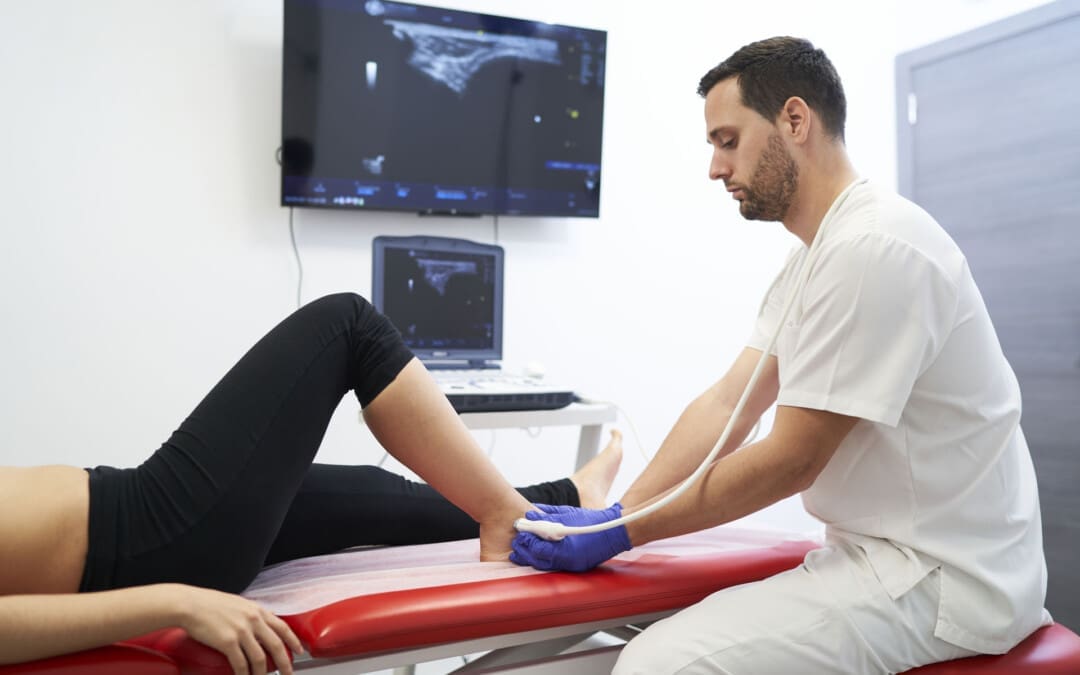
Are individuals with high foot arches or participating in sports involving repetitive ankle motion at risk for developing peroneal tendon injuries?
Contents
Peroneal Tendon Injuries
The peroneal tendons connect the muscles of the outer side of the lower leg to the foot. They may be acute—occurring suddenly—or chronic—developing over time. The basic types of peroneal tendon injuries are tendonitis, tears, and subluxation.
