Hips Positioning & MRI Anatomy
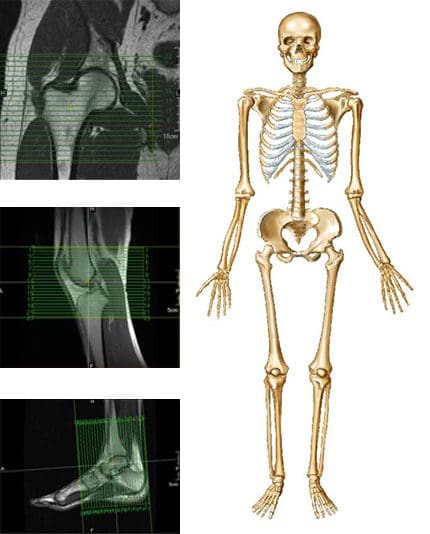 MRI may be requested for:
MRI may be requested for:
- Bone tumor
- Osteoarthritis
- Aseptic or avascular necrosis
- Bursitis
- Pain
Contents
Bones & Cartilage Of The Hips
The hips joints join the legs to the trunk of the body, and are formed by the femurs and pelvic bones. The hips are ball-and-socket type joints, where the femoral head (ball) fits into the cup-shaped acetabulum (socket) of the pelvis (Figure 1). When compared to the shoulder, which is also a ball-and-socket joint, the acetabulum is a deeper socket, and encompasses a greater area of the ball, or femoral head. This accommodation is necessary to provide stability for the hip, as it is a major weight-bearing joint, and one of the largest joints in the body. When not weight-bearing, the ball and socket of the hip joint are not perfectly fitted. However, as the hip joint bears more weight, the surface area contact increases, and the joint becomes more stable. When in a standing position, the body�s center of gravity passes through the center of the acetabula. While walking, weight-bearing stresses on the hips can be five times a person�s body weight. Healthy hips can support your weight and allow for pain-free movement. Hip injuries or disease can cause changes that affect your gait, as well as changes that affect the ability of the hips to distribute weight bearing. Abnormal stress is then placed on the joints that are above and below the hips.
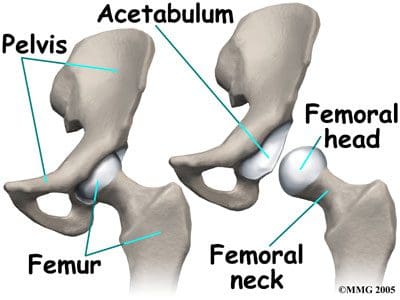
The three fused hips or innominate bones that form the acetabulum include the ilium, pubis, and ischium. The ilium forms the superior aspect, the pubis forms the inferior and anterior aspect, and the ischium forms the inferior and posterior aspect. The depth of the acetabulum socket is further increased by the attached fibrocartilaginous labrum (Figure 2). In addition to providing stability to the hip joint, the labrum allows flexibility and motion. Hip joint stability can be hampered by injuries resulting from playing sports, running, overuse, or falling, as well as by disease or tumor. MRI of the hips may be ordered to assess the joint(s) for internal derangement, fracture, or degenerative joint disease. A blow to the hip joint or a fall can result in dislocation of the hip, or a hip fracture. Osteoporosis or low bone density can also lead to hip fractures. Successful prevention and/or treatment of osteoporosis may be achieved through nutrition (adequate amounts of calcium, vitamin D and phosphorus), exercise, safety measures, and medications.
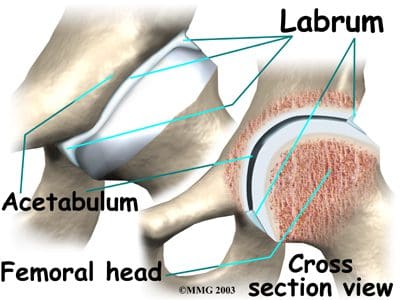
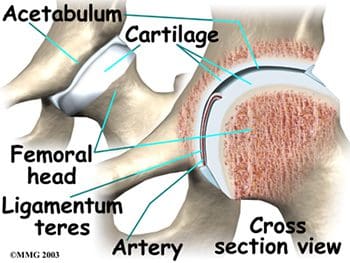
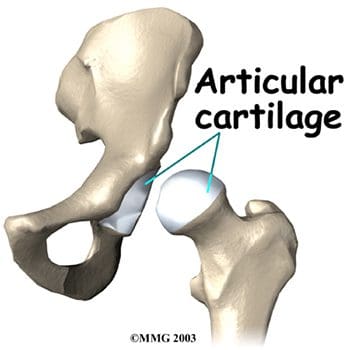
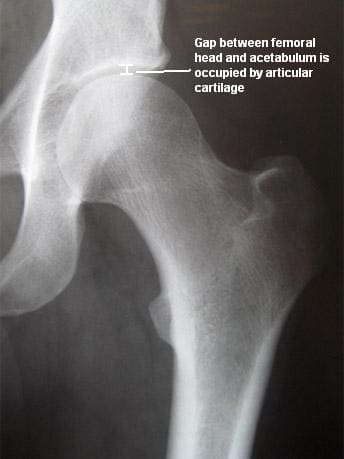
Articular cartilage covers the femoral head and the acetabulum (Figure 3). This cartilage is thin but tough, flexible, smooth and slippery, with a rubbery consistency. It absorbs shock, and allows the bones to move against each other easily and without pain. It is kept lubricated by synovial fluid, which is made in the synovial membrane (joint lining). Synovial fluid is both viscous and sticky. This fluid is what allows us to flex our joints under great pressure without wear. The articular cartilage of the hip is typically about � inch thick, except in the posterior aspect of the hip socket (Figure 4). Here, the cartilage is thicker, as this area absorbs most of the force during walking, running, and jumping. MRI of the hip joint can detect problems involving both the articular cartilage and the fibrocartilaginous ring, or labrum. Cartilage has minimal blood vessels, so it is not good at repairing itself. Fraying, fissuring, and other abnormalities or defects of the cartilage can lead to arthritis in the hip joint. Contrast can be directly injected in the hip joint for a detailed look at the cartilage and labrum.
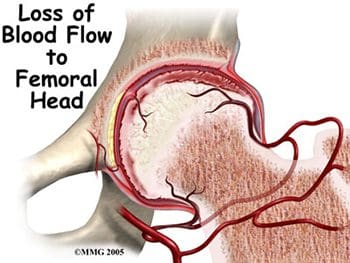
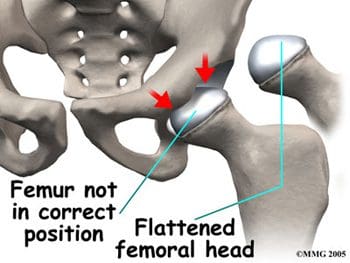
The femurs are the longest bones in the body, with large round heads that rotate and glide within the acetabula of the pelvis. The femoral head is particularly subject to pathologic changes if there is any significant alteration of blood supply (avascular necrosis). The femoral neck connects the head of the femur to the shaft. The neck ends at the greater and lesser trochanters, which are sites of muscle and tendon attachments. A disease characterized by an inadequate blood supply to the femoral head is Legg-Calve-Perthes disease, also known as LCP or simply Perthes disease. This is a degenerative disease of the hip joint that affects children, most commonly seen in boys ages two through twelve. One of the growth plates of the femoral head, the capital femoral epiphysis, is inside the joint capsule of the hip. Blood vessels that feed this epiphysis run along the side of the femoral neck, and are in danger of being torn or �pinched off� if the growth plate is damaged. This can result in a loss of blood supply to the epiphysis, leading to a deformity of the femoral head (Figure 5). The femoral head may become unstable and break easily, which can lead to incorrect healing and deformities of the entire hip joint (Figure 6). Treatment of Perthes disease is centered on the goal of returning the femoral head to a normal shape. Surgical and non-surgical treatments are used, based on the idea of �containment�- holding the femoral head in the acetabulum as much as possible, while still allowing motion of the hip joint for cartilage nutrition and healthy growth of the joint.
