Tibial Plateau Fractures
- Impaction type fractures predominate
- Result from valgus or varus stress with or w/o axial loading
- Associated with periarticular soft tissues injury
- High-stress injury m/c due to jumps falls and axial loading, often with the splitting of the tibial plateau. Men>women. Patients are in their 30s
- Low impact or no trauma in patients with osteoporosis d/t insufficiency fractures
- Impaction injury is more common with depression of tibial plateau. Women>men. Patients are in their 70s
Contents
Lateral Tibial Plateau Fractures More Common
- Functional anatomy plays a significant role
- 60% of weight bearing is by the medial plateau
- The medial plateau is more concave
- Lateral plateau is slightly higher and more convex. Valgus stress impacts lateral plateau.
- Tibial plateau fractures considered intra-articular and prone to delayed healing, non-union, meniscal injury (m/c lateral) ACL tear, secondary OA. Other complications: compartment syndrome, vascular injury.
- Management: operative in many cases especially if >3-mm step-off at the plateau
- If medial plateau or bicondylar Fxs present, ORIF will be required.
Imaging Plays A Crucial Role
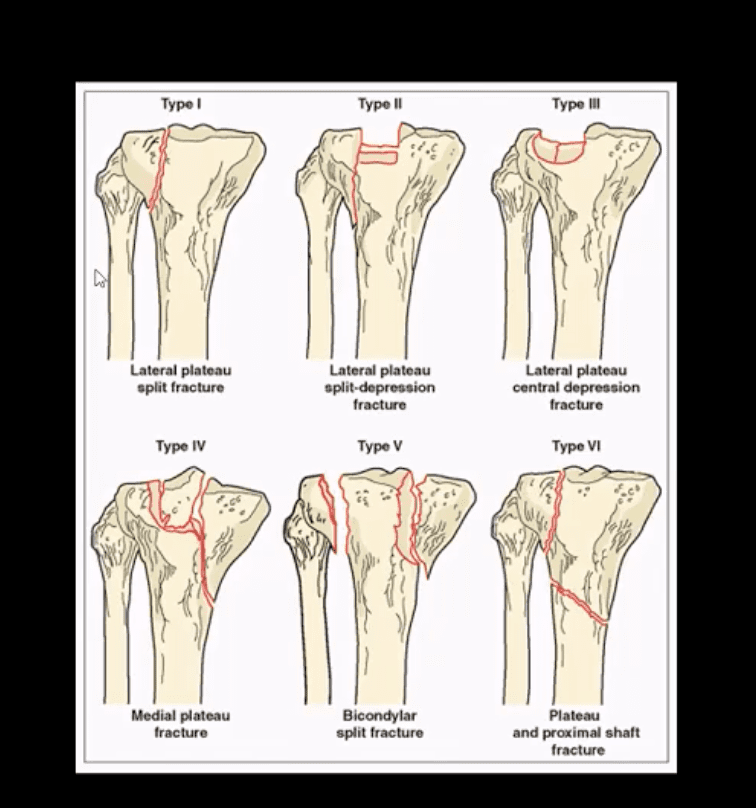
- Begins with x-radiography. X-radiography may not reveal the complexity and extent of this injury.
