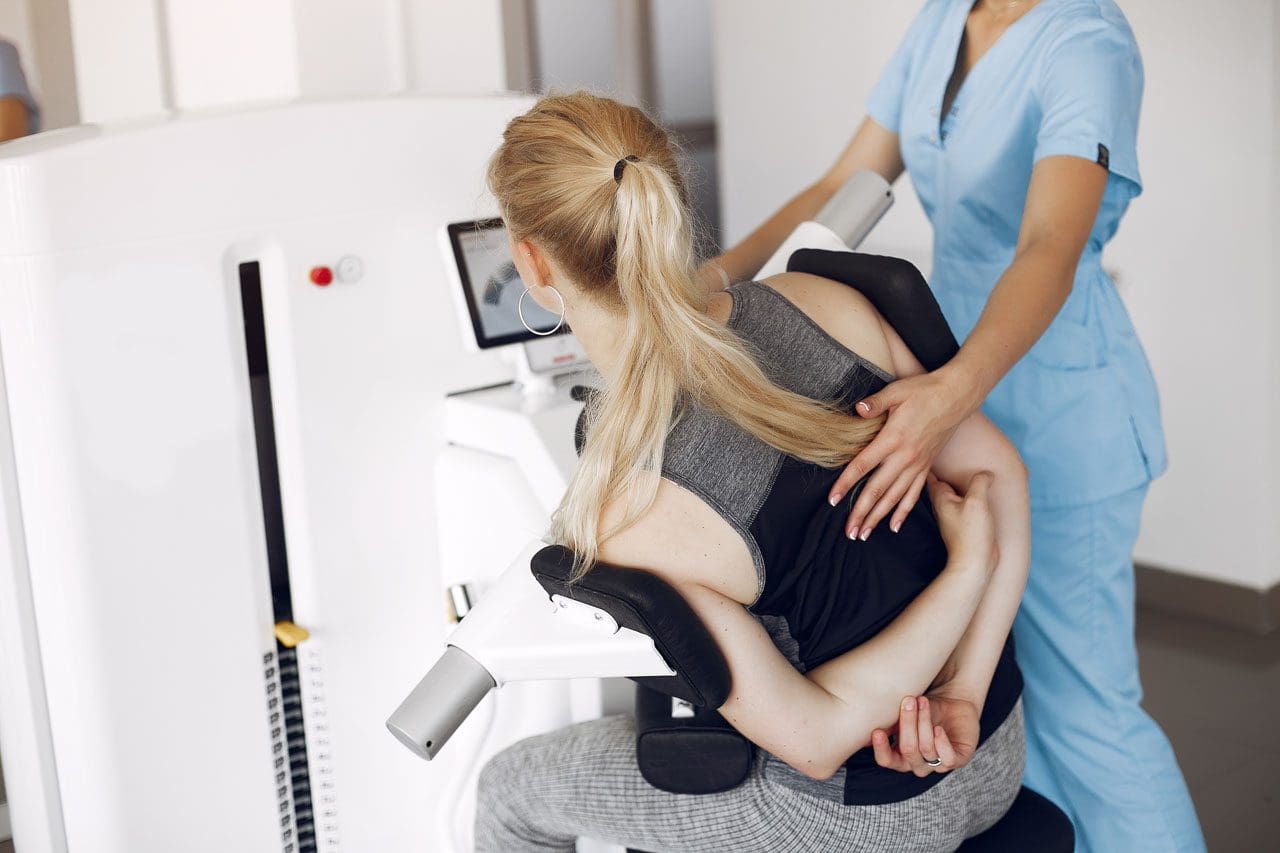
A Clinical Approach To Reproductive Health & Sexual Wellness for All Ages
Explore the clinical approach to reproductive health, focusing on evidence-based practices to enhance well-being.
Reproductive Health
In terms of reproductive health, many women may see physical changes when their menstrual cycles increase or decrease, which might have an impact on their bodies. Menstrual changes may continue anywhere from one to three years, but each woman’s menopausal symptoms will be unique.
The following are a few signs of hormonal alterations related to reproductive health:
- Sleeplessness
- Variations in weight
- Weariness Muscle and joint pain
At the same time, a woman’s body is exhibiting pain-like sensations as a result of hormonal changes related to her reproductive health. The body, hormones, and spinal structure all change with age. Low back pain may result from overlapping risk profiles for the musculoskeletal system and reproductive health caused by a variety of environmental variables that impact the body. Numerous variables, such as different menstrual cycles and greater pain sensitivity, are blamed for the low back discomfort that many people, particularly women, experience. (Chen and others, 2024)
Hormone Replacement Therapy
Hormone replacement Therapy or HRT is a treatment that can be used to treat some of the symptoms of hormonal changes associated with reproductive health by replacing hormones that are at a lower level. For females, low estrogen and progesterone levels can affect neuroprotective receptors in the brain, causing symptoms of inflammation and stress to impact the body. (Hwang et al., 2020) For males, low testosterone levels can cause skeletal muscle mass and strength reduction, decreased bone mineral density, and sexual dysfunction. (Barone et al., 2022) So, for males and females, taking HRT can help replenish the lost hormones in their bodies and reduce the overlapping pain symptoms.
Andropause & Menopause
When a woman between the ages of mid-40s and mid-50s deals with changes in their menstrual cycle, it is known as menopause. When a woman goes through menopause, it is a transition period where the woman’s ovaries stop releasing eggs, and their hormone levels of estrogen and progesterone decrease, thus ceasing a woman’s menstruation cycle. Within that time frame during menopause, most women will experience weight gain and have an increase of peripheral fat stored in the hips, glutes, and around the abdominals. (Ko & Kim, 2020) This extra weight around the abdominals and hips can lead to the development of musculoskeletal issues like back pain.