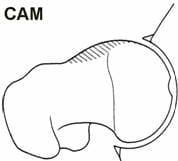
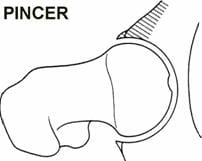
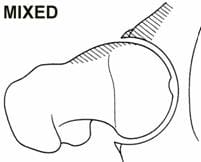
High level athletes and active individuals may be susceptible to a hip condition known as Femoro-Acetabular Impingement, or FAI. FAI is characterized by excessive friction in the hip joint. The femoral head and acetabulum rub abnormally, and can create damage to the articular or labral cartilage. FAI is also associated with labral tears, early hip arthritis, hyperlaxity and low back pain. FAI generally occurs in two forms: Cam and Pincer. The Cam form results in abnormal contact between the femoral head and the socket of the hip because the femoral head and neck relationship is aspherical (Figure 7). Males and those involved in significant contact sports typically display Cam impingement. Pincer impingement occurs when the acetabulum covers too much of the femoral head, resulting in the labral cartilage being pinched between the rim of the socket and the anterior femoral head-neck junction (Figure 8). Pincer impingement may be more common in women. Typically, these two forms exist together, and are labeled as �mixed impingement� (Figure 9).
Ewing�s sarcoma is a malignant bone tumor that may affect the pelvis and/or femur, thereby also affecting the stability of the hips. Like Perthes disease, Ewing�s sarcoma is more common in males, typically presenting in childhood or early adulthood. MRI is routinely used in the work-up of these malignant tumors to show bony and soft tissue extent of the tumor, and its relation to nearby anatomic structures (Figure 10). Contrast may be used to help determine the amount of necrosis within the tumor, which aids in determining the response to treatment before surgery.
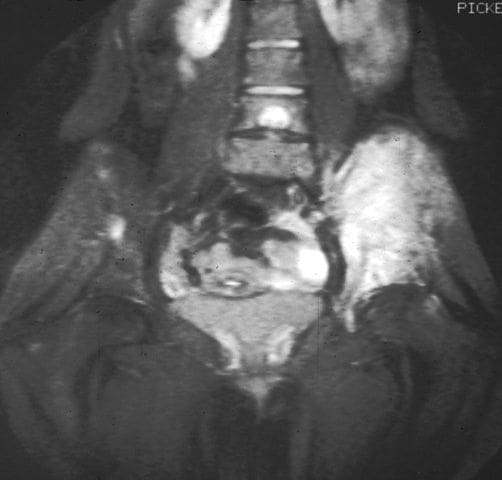
Figure 10. MRI demonstrating Ewing�s sarcoma.
Ligaments Of The Hips
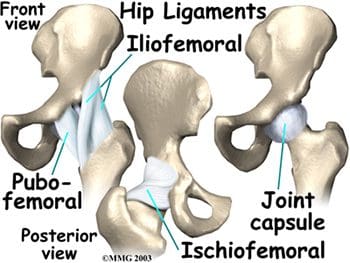
Hip stability is further increased by three strong ligaments that encompass the hip joint and form the joint capsule. These ligaments connect the femoral head to the acetabulum, with names suggestive of the bones they connect. They include the pubofemoral and iliofemoral ligaments anteriorly, and the ischiofemoral ligament posteriorly (Figure 11). The iliofemoral ligament is the strongest ligament in the body. However, sports and overuse can still result in sprains of these sturdy ligaments of the joint capsules of the hips. A smaller ligament, the ligamentum teres, is an intracapsular ligament that connects the tip of the femoral head to the acetabulum (Figure 12). A small artery within this ligament brings some of the blood supply to the femoral head. Damage to the ligamentum teres, and its enclosed artery, can result in avascular necrosis.
Muscles & Tendons Of The Hips
The muscles of the thigh and lower back work together to keep the hip stable, in alignment, and able to move. The hip gains stability because the hip muscles do not attach right at the joint. Hip muscles allow the movements of flexion, extension, abduction, adduction, and medial and lateral rotation. To better understand the functions of the muscles surrounding the hip, they can be divided into groups based on their locations- anterior, posterior, and medial.
The anterior thigh muscles are the main hip flexors, and are located anterior to the hip joint. Seventy percent of the thigh�s muscle mass is made up of the quadriceps femoris muscle, so named because it arises from four muscle heads- the rectus femoris, vastus medialis, vastus intermedius, and vastus lateralis (Figures 13, 14). The rectus femoris is the only one of the �quad� muscles to cross the hip joint. The sartorius muscle is found anterior to the quadriceps, and also serves as an abductor and lateral rotator of the hip. The most powerful of the anterior thigh hip flexors is the iliopsoas, which originates in the low back and pelvis and attaches at the lesser trochanter.
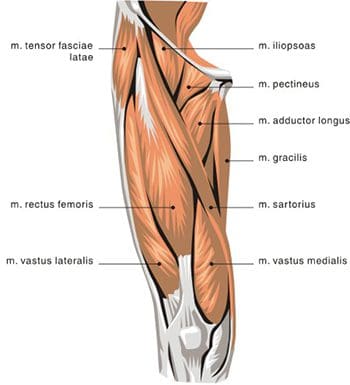
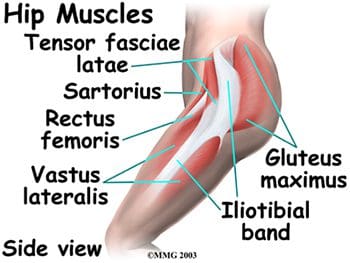
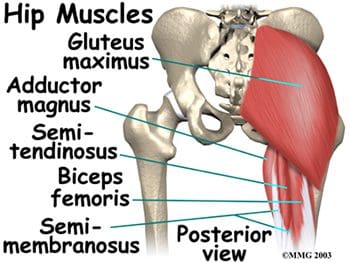
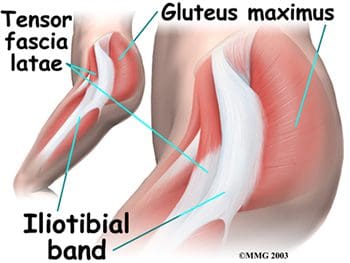
Posterior hip muscles include those of both the thigh and gluteal regions. The posterior thigh muscles are also known as the hamstrings- semimembranosus, semitendinosus, and biceps femoris (Figure 15). These muscles originate at the inferior pelvis, and are the extensors for the hip. They are active in normal walking motions. When the hamstrings are �tight�, they limit hip flexion when the knee joint is extended (bending forward from the waist with knees straight), and can limit lumbar movement, leading to back pain. The gluteal muscles include the gluteus maximus, medius, and minimus, six deep muscles that serve as lateral rotators, and the tensor fasciae latae. The three gluteals and the anterior sartorius muscle are all involved in abduction. The gluteus maximus is the main hip extensor, and is the most superficial of the gluteal muscles. It is involved in running and walking uphill, and assists with normal tone of the iliotibial band, which lies lateral to it. The gluteus medius and minimus both insert at the greater trochanter of the femur. The minimus is the deepest of the three gluteal muscles. Anterior to the gluteus minimus is the tensor fasciae latae muscle. It is a flexor and medial rotator of the hip, originating from the anterior superior iliac spine (ASIS) and inserting on the iliotibial band. The term �tensor fasciae latae� defines this muscle�s job- �muscle that stretches the band on the side�. This muscle helps the iliopsoas, gluteus medius, and gluteus minimus muscles during flexion, abduction and medial rotation of the thigh by making the iliotibial band taut, thereby steadying the trunk and stabilizing the hip (Figure 16). The iliotibial band or tract is not a muscle, but a thickened, fibrous band of deep fascia, or connective tissue. It is found at the lateral aspect of the thigh, and runs from the ilium to the tibia. It encloses the muscles and helps with lateral stabilization of the knee joint, as well as helping to maintain both hip and knee extension. Tightening of the iliotibial (IT) band typically causes more problems at the knee as opposed to the hip, but hip pain can result from the IT band rubbing as it passes over the greater trochanter.