- CT scanning w/o contrast will further delineate fracture complexity and pre-operative planning
- MR imaging may be considered to evaluate for internal derangement: meniscal, ACL injuries.
- Shatzke classification may help to evaluate the complexity of this injury
Key Diagnostic Sign
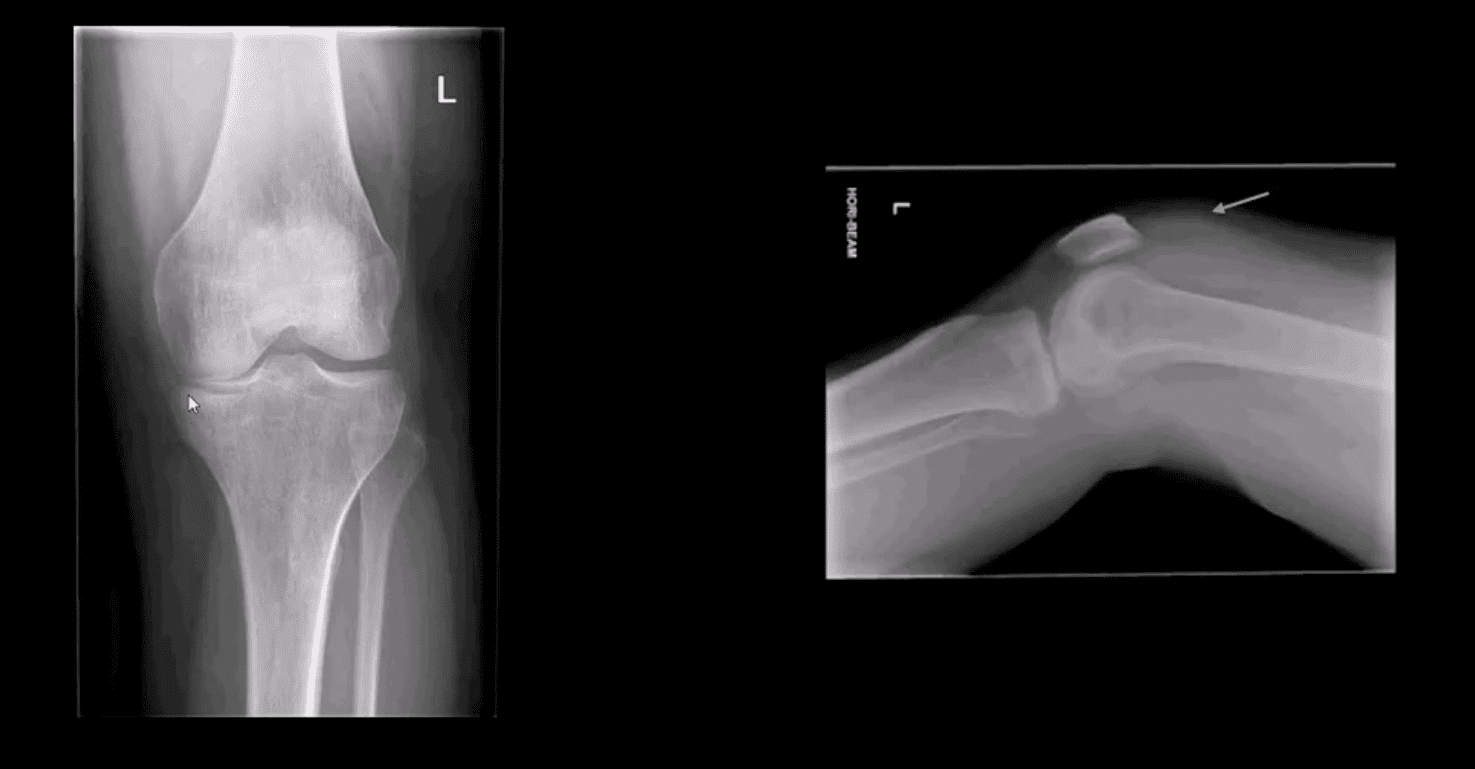
- AP and lateral horizontal beam (cross table) left knee radiograph. Note subtle depression of the lateral plateau manifested by the lateral plateau appearing at the same level or lower as the medial. A critical diagnostic sign is the presence of fat-blood-interphase or FBI sign on cross-table lateral (above arrow) indicating intra-articular knee fracture
Lipohemarthorosis aka FBI Sign
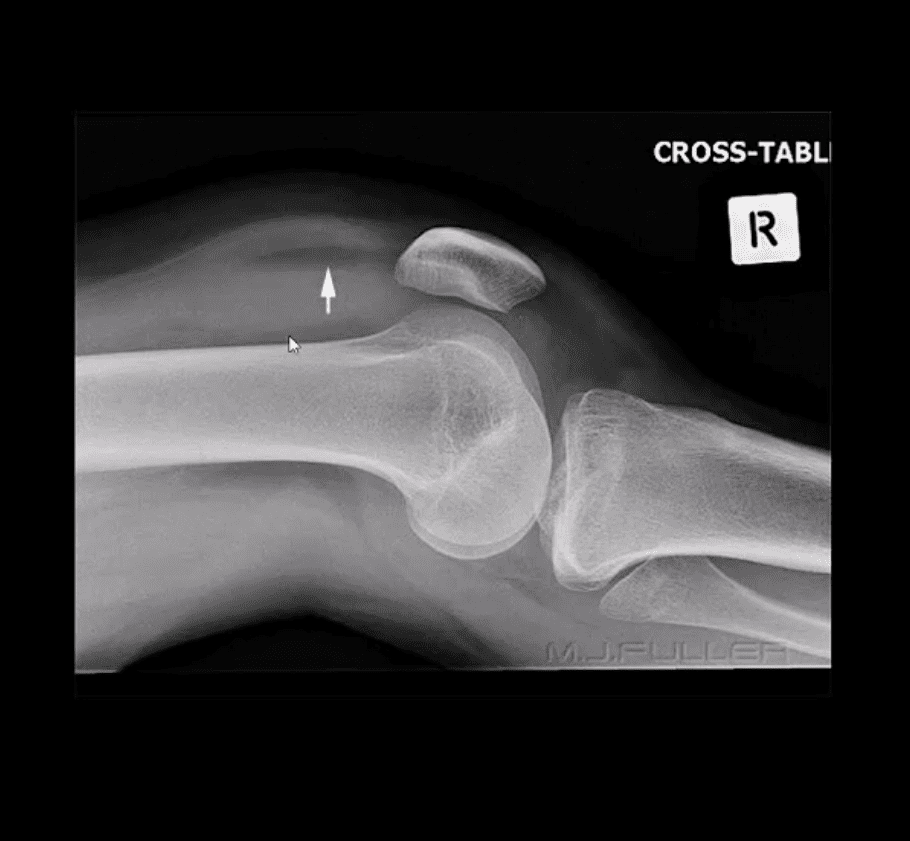
- Can be detected by radiography, CT or MR imaging
- FBI sign is a reliable secondary radiographic sign of intra-articular knee fractures, regardless of how small they are
- Mechanism: fracture results with acute hemarthrosis
- Hemarthrosis will also occur w/o Fx. However, Fx will result with a fatty marrow being released into the joint cavity. Fat is a less dense medium (lighter) and will appear on the top of the hemorrhage if the patient is held in the supine position for 5-10-minutes before the cross-table radiograph is taken
- FBI sign confirms the intra-articular Fx.
