicates extra-articular placement or capsular over-distension; reassess under ultrasound to confirm needle position.
- Persistent clicking without a discrete tear may indicate a labral suction seal disruption. Focus on deep rotator activation and pelvic control to restore functional sealing.
- Measuring progress: Use outcomes such as the Hip Outcome Score (HOS), return-to-technique benchmarks, and movement-quality metrics during controlled tasks.
When Surgery Is Considered—and Often Avoided
While hip arthroscopy for labral tears and FAI morphology can be beneficial in select cases, many dancers without large tears respond well to conservative care. If structural impingement is severe, surgical consultation may be warranted; however, careful rehab, load management, and biologic adjuncts like PRP can often provide significant relief and allow continued performance (Griffin et al., 2016).
Keeping Hormones and Medications in the Background
We maintain a primarily chiropractic and rehabilitation-centered approach. Hormonal factors, systemic inflammation, and medication considerations are reviewed as part of whole-person care, but they remain secondary to hands-on, movement-based strategies that directly influence hip stability and mechanics for dancers.
Putting It All Together: A Practical Plan for Dancers
- Assess thoroughly with imaging and functional testing to differentiate between irritation and tear and to identify instability patterns.
- Use ultrasound-guided PRP judiciously to modulate symptoms and support tissue healing in selected cases.
- Apply manual therapy to normalize tone and mechanics—avoid overstretching lax joints.
- Drive neuromuscular control of deep rotators, gluteals, and core with progressive, feedback-rich drills.
- Implement load management and technique coaching to prevent end-range overuse.
- Track objective outcomes and adjust the plan in response to functional and performance demands.
Conclusion: Durable Stability for High-Performance Hips
For dancers, the pathway back to pain-free, confident movement runs through stability, control, and smart loading. Biologic adjuncts like PRP, delivered safely under ultrasound guidance, can help create the conditions for successful rehabilitation. The heart of the solution, however, lies in integrative chiropractic care and physical therapy—precise manual techniques paired with targeted neuromuscular retraining, all tuned to the demands of dance. With this approach, many dancers move beyond pain and clicking to sustained performance, preserving the labral seal and protecting the capsule over the long term.
References
- Hip Labrum Function, Pathology, and Clinical Implications (Nepple, J., et al., 2015). Journal of Orthopaedic & Sports Physical Therapy.
- Capsular Laxity and Hip Microinstability: Clinical Considerations (Domb, B., et al., 2013). The American Journal of Sports Medicine.
- Movement System Impairments and Hip Control (Lewis, C., & Sahrmann, S., 2006). The American Journal of Sports Medicine.
- PRP Mechanisms and Clinical Applications in Musculoskeletal Medicine (Mautner, K., et al., 2015). Sports Health.
- PRP for Chronic Tendinopathy and Joint Conditions: Systematic Review (Fitzpatrick, J., et al., 2017). British Journal of Sports Medicine.
- PRP in Hip Osteoarthritis and Intra-articular Pathology: Evidence Overview (Smith, J., 2016). Sports Health.
- Blood Flow Restriction Training: Mechanisms and Applications (Hughes, L., et al., 2017). British Journal of Sports Medicine.
- FAI Management: From Conservative Care to Arthroscopy (Griffin, D., et al., 2016). British Journal of Sports Medicine.
- Gluteal Muscle Function and Hip Stability (Semciw, A., et al., 2013). Physical Therapy in Sport.
- Joint Mobilization Concepts for the Hip (Kaltenborn, F., 2003). Archives of Physical Medicine and Rehabilitation.
General Disclaimer, Licenses and Board Certifications *
Professional Scope of Practice *
The information herein on "Chiropractic PRP Care for Hip Impingement Insights" is not intended to replace a one-on-one relationship with a qualified health care professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional.
Blog Information & Scope Discussions
Welcome to El Paso's Premier Wellness and Injury Care Clinic & Wellness Blog, where Dr. Alex Jimenez, DC, FNP-C, a Multi-State board-certified Family Practice Nurse Practitioner (FNP-BC) and Chiropractor (DC), presents insights on how our multidisciplinary team is dedicated to holistic healing and personalized care. Our practice aligns with evidence-based treatment protocols inspired by integrative medicine principles, similar to those on this site and on our family practice-based chiromed.com site, focusing on naturally restoring health for patients of all ages.