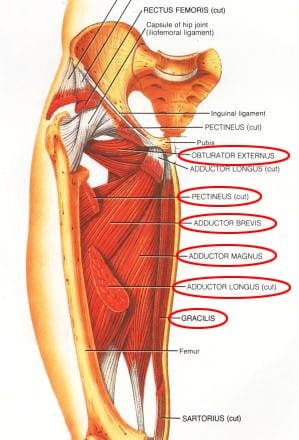
The medial thigh (groin) muscles include five muscles of adduction, and one lateral rotator (Figures 17, 18). The lone lateral rotator is the obturator externus, which covers the external surface of the obturator foramen in the deep upper medial thigh. The adductors include the gracilis, the pectineus, and the adductor brevis, longus and magnus. The gracilis is the longest adductor, extending from the medial inferior aspect of the pubic bone, to the medial aspect of the tibia. The adductor magnus is the most massive of the medial muscles of the thigh.
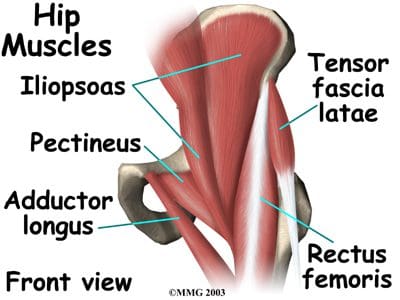
The tendons and muscles of the hips are very powerful and create great forces, making them prone to inflammation and irritation. Tendonitis of the hip can result from repetitive movements involving the soft tissues surrounding the hip joint. Overuse of the hip joint in fitness workouts can lead to tendonitis. Tendons lose their elasticity as we age, resulting in swelling and irritation when the tendons are no longer �gliding� on their normal paths. Iliopsoas tendonitis plays a major role in snapping hip syndrome, or dancer�s hip. A snapping sensation when the hip is flexed and extended may be accompanied by an audible snapping or popping noise, as well as pain. This can be both an extra-articular and an intra-articular occurrence. Extra-articular snapping is often found in those patients with a leg length difference (the longer leg is symptomatic), those with tightness of the iliotibial band on the involved side, and those with weak hip abductors and external rotators. Lateral extra-articular snapping can be caused by the iliotibial band, tensor fascia latae or gluteus medius tendon as they slide back and forth across the greater trochanter (Figure 19). If any of these connective tissue bands thickens, they can �catch� on the greater trochanter during the motion of hip extension, thereby creating the �snapping� sensation and sound. Medial extra-articular snapping, which is less common, can occur when the iliopsoas tendon catches on the anterior inferior iliac spine, lesser trochanter, or iliopectineal ridge during hip extension. Intra-articular snapping hip syndrome is similar in many ways to the extra-articular type, but often involves an underlying mechanical problem in the lower extremity, and more intense pain. Intra-articular snapping may be indicative of a torn acetabular labrum, recurrent hip subluxation, a tear of the ligamentum teres, loose bodies, articular cartilage damage, or synovial chondromatosis (cartilage formations in the synovial membrane of the joint). Snapping hip syndrome is usually found in those ages 15-40, often in those in training for the military. It can also affect athletes, especially those involved in dance, gymnastics, soccer, and track and field. These athletes will all be performing repeated hip flexions, which can lead to tendonitis in the hip area. The repetitive motions of those involved in weightlifting and running generally lead to a thickening of the tendons in the hip region, rather than snapping hip syndrome. Prevention, or at least a lessening, of this syndrome may be found with increased stretching of the iliopsosas muscle or the iliotibial band. Surgery is usually not required, unless intra-articular pathology is present.
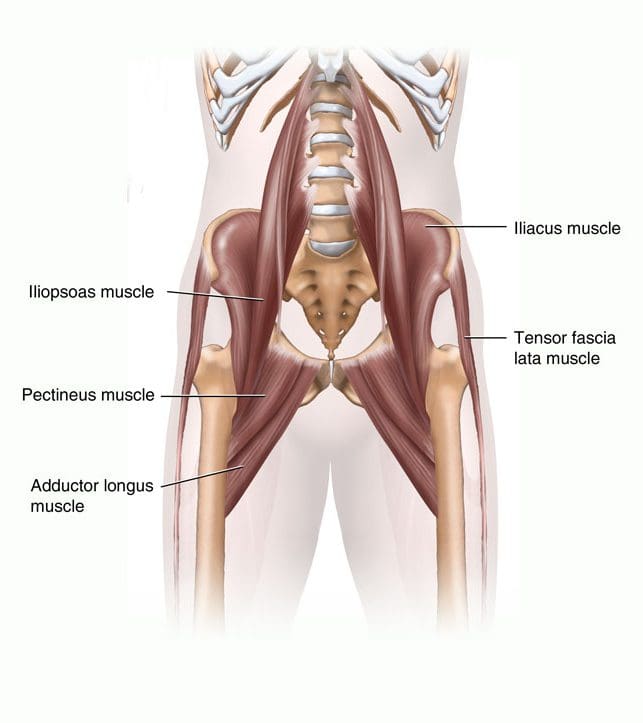
Figure 19. Hip muscles.
Tendon or muscle strains can occur suddenly, as in sports injuries, or they can develop over time, with symptoms including pain, swelling, muscle spasms, and difficulty moving certain muscles. MRI can be used to detect tendon and muscle tears and strains, as well as bone tumors and infection. MRI has shown good accuracy for the diagnosis of tears of the gluteus medius and gluteus minimus tendons, which are both abductor tendons of the hip. An association was found between these tears and areas of high signal intensity superior or lateral to the greater trochanter on T2-weighted images, tendon elongation in the gluteus medius, and tendon discontinuity (Figure 20). STIR and fat-suppressed T2-weighted coronal images are very sensitive for detection of areas of high signal intensity superior to the greater trochanter. Coronal T1-weighted images demonstrate tendon elongation in the gluteus medius (Figure 21). Axial images may prove superior for localizing involvement to individual abductor tendons and confirming tendon discontinuity (Figure 22). Tears of the abductor tendons may be the leading cause of greater trochanteric pain syndrome.