- ACL/PCL, meniscal tears will not result in FBI sign
Lateral Tibial Plateau Fx
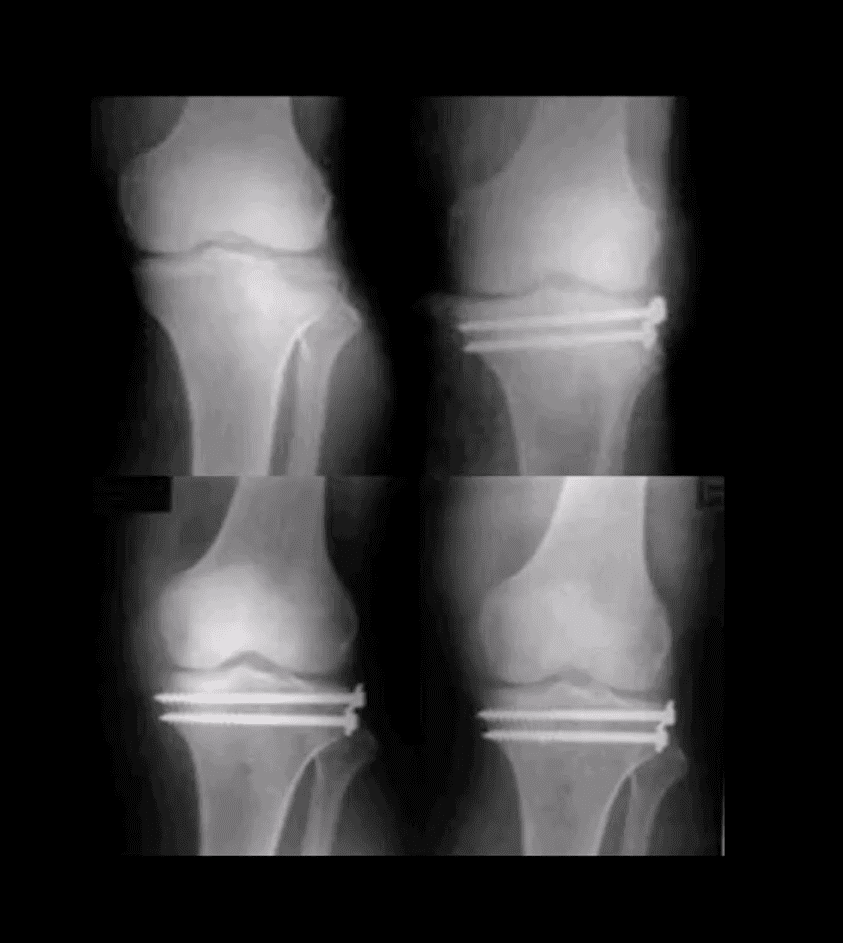
- Lateral tibial plateau Fx that was managed operatively
- Most common complication: premature secondary OA
- More complex injuries may result in more extensive operative care
Knee Internal Derangement
- Acute or chronic injuries of meniscal fibrocartilages and ligamentous restraints
- Tears of the ACL and posterior horn of the medial meniscus are the most common
- Acute ACL tears, however, often result with a lateral meniscus tear
- Acute ACL tear may occur as a combined injury of the ACL, MCL, and medial meniscus
- Functional anatomy: ACL prevents anterior displacement of the tibia and secondary varus stress
- MCL functions together with ACL in resisting external rotation of the tibia especially when the foot is planted (closed chain position)