Our areas of multidisciplinary practice include Wellness & Nutrition, Chronic Pain, Personal Injury, Auto Accident Care, Work Injuries, Back Injury, Low Back Pain, Neck Pain, Migraine Headaches, Sports Injuries, Severe Sciatica, Scoliosis, Complex Herniated Discs, Fibromyalgia, Complex Injuries, Stress Management, Functional Medicine Treatments, and in-scope care protocols.
Our information scope is multidisciplinary, focusing on musculoskeletal and physical medicine, wellness, contributing etiological viscerosomatic disturbances within clinical presentations, associated somato-visceral reflex clinical dynamics, subluxation complexes, sensitive health issues, and functional medicine articles, topics, and discussions.
We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for musculoskeletal injuries or disorders.
Our videos, posts, topics, and insights address clinical matters and issues that are directly or indirectly related to our clinical scope of practice.
Our office has made a reasonable effort to provide supportive citations and has identified relevant research studies that support our posts. We provide copies of supporting research studies upon request to regulatory boards and the public.
We understand that we cover matters that require an additional explanation of how they may assist in a particular care plan or treatment protocol; therefore, to discuss the subject matter above further, please feel free to ask Dr. Alex Jimenez, DC, APRN, FNP-BC, or contact us at 915-850-0900.
We are here to help you and your family.
Blessings
Dr. Alex Jimenez, DC, MSACP, APRN, FNP-BC*, CCST, IFMCP, CFMP, ATN
email: [email protected]
Multidisciplinary Licensing & Board Certifications:
Licensed as a Doctor of Chiropractic (DC) in Texas & New Mexico*
Texas DC License #: TX5807, Verified: TX5807
New Mexico DC License #: NM-DC2182, Verified: NM-DC2182
Multi-State Advanced Practice Registered Nurse (APRN*) in Texas & Multi-States
Multi-state Compact APRN License by Endorsement (42 States)
Texas APRN License #: 1191402, Verified: 1191402 *
Florida APRN License #: 11043890, Verified: APRN11043890 *
Colorado License #: C-APN.0105610-C-NP, Verified: C-APN.0105610-C-NP
New York License #: N25929, Verified N25929
License Verification Link: Nursys License Verifier
* Prescriptive Authority Authorized
ANCC FNP-BC: Board Certified Nurse Practitioner*
Compact Status: Multi-State License: Authorized to Practice in 40 States*
Graduate with Honors: ICHS: MSN-FNP (Family Nurse Practitioner Program)
Degree Granted. Master's in Family Practice MSN Diploma (Cum Laude)
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
My Digital Business Card
Licenses and Board Certifications:
DC: Doctor of Chiropractic
APRNP: Advanced Practice Registered Nurse
FNP-BC: Family Practice Specialization (Multi-State Board Certified)
RN: Registered Nurse (Multi-State Compact License)
CFMP: Certified Functional Medicine Provider
MSN-FNP: Master of Science in Family Practice Medicine
MSACP: Master of Science in Advanced Clinical Practice
IFMCP: Institute of Functional Medicine
CCST: Certified Chiropractic Spinal Trauma
ATN: Advanced Translational Neutrogenomics
Memberships & Associations:
TCA: Texas Chiropractic Association: Member ID: 104311
AANP: American Association of Nurse Practitioners: Member ID: 2198960
ANA: American Nurse Association: Member ID: 06458222 (District TX01)
TNA: Texas Nurse Association: Member ID: 06458222
NPI: 1205907805
| Primary Taxonomy | Selected Taxonomy | State | License Number |
|---|---|---|---|
| No | 111N00000X - Chiropractor | NM | DC2182 |
| Yes | 111N00000X - Chiropractor | TX | DC5807 |
| Yes | 363LF0000X - Nurse Practitioner - Family | TX | 1191402 |
| Yes | 363LF0000X - Nurse Practitioner - Family | FL | 11043890 |
| Yes | 363LF0000X - Nurse Practitioner - Family | CO | C-APN.0105610-C-NP |
| Yes | 363LF0000X - Nurse Practitioner - Family | NY | N25929 |
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
My Digital Business Card