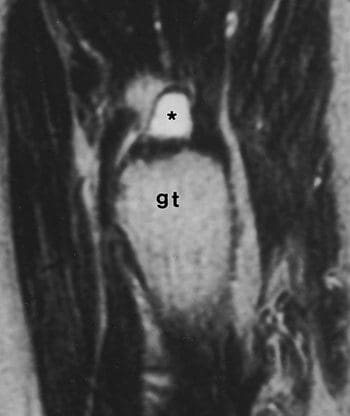
Figure 20. Sag. T2 shows high signal intensity superior to greater trochanter (gt) corresponding to swollen bursa (*).
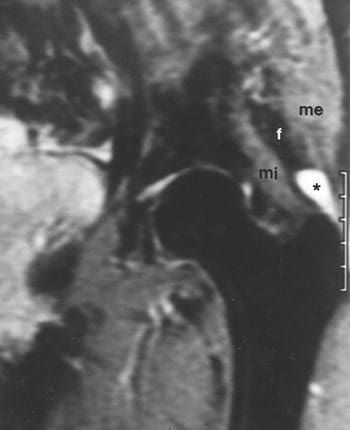
Figure 21. Coronal STIR shows high signal intensity superior to greater trochanter in bursa (*) between gluteus medius (me) and gluteus minimus (mi) tendons.
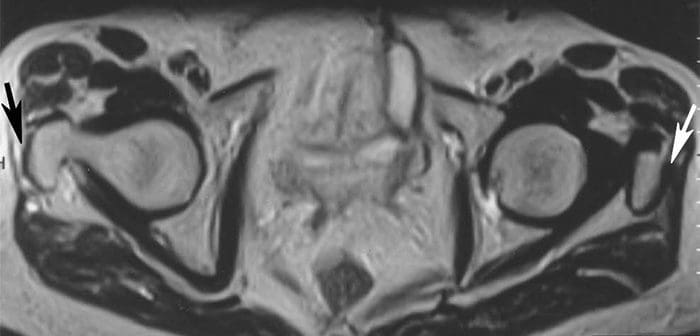
Figure 22. Axial T2 shows high signal intensity corresponding to fluid replacing distal rt. gluteus medius tendon (black arrow); normal left tendon (white arrow).
Nerves Of The Hips
The nerves of the hip supply the various muscles in the hip area. The major nerves include the femoral, obturator, and lateral femoral cutaneous nerves anteriorly, and the large sciatic nerve posteriorly (Figure 23). The femoral nerve innervates the quadriceps femoris and sartorius, and is the sensory nerve to the anterior thigh. Trauma to this nerve usually occurs in the pelvis, as it passes through or near the psoas muscle. The obturator nerve passes along the lateral pelvic wall and through the obturator foramen, then splits into branches that supply the adductor muscle group. This nerve can also be subject to trauma in the pelvis due to its passage through the obturator foramen. The lateral femoral cutaneous nerve is a sensory nerve that travels along the anterolateral aspect of the thigh. It supplies sensation to the skin surface of the thigh. This is the single nerve involved in a painful condition called meralgia paresthetica, which is characterized by tingling, numbness, and burning pain in the outer part of the thigh. Meralgia paresthetica results from focal entrapment of the lateral femoral cutaneous nerve as it passes through the tunnel formed by the lateral attachment of the inguinal ligament and the ASIS. The posterior sciatic nerve passes deep to the gluteus maximus into the posterior thigh, where it innervates the hamstring muscles, on its way down to the lower leg and foot. The sciatic nerve is approximately as big around as the thumb, and is the largest single nerve in the human body. It can be injured in cases of posterior hip dislocation. Pressure on this nerve can cause nerve pain, numbness, tingling and weakness (sciatica symptoms) in the buttocks, leg, or foot, depending on the site of origin of the sciatic nerve compression.

Figure 23. Anterior and posterior views of the nerves of the hip.
Arteries & Veins Of The Hips
The arterial blood vessels that supply the hips are branches of the internal and external iliacs. The internal iliac artery gives off the superior and inferior gluteals, and the obturator artery. The inferior gluteal flows to the posterior aspect of the hip joint and proximal femur, where it joins a branch of the femoral artery. The obturator artery runs through the obturator foramen, and sends its acetabular branch to the ligamentum teres as part of the blood supply to the femoral head. The external iliac becomes the femoral artery, which has numerous branches that supply the hip and proximal femur. The largest femoral branch is the profunda femoris, which branches superiorly into the medial and lateral circumflex femorals (Figure 24). The circumflex femorals and the inferior gluteal artery contribute to the anastomoses to supply the femoral head, femoral neck, and the hip joint. The medial circumflex also has an acetabular branch to the ligamentum teres. Congenital anomalies in the hip anastomoses, degenerative processes, and trauma can all compromise the blood supply to the hip joint area.
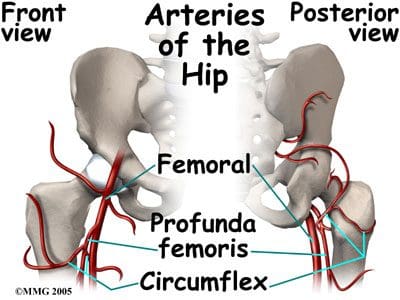
Figure 24. Anterior and posterior views of the arteries of the hip.
Venous flow in the hip and proximal femur typically follows the arterial flow, including the same names for the vessels. The deep veins of the hip and thigh can be the origination of a deep vein thrombosis, which can result in a pulmonary embolus. This can be caused by immobility after hip surgery, sitting in cars or airplanes for extended trips, being overweight, or slow or low blood flow. These blood clots can break off, travel through the larger veins of the thigh and hip, continue through the heart, and become lodged in the smaller vessels of the lung. MRI is being used more frequently to diagnose this very serious condition.
Bursae Of The Hips
The hip joint is surrounded by bursae, similar to the shoulder. These fluid-filled sacs are lined with a synovial membrane, which produces synovial fluid. Their function is to lessen the friction between tendon and bone, ligament and bone, tendons and ligaments, and between muscles. There may be as many as 20 bursae around the hip. If they become infected or inflamed, the result is a painful condition called bursitis. Common hip bursae that may become inflamed include the greater trochanteric bursa, the iliopsoas bursa, and the ischial bursa (Figure 25). The greater trochanteric bursa is sandwiched between the greater trochanter of the femur, and the muscles and tendons that cross over it. If this bursal sac becomes inflamed, patients experience pain with every step they take, as each step requires the tendon to move over the femur at the hip joint. A tight iliotibial band can also cause irritation of the greater trochanteric bursa. Iliopsoas bursitis can result from irritation of the bursa found between the hip joint and the iliopsoas muscle that passes in front of it. Another common site for bursitis is the ischial bursa, which acts as a lubricating pad between tendons and the ischial tuberosity, which is the bony prominence of the pelvis that you sit on. The ischial bursa acts to prevent destruction of the tendons as they move over the ischial tuberosity. Prolonged sitting can cause ischial bursitis. Inflammation around the ischial tuberosity can irritate the sciatic nerve, and trigger symptoms similar to sciatica. Hip bursitis is seen in runners and athletes in sports that involve excessive running (soccer, football, etc.). It can also be caused by an injury (traumatic bursitis), and is seen in post-op hip replacement and hip surgery patients. Treatment for hip bursitis typically includes rest, anti-inflammatory medications, and ice. It may become necessary to aspirate the bursa, which can be combined with a cortisone injection. MRI may be needed if the diagnosis is unclear, or if the problem does not resolve with normal treatments.
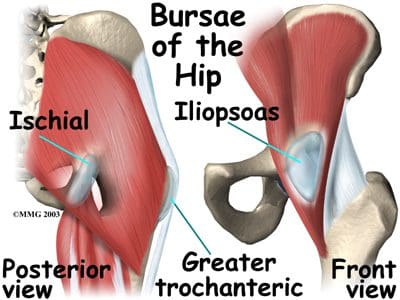
Figure 25. Bursae of the hip.