- MCL is firmly attached to the medial meniscus, explaining the classic triad of ACL, MCL and medial meniscal tear (O’Donahue terrible triad)
- Cruciate ligaments (ACL/PCL) are intra-articular but extra-synovial. Less likely to be torn in closed pack position (full extension). When all articular facets of tibia and femur are in full contact, the ACL/PCL are at least tension and stable
- When the knee is flexed 20-30-degrees or more ACL is taut and remains unstable
- ACL is a significant mechanoreceptor that feeds the info to CNS about the joint position. Thus the majority of previous ACL tears will lead to some degree of knee instability
Functional Anatomy of ACL
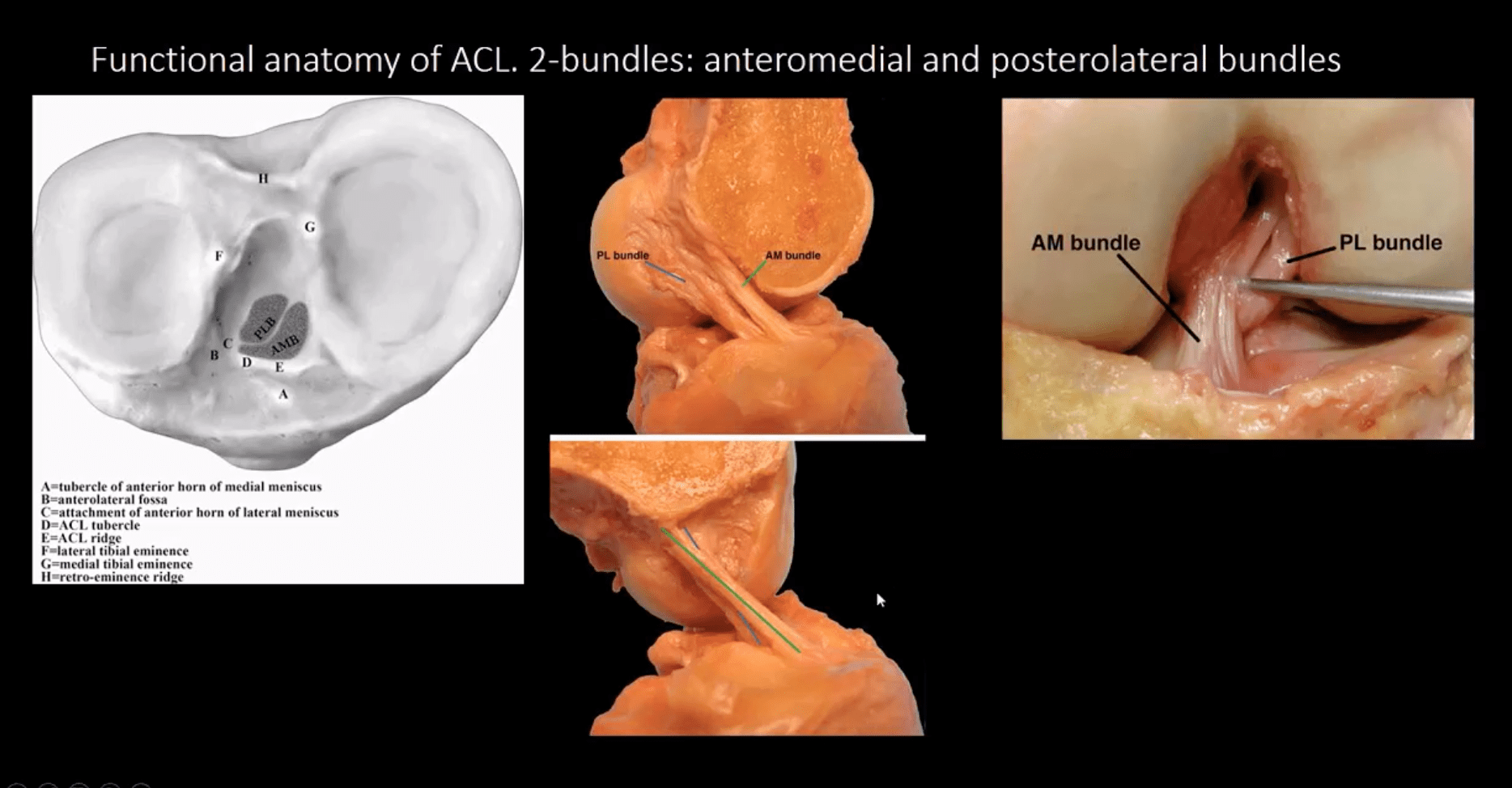
Diagnosis of ACL Tear
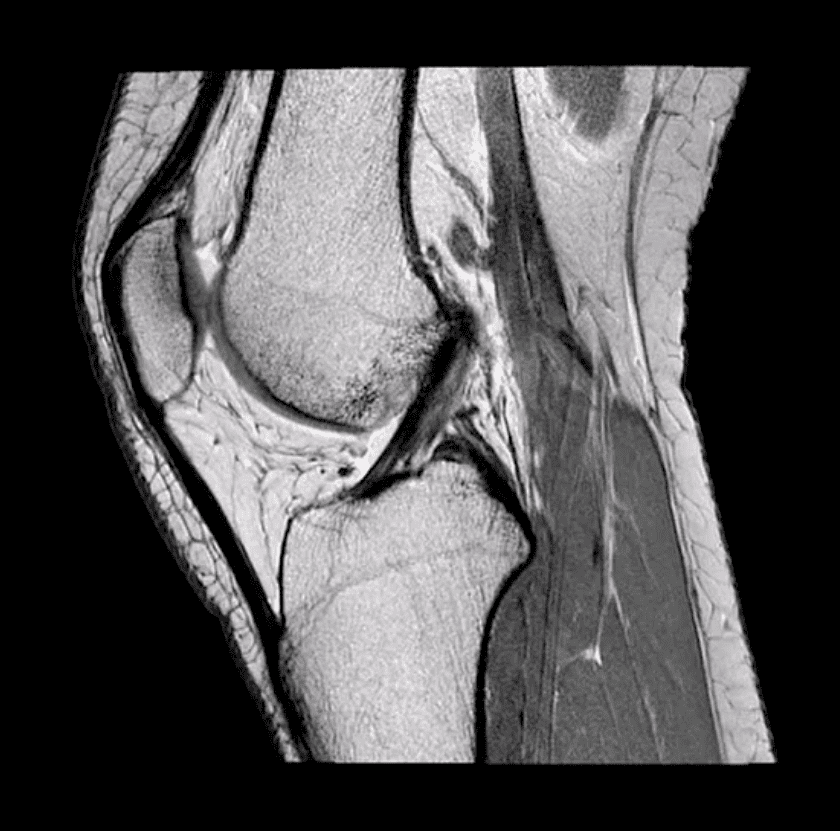
- Diagnosis of ACL tear requires MR imaging
- Concerns exist of not only ligamentous injuries but injuries to the articular cartilage and menisci.