While males have the capability of reproduction throughout their lives after puberty, when they begin to age, they produce low testosterone levels and fewer sperm. Additionally, a majority of men can experience low levels of testosterone hormones as they start to notice a decreased libido, body hair loss, loss of muscle mass, and breast enlargement. This is known as andropause, where, like menopause in women, the testosterone hormone levels are lowered. Luckily, low testosterone levels can be tested, allowing males to be treated with testosterone replacement therapy. Testosterone replacement therapy can provide beneficial results by replenishing testosterone levels associated with reducing symptoms of decreased libido, improving skeletal muscle function, and restoring bone mineral density. (Barbonetti et al., 2020)
Testosterone Deficiency In Men- Video
Surgical & Non-Surgical Interventions
Many middle-aged adults would discuss with their partners about not wanting to have children or are finished having children. When it comes to interventions such as this, many choose surgical or non-surgical procedures. Females can have a surgical procedure known as tubal ligation. This procedure has the fallopian tubes either cut, tied, or removed to prevent pregnancy while still having their menstrual cycle until menopause, so there is no impact on the hormones. For males, they can go through a surgical procedure known as a vasectomy so that the vas deferens are cut and sealed. Both methods are 99% effective in preventing pregnancy. These outpatient procedures have different state laws and safeguards regarding sterilization surgery.
However, not many people will go on the surgical route to prevent surgery and will go on the non-surgical route. Many people will utilize birth control methods like birth control medication, condoms, and natural cycle planning. For women, many will incorporate hormonal birth control medication as part of their routine in preventing pregnancy. Some of the added benefits for women who are taking contraceptives include: (Allen et al., 2013)
- Restoring menstrual regularity
- Improving vasomotor symptoms
- Preventing bone mineral density decline
Sex Changes In Middle Adulthood
Many people are sexually active via communication and strong connections with their partners, making them an integral part of people’s life at any age. Intimacy allows many healthy couples to express their needs and desires more easily. Adults also experience sexual changes associated with their reproductive health as they age. Many women have pelvic discomfort as a result of decreased lubrication brought on by the vagina’s normal constriction, shortening, and thinning of its walls.
As men age, their erection functionality also changes, particularly if they have health and wellness-related comorbidities. The inability to get an erection, often known as erectile dysfunction or ED, is one of the most prevalent changes in older guys. (Sooriyamoorthy & Leslie, 2025) When risk profiles from environmental variables intersect, ED may develop as a symptom. Fortunately, ED may be treated by altering one’s lifestyle and taking care of interpersonal or psychological problems. (Lowy & Ramanathan, 2022) Men may find it challenging to talk to their physicians about it, but it is crucial for their health and welfare.
Final Thoughts
In general, many people who suffer from pain and musculoskeletal problems might benefit from a personalized treatment plan for their sexual and reproductive health. In the long run, small changes to a routine can pay off, and gradually introducing a new routine—such as eating more vegetables and lean meats, exercising for half an hour, or getting a wellness checkup—can help manage pain-like symptoms brought on by environmental factors and support an individual’s health journey.
Injury Medical & Functional Medicine Clinic
We associate with certified medical providers who understand the importance of assessing individuals dealing with reproductive and sexual health associated with body pain. When asking important questions to our associated medical providers, we advise patients to implement various approaches to their reproductive and sexual health associated with their pain. Dr. Alex Jimenez, D.C., utilizes this information as an academic service. Disclaimer.
References
Allen, R. H., Cwiak, C. A., & Kaunitz, A. M. (2013). Contraception in women over 40 years of age. CMAJ, 185(7), 565-573. https://doi.org/10.1503/cmaj.121280
Barbonetti, A., D’Andrea, S., & Francavilla, S. (2020). Testosterone replacement therapy. Andrology, 8(6), 1551-1566. https://doi.org/10.1111/andr.12774
Barone, B., Napolitano, L., Abate, M., Cirillo, L., Reccia, P., Passaro, F., Turco, C., Morra, S., Mastrangelo, F., Scarpato, A., Amicuzi, U., Morgera, V., Romano, L., Calace, F. P., Pandolfo, S. D., De Luca, L., Aveta, A., Sicignano, E., Trivellato, M.,…Crocetto, F. (2022). The Role of Testosterone in the Elderly: What Do We Know? Int J Mol Sci, 23(7). https://doi.org/10.3390/ijms23073535
Chen, D., Zhou, J., Lin, C., Li, J., Zhu, Z., Rao, X., Wang, J., Li, J., Chen, H., Wang, F., Li, X., Gao, M., Zhou, Z., Xi, Y., & Li, S. (2024). A causal examination of the correlation between hormonal and reproductive factors and low back pain. Front Endocrinol (Lausanne), 15, 1326761. https://doi.org/10.3389/fendo.2024.1326761
Hwang, W. J., Lee, T. Y., Kim, N. S., & Kwon, J. S. (2020). The Role of Estrogen Receptors and Their Signaling across Psychiatric Disorders. Int J Mol Sci, 22(1). https://doi.org/10.3390/ijms22010373
Ko, S. H., & Kim, H. S. (2020). Menopause-Associated Lipid Metabolic Disorders and Foods Beneficial for Postmenopausal Women. Nutrients, 12(1). https://doi.org/10.3390/nu12010202
Leslie, S. W., & Sooriyamoorthy, T. (2025). Erectile Dysfunction. In StatPearls. https://www.ncbi.nlm.nih.gov/pubmed/32965924
Lowy, M., & Ramanathan, V. (2022). Erectile dysfunction: causes, assessment and management options. Aust Prescr, 45(5), 159-161. https://doi.org/10.18773/austprescr.2022.051