Axial Scans
When positioning unilateral axial slices for the hip, a coronal image can be used to ensure inclusion of all pertinent anatomy. The slices should extend superiorly to include the entire femoral head and acetabulum, and inferiorly to include anatomy below the lesser trochanter. The slices should be aligned perpendicular to the shaft of the femur, as seen in the coronal image in Figure 39.
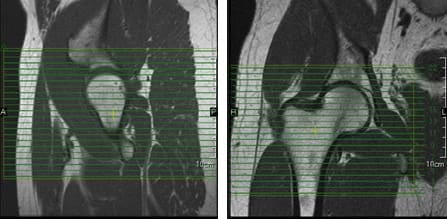
Figure 39. Axial slice setup using sagittal and coronal images.
For bilateral axial hip slice setup, parameters may have to be altered to maintain adequate resolution with the larger FOV that is required (Figure 40). The slice group may require angulation to maintain alignment of the femoral heads on the resultant images.
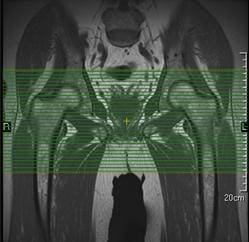
Figure 40. Bilateral axial slice setup using a coronal image.
Coronal Scans
Coronal slices of the hip should cover the area from the posterior margin to the anterior margin of the femoral head. The area from the proximal margin of the femoral shaft to the greater sciatic notch should be included in the image (Figure 41). Slices may be angled so that they are parallel to the femoral neck. Thinner slices may be requested for coronal scanning.
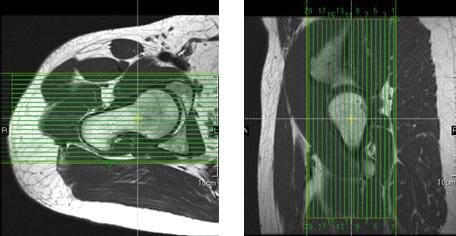
Figure 41. Coronal slice setup using axial and sagittal images.
Sagittal Scans
Sagittal slices of the hip should extend past the greater trochanter laterally, and through the acetabulum medially. The slices should be aligned along the long axis of the femur, and perpendicular to the coronal slices, as seen in the coronal image in Figure 42. Two different slice groups will be necessary when performing bilateral sagittal scans.
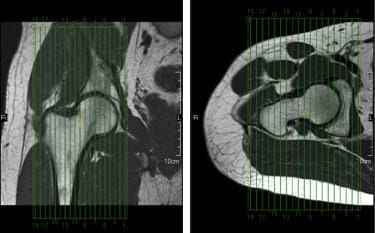
Figure 42. Sagittal slice setup using coronal and axial images.
Hips Arthrography
MR hip arthrography is often times referred to as the gold standard for assessment of the labrum of the hip. The most clinically significant abnormal findings that result from hip arthrography are labral detachments and tears. Detachment of the labrum, which is more common than a labral tear, can be diagnosed from the appearance of the injected contrast at the acetabular-labral interface (Figure 43). A labral tear can result in injected contrast appearing within the substance of the labrum (Figure 44). Contrast injection is necessary to differentiate torn or detached labra from other pathologic conditions, which may have separate signal intensities. The sensitivity and accuracy for the diagnosis of labral tears and detachment with MR arthrography vs. nonarthrographic MR is 90%. Hip arthrography with MR can also depict intrarticular loose bodies, osteochondral abnormalities, and abnormalities of soft-tissue structures.
Hip arthrography can be performed under fluoro in the x-ray dept., with the patient being moved to the MRI dept. for further imaging, or the entire procedure can be performed in the MRI suite, if MR compatible supplies are available for interventional techniques. The patient should be securely positioned with the hips in internal rotation.
T1-weighted imaging is performed post-contrast to visualize the high signal of the intraarticular contrast. T1 gradient echo sequences offer the benefits of thin sections, elimination of partial volume averaging, and increased detection of small tears. Fatsat sequences are helpful in increasing the contrast between the injected contrast and the adjacent soft tissue. STIR or fatsat T2 sequences performed in the coronal plane may help to detect unsuspected pathologic conditions in the soft tissue and adjacent osseous structures.
Post-contrast axial oblique images have been shown to optimize the detection of the most common sports-related acetabular labral tears, which are anterior or anterosuperior in location. Using a mid-coronal localizer, the axial oblique slices should be prescribed parallel to the long axis of the femoral neck.
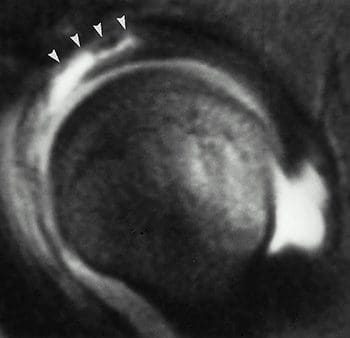
Figure 43. Labral detachment as seen in a fat-suppressed T1-wtd. sag. image; arrowheads indicate involvement of anterior and anterosuperior labrum.
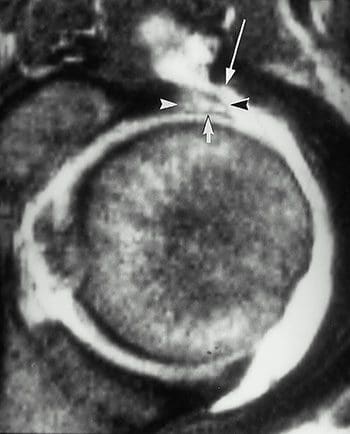
Figure 44. Labral tear as seen in a T1-wtd. image; arrowheads indicate enlarged labrum; short arrow indicates linear intralabral collection of contrast material; long arrow indicates communication between the joint and the iliopsoas bursa.
blank
References:
Kapit, Wynn, and Lawrence M. Elson. The Anatomy Coloring Book. New York: HarperCollins, 1993.