- Most vendors will perform at least: one T1 WI in coronal or sagittal planes. Sagittal and coronal Proton-density slices to evaluate cartilaginous structures. Fast spin-echo sagittal, axial and coronal T2 fat-saturated or sagittal and coronal STIR images are crucial to demonstrate edema within the substance of knee ligaments
- Note sagittal proton-density MRI slice showing intact ACL (above)
- ACL is aligned along the Blumensaat line or oblique line corresponding the intercondylar roof of Femoral condyles. Lack of such alignment by the ACL is significant for ACL tear
Imaging Dx of Internal Derangement
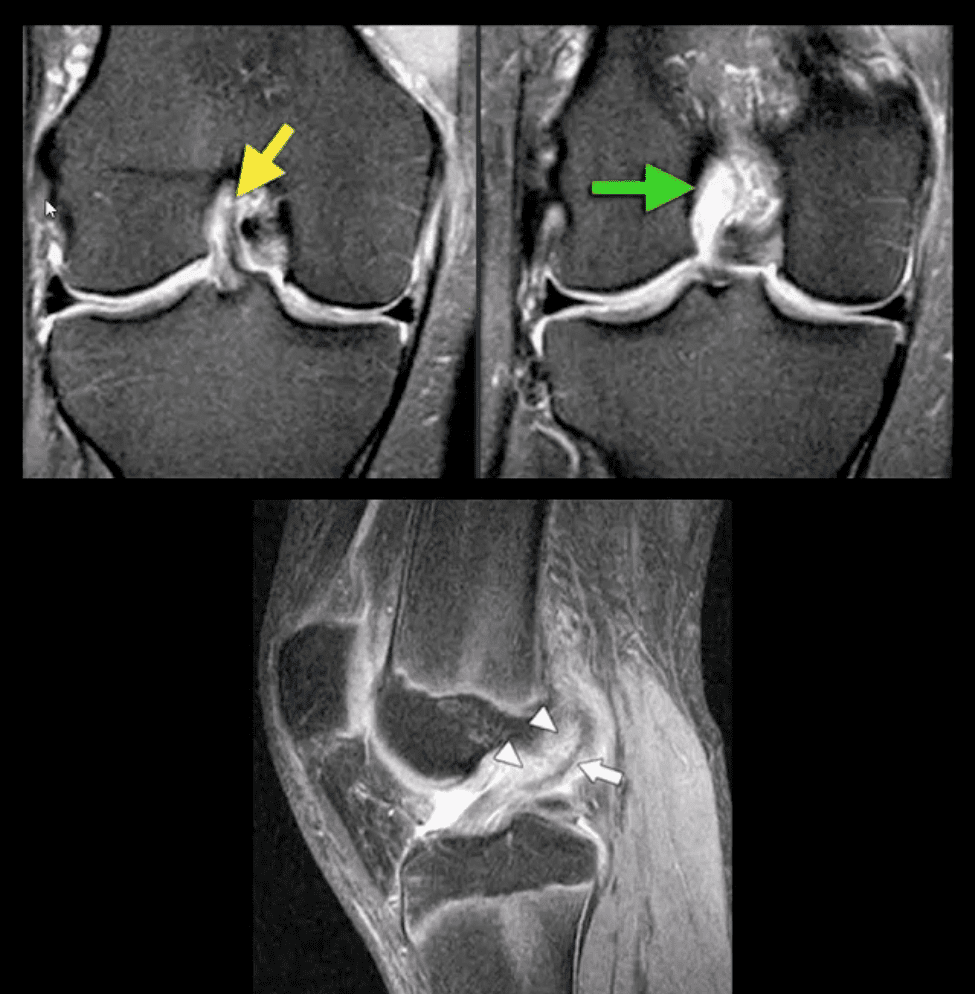