Anatomy and Function
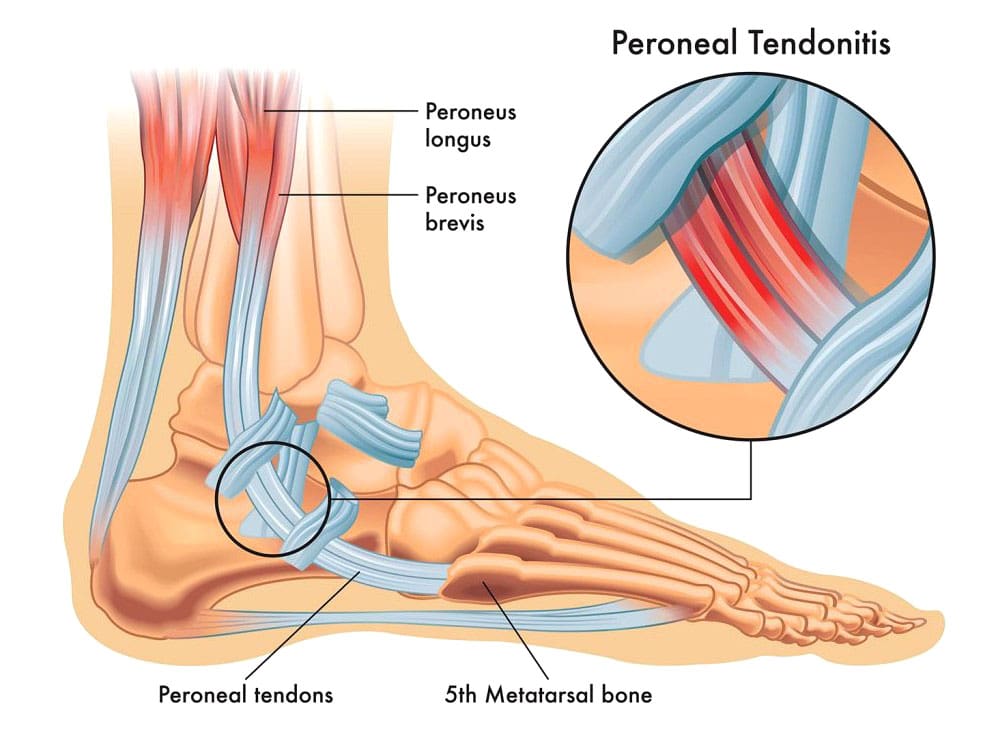
The two major peroneal muscles (peroneus longus and peroneus brevis) are outside the lower leg, next to the calf muscles. The peroneal tendons run along the outer side of the ankle and attach to the foot, connecting these muscles to bone. They help stabilize the ankle joint, point the foot downward (plantarflexion), and turn the foot outward (eversion). In normal gait, the motion of the peroneal muscles is balanced by the muscles that invert the foot or rock the foot inward from the ankle. The two peroneal tendons sit one on top of the other right behind the fibula (the smaller lower leg bone). This closeness can contribute to problems with the peroneal tendons, as they rub together behind the ankle.
Tendonitis
The most common problem is inflammation or tendonitis. The tendons are usually inflamed just behind the fibula bone at the ankle joint. This part of the fibula is the bump on the outside of the ankle, and the peroneal tendons are located just behind that bony prominence. Tendonitis can either result from repetitive overuse or an acute injury. Common symptoms of tendonitis include:
- Pain behind the ankle
- Swelling over the peroneal tendons
- Tenderness of the tendons
- Pain usually worsens if the foot is pulled down and inwards, stretching the peroneal tendons.
- X-rays of the ankle are taken.
- MRI may show inflammation and fluid around the tendons. (Walt J. & Massey P. 2023)
Typical treatment of peroneal tendonitis is accomplished by:
Ice application
- Applying ice to the area can help reduce swelling and control pain.
Rest
- Resting is important to allow the tendon to heal.
- A supportive device (walking boot or ankle brace) or crutches can help in severe cases.
- Braces and boots provide support, reduce tendons’ stress, and allow rest and inflammation to subside.
Anti-inflammatory Medications
- Motrin or Aleve are anti-inflammatory and can reduce the swelling around the tendon.
Physical Therapy
- Physical therapy can help restore normal ankle joint mechanics, help with swelling and pain relief, and correct strength imbalances.
Cortisone Injections
- Cortisone injections are low-risk if administered to the area around the tendon and not more often than every three months.
- Ultrasound guidance can help ensure the medication is injected into the correct area. (Walt J. & Massey P. 2023)
Tendon Tears
Tears can occur and are more likely to happen in the peroneus brevis tendon. Tears are believed to be the result of two issues with the tendon. One is the blood supply. Tears of the peroneus brevis tendon almost always occur in the area where the blood supply and nutrition of the tendon are the poorest.