Hip Anatomy, Function, and Common Problems. (Last updated 28July2010). Retrieved from http://healthpages.org/anatomy-function/hip-structure-function-common-problems/
Cluett, J. M.D. (Updated 22May2012). Labral Tear of the Hip Joint. Retrieved from http://orthopedics.about.com/od/hipinjuries/qt/labrum.htm
Hughes, M. D.C. (15July2010). Diseases of the Femur Bone. Retrieved from http://www.livestrong.com/article/175599-diseases-of-the-femur-bone/
A Patient�s Guide to Perthes Disease of the hip. (n.d.). Retrieved from http://www.orthopediatrics.com/docs/Guides/perthes.html
Hip Injuries and Disorders. (Last reviewed 10February2012). Retrieved from http://nlm.nih.gov/medlineplus/hipinjuriesanddisorders.html
Ligament of head of femur. (Updated 20December2011). Retrieved from http://en.wikipedia.org/wiki/Ligament_of_head_of_femur
Ewing�s sarcoma. (Last modified 06January2012). Retrieved from http://en.wikipedia.org/wiki/Ewing%27s_sarcoma
Hip Anatomy. (n.d.). Retrieved from http://www.activemotionphysio.ca/Injuries-Conditions/Hip
Iliotibial Band Friction Syndrome. (n.d.). Retrieved from http://www.physiotherapy-treatment.com/iliotibial-band-friction-syndrome.html
Snapping hip syndrome. (Last modified 09November2011). Retrieved from http://en.wikipedia.org/wiki/Snapping_hip_syndrome
Sekul, E. (Updated 03February2012). Meralgia Paresthetica. Retrieved from http://emedicine.medscape.com/article/1141848-overview
Yeomans, S. D.C. (Updated 07July2010). Sciatic Nerve and Sciatica. Retrieved from http://www.spine-health.com/conditions/sciatica/sciatic-nerve-and-sciatica
Mayo Clinic staff. (26July2011). Meralgia paresthetica. Retrieved from http://www.mayoclinic.com/health/meralgia-paresthetica/DS00914
Deep Vein Thrombosis (DVT)-Blood Clots in the Legs. (n.d.). Retrieved from http://catalog/nucleusinc.com/displaymonograph.php?MID=148
Petersilge, C. M.D. (03May2000). Chronic Adult Hip Pain: MR Arthrography of the Hip. Retrieved from http://radiographics.rsna.org/content/20/suppl_1/S43.full
Acetabular branch of medial circumflex femoral artery. (Last modified 17November2011). Retrieved from http://en.wikipedia.org/wiki/Acetabular_branch_of_medial_circumflex_femoral_artery
Cluett, J. M.D. (Updated 26March2011). Hip Bursitis. Retrieved from http://orthopedics.about.com/cs/hipsurgery/a/hipbursitis.htm
Steinbach, L. M.D., Palmer, W. M.D., Schweitzer, M. M.D. (10June2002). Special Focus Session MR Arthrography. Retrieved from http://radiographics.rsna.org/content/22/5/1223.full
Schueler, S. M.D., Beckett, J.M.D., Gettings, S.M.D. (Last updated 05August2010). Ischial Bursitis/Overview. Retrieved from http://www.freemd.com/ischial-bursitis/overview.htm
Hwang, B., Fredericson, M., Chung, C., Beaulieu, C., Gold, G. (29October2004). MRI Findings of Femoral Diaphyseal Stress Injuries in Athletes. Retrieved from http://www.ajronline.org/content/185/1/166.full.pdf
The Femur (Thigh Bone). (n.d.). Retrieved from http://education.yahoo.com/reference/gray/subjects/subject/59
Norman, W. PhD, DSc. (n.d.). Joints of the Lower Limb. Retrieved from http://home.comcast.net/~wnor/lljoints.htm
Femur. (Last modified 24September2012). Retrieved from http://en.wikipedia.org/wiki/Femur
Wheeless, C. III, M.D. (Last updated 25April2012). Ligaments of Humphrey and Wrisberg. Retrieved from http://wheelessonline.com/ortho/ligaments_of_humphrey_and_wrisberg
Muscle Strains in the Thigh. (Last reviewed August2007). Retrieved from http://orthoinfo.aaos.org/topic.cfm?topic=A00366
Shiel, W. Jr., M.D. (Last reviewed 23July2012). Hamstring Injuries. Retrieved from http://www.medicinenet.com/hamstring_injury/article.htm
Hamstring Muscle Injuries. (Last reviewed July 2009). Retrieved from http://orthoinfo.aaos.org/topic.cfm?topic=a00408
Knee. (Last modified 19September2012). Retrieved from http://en.wikipedia.org/wiki/Knee
DeBerardino, T. M.D. (Updated 30March2012). Quadriceps Injury. Retrieved from http://emedicine.medscape.com/article/91473-overview
Kan, J.H. (n.d.). Osteochondral Abnormalities: Pitfalls, Injuries, and Osteochondritis Dissecans. Retrieved from http://www.arrs.org/shopARRS/products/s11p_sample.pdf
Nerves of the Lower Limb. (Last updated 30March2006). Retrieved from http://download.videohelp.com/vitualis/med/lowrnn.htm
The Adductor Canal. (Last updated 30March2006). Retrieved from http://download.videohelp.com/vitualis/med/addcanal.htm
Nabili, S. M.D. (n.d.). Varicose Veins & Spider Veins. Retrieved from http://www.medicinenet.com/varicose_veins/article.htm
Basic Venous Anatomy. (n.d.). Retrieved from http://vascular-web.com/asp/samples/sample104.asp
Femoral nerve. (Last modified 23September2012). Retrieved from http://en.wikipedia.org/wiki/Femoral_nerve
Peron, S. RDCS. (Last modified 16October2010). Anatomy � Lower Extremity Veins. Retrieved from http://www.vascularultrasound.net/vascular-anatomy/veins/lower-extremity-veins
Medical Multimedia Group, L.L.C. (n.d.). Knee Anatomy. Retrieved from http://www.eorthopod.com/content/knee-anatomy
Knee Joint Anatomy, Function and Problems. (Last updated 06July2010). Retrieved from http://healthpages.org/anatomy-function/knee-joint-structure-function-problems/
Coronary ligament of the knee. (Last modified 09May2010). Retrieved from http://en.wikipedia.org/wiki/Coronary_ligament_of_the_knee
Walker, B. (n.d.). Patellar Tendonitis Treatment � Jumper�s Knee. Retrieved from http://www.thestretchinghandbook.com/archives/patellar-tendonitis.php
Osgood-Schlatter disease. (Last reviewed 12November2010). Retrieved from http://www.ncbi.nlm.nih.gov/pubmedhealth/PMH0002238/
Grelsamer, R. M.D. (n.d.). The Anatomy of the Patella and the Extensor Mechanism. Retrieved from http://kneehippain.com/patient_pain_anatomy.php
Oblique popliteal ligament. (Last modified 24March2012). Retrieved from http://en.wikipedia.org/wiki/Oblique_popliteal_ligament
Shiel, W. Jr., M.D. (Last reviewed 27July2012). Chondromalacia Patella (Patellofemoral Syndrome). Retrieved from http://www.medicinenet.com/patellofemoral_syndrome/article.htm
Knee. (Last modified 19September2012). Retrieved from http://en.wikipedia.org/wiki/Knee
Mosher, T. M.D. (Last updated 11April2011). MRI of Knee Extensor Mechanism Injuries Overview of the Knee Extensor Mechanism. Retrieved from http://emedicine.medscape.com/article/401001-overview
Carroll, J. M.D. (December 2007). Oblique Menisco-meniscal Ligament. Retrieved from http://radsource.us/clinic/0712