- MRI shows 78-100% sensitivity and 78-100% specificity
- Primary signs of ACL tear: non-visualization of ACL (above green arrow), loss of its axis along the Blumensaat line (above triangle heads), wavy appearance and substance tear (above white arrow) or edema and cloud-like indistinctness (above yellow arrow)
Reliable Secondary Signs of ACL Tear
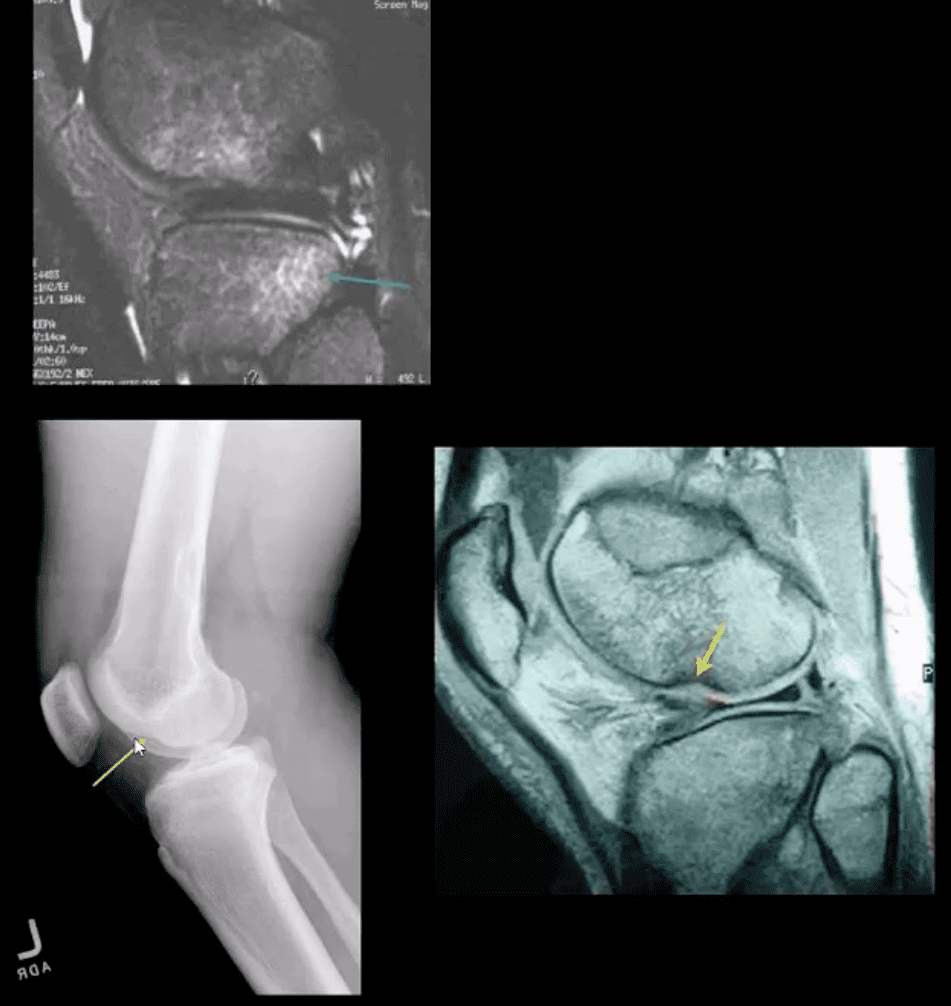
- May be observed on the radiographs and MRI
- Segond avulsion fracture (80% specificity for ACL tear) (next slide)
- Deep femoral notch sign indicating osteochondral fracture (above bottom images) and