The second issue is the closeness between the two tendons, causing the peroneus brevis tendon to be wedged between the peroneus longus tendon and the bone. (Saxena A., & Bareither D. 2001) Tears of the peroneus brevis tendon are often treated with the same treatments for tendonitis. About half of the tears diagnosed by imaging are found to be asymptomatic. For individuals who don’t find lasting relief from symptoms, surgery may be necessary. Surgical options for peroneal tendon tears (Dombek M. F. et al., 2001)
Tendon Debridement and Repair
- During a tendon debridement, the damaged tendon and the surrounding inflammatory tissue are removed.
- The tear can be repaired, and the tendon can be tubularized to restore its normal shape.
Tenodesis
- A tenodesis is a procedure where the damaged area of the tendon is sewn to the normal tendon.
- In this case, the damaged segment of the peroneal tendon is removed, and the ends left behind are sewn to the adjacent remaining peroneal tendon.
- Tenodesis is often recommended for tears involving more than 50% of the tendon. (Castilho R. S. et al., 2024)
Depending on the surgical procedure, Recovery after surgery can take several weeks of restricted weight-bearing and immobilization. Following immobilization, therapy can begin. Recovery is usually six to 12 weeks, depending on the surgery, but a full return to sports and activities may take several months. Risks of surgery include infection, stiffness, skin numbness near the incision, persistent swelling, and persistent pain.
Injury Medical Chiropractic and Functional Medicine Clinic
Injury Medical Chiropractic and Functional Medicine Clinic works with primary healthcare providers and specialists to build optimal health and wellness solutions. We focus on what works for you to relieve pain, restore function, prevent injury, and help mitigate issues through adjustments that help the body realign itself. They can also work with other medical professionals to integrate a treatment plan to resolve musculoskeletal problems.
The Difference of Using Custom Foot Orthotics
References
Walt, J., & Massey, P. (2025). Peroneal Tendon Syndromes. In StatPearls. https://www.ncbi.nlm.nih.gov/pubmed/31335074
Saxena, A., & Bareither, D. (2001). Magnetic resonance and cadaveric findings of the “watershed band” of the Achilles tendon. The Journal of foot and ankle surgery: official publication of the American College of Foot and Ankle Surgeons, 40(3), 132–136. https://doi.org/10.1016/s1067-2516(01)80078-8
Dombek, M. F., Orsini, R., Mendicino, R. W., & Saltrick, K. (2001). Peroneus brevis tendon tears. Clinics in podiatric medicine and surgery, 18(3), 409–427.
Castilho, R. S., Magalhães, J. M. B., Veríssimo, B. P. M., Perisano, C., Greco, T., & Zambelli, R. (2024). Minimally Invasive Peroneal Tenodesis Assisted by Peroneal Tendoscopy: Technique and Preliminary Results. Medicina (Kaunas, Lithuania), 60(1), 104. https://doi.org/10.3390/medicina60010104
General Disclaimer, Licenses and Board Certifications *
Professional Scope of Practice *
The information herein on "Peroneal Tendon Damage: Causes and Treatment" is not intended to replace a one-on-one relationship with a qualified health care professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional.
Blog Information & Scope Discussions
Welcome to El Paso's Premier Wellness and Injury Care Clinic & Wellness Blog, where Dr. Alex Jimenez, DC, FNP-C, a Multi-State board-certified Family Practice Nurse Practitioner (FNP-BC) and Chiropractor (DC), presents insights on how our multidisciplinary team is dedicated to holistic healing and personalized care. Our practice aligns with evidence-based treatment protocols inspired by integrative medicine principles, similar to those on this site and on our family practice-based chiromed.com site, focusing on naturally restoring health for patients of all ages.
Our areas of multidisciplinary practice include Wellness & Nutrition, Chronic Pain, Personal Injury, Auto Accident Care, Work Injuries, Back Injury, Low Back Pain, Neck Pain, Migraine Headaches, Sports Injuries, Severe Sciatica, Scoliosis, Complex Herniated Discs, Fibromyalgia, Complex Injuries, Stress Management, Functional Medicine Treatments, and in-scope care protocols.