DeBerardino, T. M.D. (Last updated 30March2012). Medial Collateral Knee Ligament Injury. Retrieved from http://emedicine.medscape.com/article/89890-overview#a0106
Farr, G. (Last updated 31December2007). Joints and Ligaments of the Lower Limb. Retrieved from http://becomehealthynow.com/article/bodyskeleton/951/
Knee anatomy overview. (02March2008). Retrieved from http://www.kneeguru.co.uk/KNEEnotes/node/741
Dixit, S. M.D., Difiori, J. M.D., Burton, M. M.D., Mines, B. M.D. (15January2007). Management of Patellofemoral Pain Syndrome. Retrieved from http://www.aafp.org/afp/2007/0115/p194.html
Knee Muscles. (Last updated 05September2012). Retrieved from http://www.knee-pain-explained.com/kneemuscles.html
Popliteus muscle. (Last updated 20February2012). Retrieved from http://en.wikipedia.org/wiki/Popliteus_muscle
Kneedoc. (10February2011). Nerves. Retrieved from http://thekneedoc.co.uk/neurovascular/nerves
Wheeless, C. III, M.D. (Last updated 15December2011). Popliteal Artery. Retrieved from http://wheelessonline.com/ortho/popliteal_artery
The Popliteal Artery. (n.d.) Retrieved from http://education.yahoo.com/reference/gray/subjects/subject/159
Knee bursae. (Last updated 09May2012). Retrieved from http://en.wikipedia.org/wiki/Bursae_of_the_knee_joint
Hirji, Z., Hunjun, J., Choudur, H. (02May2011). Imaging of the Bursae. Retrieved from http://www.ncbi.nlm.nih.gov/pmc/articles/PMC3177464/
Kimaya Wellness Limited. (n.d.). Organ>Popliteal Artery. Retrieved from http://kimayahealthcare.com/OrganDetail.aspx?OrganID=103&AboutID=1
Total Vein Care. (Last updated 24February2012). Varicose Vein Anatomy and Function for Patients. Retrieved from http://www.veincare.com/education/
Tibia. (Last updated 01April2012). Retrieved from http://en.wikipedia.org/wiki/Tibia
Norkus,S., Floyd, R. (Published 2001). The Anatomy and Mechanisms of Syndesmotic Ankle Sprains. Retrieved from http://www.ncbi.nlm.nih.gov/pmc/articles/PMC155405/
Soleus muscle. (Last updated 10April2012). Retrieved from http://en.wikipedia.org/wiki/Soleus_muscle
Achilles Tendinitis. (Last reviewed June2010). Retrieved from http://orthoinfo.aaos.org/topic.cfm?topic=A00147
Wheeless, C. III,M.D. (Last updated 11April2012). Sural Nerve. Retrieved from http://wheelessonline.com/ortho/sural_nerve
Medical Multimedia Group, L.L.C. (Last updated 26July2006). Ankle Syndesmosis Injuries. Retrieved from http://www.orthogate.org/patient-education/ankle/ankle-syndesmosis-injuries.html
Cluett, J. M.D. (Last updated 16September2008). Exertional Compartment Syndrome. Retrieved from http://orthopedics.about.com/od/overuseinjuries/a/compartment.htm
Leg Veins (Thigh, Lower Leg) Anatomy, Pictures and Names. (Last updated 21November2010). Retrieved from http://www.healthype.com/leg-veins-thigh-lower-leg-anatomy-pictures-and-names.html
Cluett, J.M.D. (Last updated 6October2009). Stress Fracture. Retrieved from http://orthopedics.about.com/cs/otherfractures/a/stressfracture.htm
Ostlere, S. (1December2004). Imaging the ankle and foot. Retrieved from http://imaging.birjournals.org/content/15/4/242.full
Inverarity, L. D.O. (Last updated 23January2008). Ligaments of the Ankle Joint. Retrieved from http://physicaltherapy.about.com/od/humananatomy/p/ankleligaments.htm
Golano, P., Vega, J., DeLeeuw, P., Malagelada, F.,Manzanares, M., Gotzens, V., van Dijk, C. (Published online 23March2010). Anatomy of the ankle ligaments:a pictorial essay. Retrieved from http://www.ncbi.nlm.nih.gov/pmc/articles/PMC2855022/
Numkarunarunrote, N., Malik, A., Aguiar, R.,Trudell, D., Resnick, D. (11October2006). Retinacula of the Foot and Ankle: MRI with Anatomic Correlation in Cadavers. Retrieved from http://www.ajronline.org/content/188/4/W348.full
Medical Multimedia Group, L.L.C. (n.d.). A Patient�s Guide to Ankle Anatomy. Retrieved from http://www.eorthopod.com/content/ankle-anatomy
The Anterior Tibial Artery. (n.d.). Retrieved from http://education.yahoo.com/reference/gray/subjects/subject/160
Foot and Ankle Anatomy. (Last updated 28July2011). Retrieved from http://northcoastfootcare.com/pages/Foot-and-Ankle-Anatomy.html
Donnelly, L., Betts, J., Fricke, B. (1July2009). Skimboarder�s Toe: Findings on High-Field MRI. Retrieved from http://www.ajronline.org/content/184/5/1481.full
Foot. (Last updated 28August2012). Retrieved from http://en.wikipedia.org/wiki/Foot
Wiley, C. (n.d.). Major Ligaments in the Foot. Retrieved from http://www.ehow.com/list_6601926_major-ligaments-foot.html
Turf Toe: Symptoms, Causes, and Treatments. (Last reviewed 9August2012). Retrieved from http://www.webmd.com/fitness-exercise/turf-toe-symptoms-causes-and-treatments
Cluett, J. M.D. (Last updated 02April2012). Turf Toe. Retrieved from http://orthopedics.about.com/od/toeproblems/p/turftoe.htm
Neurology and the Feet. (n.d.) Retrieved from http://footdoc.ca/www.FootDoc.ca/Website%20Nerves%20Of%20The%20Feet.htm
The Veins of the Lower Extremity, Abdomen, and Pelvis. (n.d.). Retrieved from http://education.yahoo.com/reference/gray/subjects/subject/173
Corley, G., Broderick, B., Nestor, S., Breen, P., Grace, P., Quondamatteo, F., O�Laighin, G. (n.d.). The Anatomy and Physiology of the Venous Foot Pump. Retrieved from http://www.eee.nuigalway.ie/documents/go_anatomy_of_the_plantar_venous_plexus_manuscript.pdf
Morton�s neuroma. (Last modified 8August2012). Retrieved from http://en.wikipedia.org/wiki/Morton%27s_metatarsalgia
Close Accordion
blank
References Anatomy Pics:
Figures 1, 5, 6, 24- http://www.orthopediatrics.com/docs/Guides/perthes.html
Figures 2, 3, 11, 12, 14, 15, 16, 18, 23, 25- http://www.activemotionphysio.ca/Injuries-Conditions/Hip/Hip-Anatomy/a~299/article.html
Figure 4- http://hipkneeclinic.com/images/uploaded/hipanatomy_xray.jpg
Figures 7, 8, 9- http://hipfai.com/
Figure 10- http://en.wikipedia.org/wiki/File:Ewing%27s_sarcoma_MRI_nci-vol-1832-300.jpg
Figure 13- http://www.chiropractic-help.com/Patello-Femoral-Pain-Syndrome.html
Figure 17- http://www.thestretchinghandbook.com/archives/ezine_images/adductor.jpg
Figure 19- http://media.summitmedicalgroup.com/media/db/relayhealth-images/hipanat.jpg
Figures 20-22- http://www.ajronline.org/content/182/1/137.full.pdf+html
Figure 43, 44- http://radiographics.rsna.org/content/20/suppl_1/S43.full
Figure 45- http://www.exploringnature.org/db/detail.php?dbID=24&detID=2768
Figures 46-48- http://www.ajronline.org/content/185/1/166.full.pdf
Figure 49- http://arrs.org/shopARRS/products/s11p_sample.pdf