- Pivot -shift bone marrow edema in the posterolateral tibial condyle d/t external rotation and often valgus impact by the lateral femoral condyles (above top image)
Segond Fracture (Avulsion by ITB)
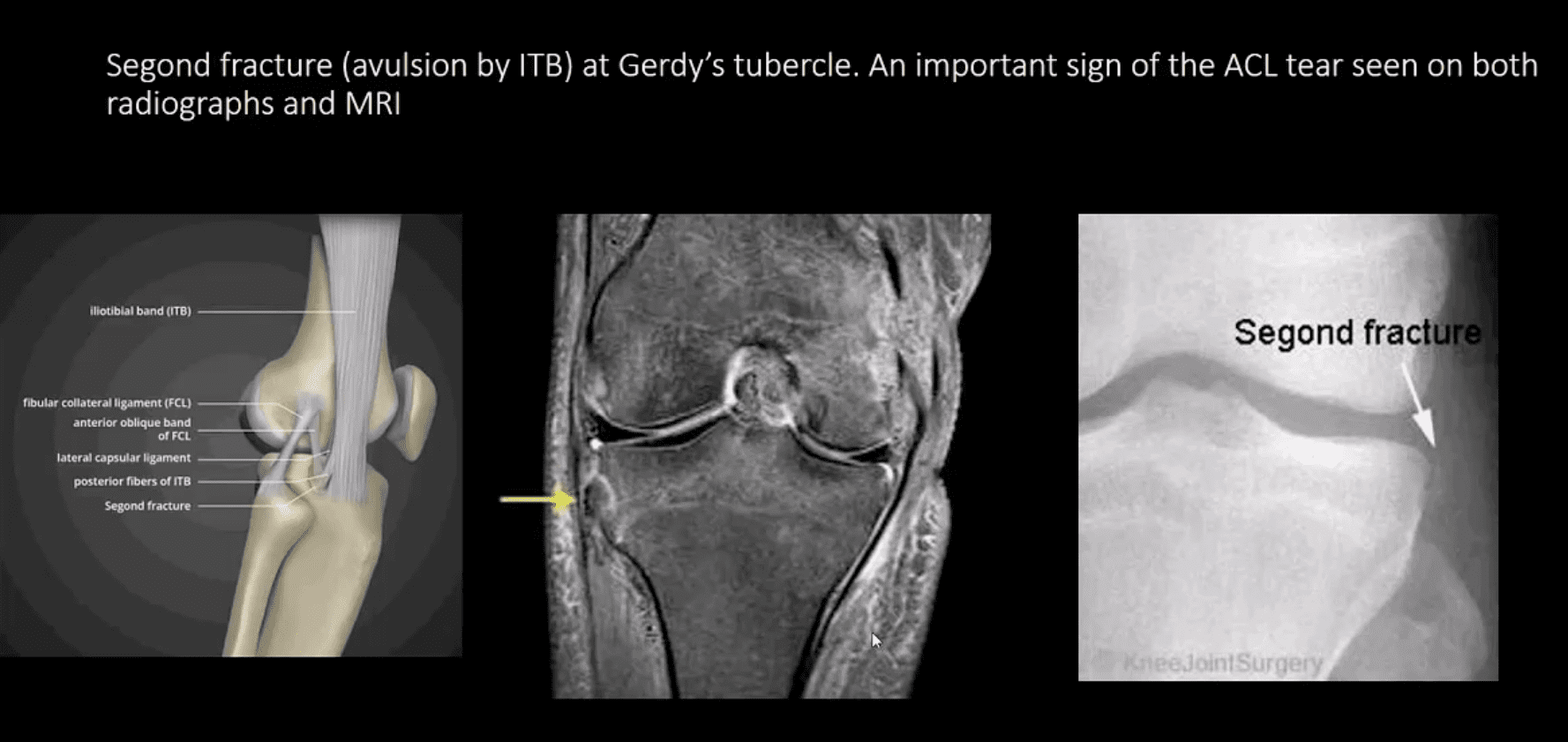
- Segond fracture at Gerdy’s tubercle. A vital sign of the ACL tear seen on both radiographs and MRI
Management of ACL Tears
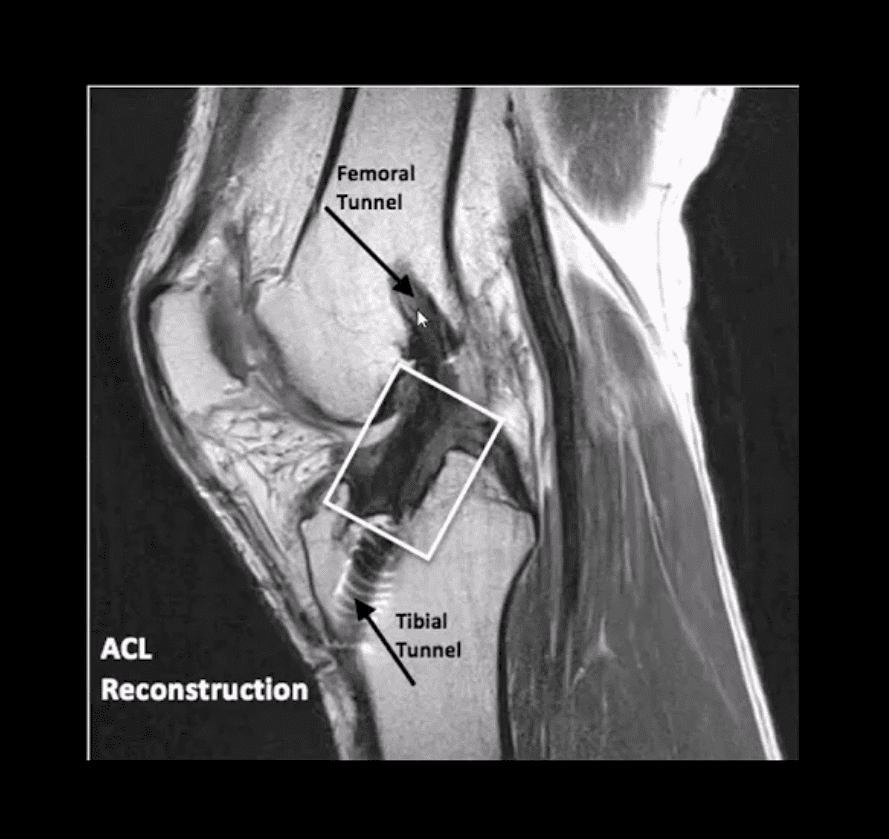
- In acute cases, usually operative using cadaveric or autograft (patella ligament or hamstring) ACL reconstruction
- Complications: graft tear, instability and premature DJD, joint stiffness d/t lack of postoperative rehab or gaft shortening. More rare, infection, a formation of intraosseous synovial cysts, etc.