Our information scope is multidisciplinary, focusing on musculoskeletal and physical medicine, wellness, contributing etiological viscerosomatic disturbances within clinical presentations, associated somato-visceral reflex clinical dynamics, subluxation complexes, sensitive health issues, and functional medicine articles, topics, and discussions.
We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for musculoskeletal injuries or disorders.
Our videos, posts, topics, and insights address clinical matters and issues that are directly or indirectly related to our clinical scope of practice.
Our office has made a reasonable effort to provide supportive citations and has identified relevant research studies that support our posts. We provide copies of supporting research studies upon request to regulatory boards and the public.
We understand that we cover matters that require an additional explanation of how they may assist in a particular care plan or treatment protocol; therefore, to discuss the subject matter above further, please feel free to ask Dr. Alex Jimenez, DC, APRN, FNP-BC, or contact us at 915-850-0900.
We are here to help you and your family.
Blessings
Dr. Alex Jimenez, DC, MSACP, APRN, FNP-BC*, CCST, IFMCP, CFMP, ATN
email: [email protected]
Multidisciplinary Licensing & Board Certifications:
Licensed as a Doctor of Chiropractic (DC) in Texas & New Mexico*
Texas DC License #: TX5807, Verified: TX5807
New Mexico DC License #: NM-DC2182, Verified: NM-DC2182
Multi-State Advanced Practice Registered Nurse (APRN*) in Texas & Multi-States
Multi-state Compact APRN License by Endorsement (42 States)
Texas APRN License #: 1191402, Verified: 1191402 *
Florida APRN License #: 11043890, Verified: APRN11043890 *
Colorado License #: C-APN.0105610-C-NP, Verified: C-APN.0105610-C-NP
New York License #: N25929, Verified N25929
License Verification Link: Nursys License Verifier
* Prescriptive Authority Authorized
ANCC FNP-BC: Board Certified Nurse Practitioner*
Compact Status: Multi-State License: Authorized to Practice in 40 States*
Graduate with Honors: ICHS: MSN-FNP (Family Nurse Practitioner Program)
Degree Granted. Master's in Family Practice MSN Diploma (Cum Laude)
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
My Digital Business Card
Licenses and Board Certifications:
DC: Doctor of Chiropractic
APRNP: Advanced Practice Registered Nurse
FNP-BC: Family Practice Specialization (Multi-State Board Certified)
RN: Registered Nurse (Multi-State Compact License)
CFMP: Certified Functional Medicine Provider
MSN-FNP: Master of Science in Family Practice Medicine
MSACP: Master of Science in Advanced Clinical Practice
IFMCP: Institute of Functional Medicine
CCST: Certified Chiropractic Spinal Trauma
ATN: Advanced Translational Neutrogenomics
Memberships & Associations:
TCA: Texas Chiropractic Association: Member ID: 104311
AANP: American Association of Nurse Practitioners: Member ID: 2198960
ANA: American Nurse Association: Member ID: 06458222 (District TX01)
TNA: Texas Nurse Association: Member ID: 06458222
NPI: 1205907805
| Primary Taxonomy | Selected Taxonomy | State | License Number |
|---|---|---|---|
| No | 111N00000X - Chiropractor | NM | DC2182 |
| Yes | 111N00000X - Chiropractor | TX | DC5807 |
| Yes | 363LF0000X - Nurse Practitioner - Family | TX | 1191402 |
| Yes | 363LF0000X - Nurse Practitioner - Family | FL | 11043890 |
| Yes | 363LF0000X - Nurse Practitioner - Family | CO | C-APN.0105610-C-NP |
| Yes | 363LF0000X - Nurse Practitioner - Family | NY | N25929 |
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
My Digital Business Card