Knee Trauma
General Disclaimer, Licenses and Board Certifications *
Professional Scope of Practice *
The information herein on "Knee Pain & Acute Trauma Diagnosis Imaging Part I | El Paso, TX" is not intended to replace a one-on-one relationship with a qualified health care professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional.
Blog Information & Scope Discussions
Welcome to El Paso's Premier Wellness and Injury Care Clinic & Wellness Blog, where Dr. Alex Jimenez, DC, FNP-C, a Multi-State board-certified Family Practice Nurse Practitioner (FNP-BC) and Chiropractor (DC), presents insights on how our multidisciplinary team is dedicated to holistic healing and personalized care. Our practice aligns with evidence-based treatment protocols inspired by integrative medicine principles, similar to those on this site and on our family practice-based chiromed.com site, focusing on naturally restoring health for patients of all ages.
Our areas of multidisciplinary practice include Wellness & Nutrition, Chronic Pain, Personal Injury, Auto Accident Care, Work Injuries, Back Injury, Low Back Pain, Neck Pain, Migraine Headaches, Sports Injuries, Severe Sciatica, Scoliosis, Complex Herniated Discs, Fibromyalgia, Complex Injuries, Stress Management, Functional Medicine Treatments, and in-scope care protocols.
Our information scope is multidisciplinary, focusing on musculoskeletal and physical medicine, wellness, contributing etiological viscerosomatic disturbances within clinical presentations, associated somato-visceral reflex clinical dynamics, subluxation complexes, sensitive health issues, and functional medicine articles, topics, and discussions.
We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for musculoskeletal injuries or disorders.
Our videos, posts, topics, and insights address clinical matters and issues that are directly or indirectly related to our clinical scope of practice.
Our office has made a reasonable effort to provide supportive citations and has identified relevant research studies that support our posts. We provide copies of supporting research studies upon request to regulatory boards and the public.
We understand that we cover matters that require an additional explanation of how they may assist in a particular care plan or treatment protocol; therefore, to discuss the subject matter above further, please feel free to ask Dr. Alex Jimenez, DC, APRN, FNP-BC, or contact us at 915-850-0900.
We are here to help you and your family.
Blessings
Dr. Alex Jimenez, DC, MSACP, APRN, FNP-BC*, CCST, IFMCP, CFMP, ATN
email: [email protected]
Multidisciplinary Licensing & Board Certifications:
Licensed as a Doctor of Chiropractic (DC) in Texas & New Mexico*
Texas DC License #: TX5807, Verified: TX5807
New Mexico DC License #: NM-DC2182, Verified: NM-DC2182
Multi-State Advanced Practice Registered Nurse (APRN*) in Texas & Multi-States
Multi-state Compact APRN License by Endorsement (42 States)
Texas APRN License #: 1191402, Verified: 1191402 *
Florida APRN License #: 11043890, Verified: APRN11043890 *
Colorado License #: C-APN.0105610-C-NP, Verified: C-APN.0105610-C-NP
New York License #: N25929, Verified N25929
License Verification Link: Nursys License Verifier
* Prescriptive Authority Authorized
ANCC FNP-BC: Board Certified Nurse Practitioner*
Compact Status: Multi-State License: Authorized to Practice in 40 States*
Graduate with Honors: ICHS: MSN-FNP (Family Nurse Practitioner Program)
Degree Granted. Master's in Family Practice MSN Diploma (Cum Laude)
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
My Digital Business Card
Licenses and Board Certifications:
DC: Doctor of Chiropractic
APRNP: Advanced Practice Registered Nurse
FNP-BC: Family Practice Specialization (Multi-State Board Certified)
RN: Registered Nurse (Multi-State Compact License)
CFMP: Certified Functional Medicine Provider
MSN-FNP: Master of Science in Family Practice Medicine
MSACP: Master of Science in Advanced Clinical Practice
IFMCP: Institute of Functional Medicine
CCST: Certified Chiropractic Spinal Trauma
ATN: Advanced Translational Neutrogenomics
Memberships & Associations:
TCA: Texas Chiropractic Association: Member ID: 104311
AANP: American Association of Nurse Practitioners: Member ID: 2198960
ANA: American Nurse Association: Member ID: 06458222 (District TX01)
TNA: Texas Nurse Association: Member ID: 06458222
NPI: 1205907805
| Primary Taxonomy | Selected Taxonomy | State | License Number |
|---|---|---|---|
| No | 111N00000X - Chiropractor | NM | DC2182 |
| Yes | 111N00000X - Chiropractor | TX | DC5807 |
| Yes | 363LF0000X - Nurse Practitioner - Family | TX | 1191402 |
| Yes | 363LF0000X - Nurse Practitioner - Family | FL | 11043890 |
| Yes | 363LF0000X - Nurse Practitioner - Family | CO | C-APN.0105610-C-NP |
| Yes | 363LF0000X - Nurse Practitioner - Family | NY | N25929 |
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
My Digital Business Card