Figure 50- http://www.thestretchinghandbook.com/archives/medial-collateral-ligament.php
Figures 51, 52- http://www.radsource.us/clinic/0712
Figures 53, 54- http://www.osteo-path.co.uk/BodyMap/Thighs.html
Figure 55- http://www.ncbi.nlm.nih.gov/pmc/articles/PMC1963576/
Figure 56- http://legacy.owensboro.kctcs.edu/gcaplan/anat/Notes/API%20Notes%20M%20%20Peripheral%20Nerves.htm
Figure 57- http://www.keywordpictures.com/keyword/lateral%20cutaneous%20nerve%20of%20thigh/
Figure 58- http://home.comcast.net/~wnor/postthigh.htm
Figure 59- http://becomehealthynow.com/glossary/CONG437.htm
Figure 60- http://fitsweb.uchc.edu/student/selectives/Luzietti/Vascular_pvd.htm
Figure 61- http://www.fashion-res.com/peripheral-vascular-disease-with-stenting-in-the/
Figure 62- http://www.wpclipart.com/medical/anatomy/blood/femoral_artery_and_branches_in_leg.png.html
Figure 63- http://www.globalteleradiologyservices.com/Deep_Vein_Thrombosis_Overview.htm
Figure 64- http://www.vascularultrasound.net/vascular-anatomy/veins/lower-extremity-veins
Figure 82- http://www.jeffersonhospital.org/diseases-conditions/knee-ligament-injury.aspx?disease=658f267f-75ab-4bde-8781-f2730fafa958
Figure 83- http://javierjuan.ifunnyblog.com/anatomybackofknee/
Figure 84- http://www.kneeandshouldersurgery.com/knee-disorders/tibial-osteotomy.html
Figure 85- http://www.disease-picture.com/chondromalacia-patella-physical-therapy/
Figure 86- http://www.eorthopod.com/content/bipartite-patella
Figure 87- http://www.orthogate.org/patient-education/knee/articular-cartilage-problems-of-the-knee.html
Figure 88- http://www.webmd.com/pain-management/knee-pain/menisci-of-the-knee-joint
Figure 89- http://sumerdoc.blogspot.com/2008_07_01_archive.html
Figure 90- http://www.concordortho.com/patient-education/topic-detail-popup.aspx?topicID=55befba2d440dc8e25b85747107b5be0
Figure 91- http://trialx.com/curebyte/2011/08/16/pictures-for-chondromalacia-patella/
Figure 92- http://radiopaedia.org/images/1059
Figure 93- http://radiologycases.blogspot.com/2011/01/osgood-schlatter-disease.html
Figure 94- http://www.physioquestions.com/2010/09/07/knee-injury-acl-part-i/
Figure 95- http://www.jeffersonhospital.org/diseases-conditions/knee-ligament-injury.aspx?disease=4e3fcaf5-0145-43ea-820f-a175e586e3c8
Figures 96, 97- http://radiology.rsna.org/content/213/1/213.full
Figures 98-101- http://appliedradiology.com/Issues/2008/12/Articles/Imaging-the-knee–Ligaments.aspx
Figure 102- http://radiopaedia.org/images/408156
Figure 103- http://aftabphysio.blogspot.com/2010/08/joints-of-lower-limb.html
Figures 104, 105- http://www.radsource.us/clinic/0310
Figure 106- http://nwrunninglab.com/patellar-tendonitis.html
Figure 107- http://www.aafp.org/afp/2007/0115/p194.html
Figure 108- http://www.reboundsportspt.com/blog/tag/knee-pain
Figure 109- http://www.norwellphysicaltherapy.com/Injuries-Conditions/Knee/Knee-Issues/Quadriceps-Tendonitis-of-the-Knee/a~1803/article.html
Figure 110- http://kneeguru.co.uk/KNEEnotes/node/479
Figure 111- http://www.magicalrobot.org/BeingHuman/2010/03/fascia-bones-and-muscles
Figure 112- http://home.comcast.net/~wnor/postthigh.htm
Figures 113, 115, 157-159- http://ipodiatry.blogspot.com/2010/02/anatomy-of-foot-and-ankle_26.html
Figure 114- http://medchrome.com/basic-science/anatomy/the-knee-joint/
Figure 116- http://www.sharecare.com/question/what-are-varicose-veins
Figure 117- http://mendmyknee.com/knee-and-patella-injuries/anatomy-of-the-knee.php
Figures 118-120- http://www.ncbi.nlm.nih.gov/pmc/articles/PMC3177464/
Figure 121- http://www.riversideonline.com/health_reference/Disease-Conditions/DS00448.cfm
Figure 122- http://arthritis.ygoy.com/2011/01/01/what-is-an-arthritis-knee-cyst/
Figure 143- http://usi.edu/science/biology/mkhopper/hopper/BIOL2401/LABUNIT2/LabEx11week6/tibiaFibulaAnswer.htm
Figure 144- http://web.donga.ac.kr/ksyoo/department/education/grossanatomy/doc/html/fibula1.html
Figure 145- http://becomehealthynow.com/popups/ligaments_tib_fib_bh.htm
Figure 146- http://www.parkwayphysiotherapy.ca/article.php?aid=121
Figure 147- http://aidmyankle.com/high-ankle-sprains.php
Figure 148- http://legsonfire.wordpress.com/what-is-compartment-syndrome/
Figures 149, 152- http://www.stepbystepfootcare.ca/anatomy.html
Figures 150, 151- http://www.gla.ac.uk/ibls/US/fab/tutorial/anatomy/jiet.html
Figure 153- http://www.athletictapeinfo.com/?s=tennis+leg
Figure 154- http://radsource.us/clinic/0608
Figure 155- http://www.eorthopod.com/content/achilles-tendon-problems
Figure 156- http://achillesblog.com/assumptiondenied/not-a-rupture/
Figure 181- http://www.orthopaedicclinic.com.sg/ankle/a-patients-guide-to-ankle-anatomy/
Figure 182- http://www.activemotionphysio.ca/article.php?aid=47
Figure 183- http://www.ajronline.org/content/193/3/687.full
Figures 184, 186- http://www.eorthopod.com/content/ankle-anatomy
Figure 185- http://www.crossfitsouthbay.com/physical-therapy/learn-yourself-a-quick-anatomy-reference/ankle/
Figures 187, 227- http://www.activemotionphysio.ca/Injuries-Conditions/Foot/Foot-Anatomy/a~251/article.html
Figure 188- http://inmotiontherapy.com/article.php?aid=124
Figures 189, 190- http://home.comcast.net/~wnor/ankle.htm
Figure 191- http://skillbuilders.patientsites.com/Injuries-Conditions/Ankle/Ankle-Anatomy/a~47/article.html
Figure 192- http://metrosportsmed.patientsites.com/Injuries-Conditions/Foot/Foot-Anatomy/a~251/article.html
Figure 193- http://musc.edu/intrad/AtlasofVascularAnatomy/images/CHAP22FIG30.jpg
Figure 194- http://musc.edu/intrad/AtlasofVascularAnatomy/images/CHAP22FIG31B.jpg
Figure 195- http://veinclinics.com/physicians/appearance-of-vein-disease/
Figure 196- http://mdigradiology.com/services/interventional-services/varicose-veins.php
Figure 216- http://kidport.com/RefLib/Science/HumanBody/SkeletalSystem/Foot.htm
Figure 217- http://www.joint-pain-expert.net/foot-anatomy.html
Figure 218- http://www.thetoedoctor.com/turf-toe-symptoms-and-treatment/
Figures 219, 220- http://radsource.us/clinic/0303
Figure 221- http://www.ajronline.org/content/184/5/1481.full
Figure 222- http://www.answers.com/topic/arches
Figure 223- http://www.mayoclinic.com/health/medical/IM00939
Figure 224- http://radsource.us/clinic/0904
Figure 225- http://www.ortho-worldwide.com/anfobi.html
Figure 226- http://www.coringroup.com/lars_ligaments/patientscaregivers/your_anatomy/foot_and_ankle_anatomy/
Figure 228- http://www.stepbystepfootcare.ca/anatomy.html
Figure 229- http://iupucbio2.iupui.edu/anatomy/images/Chapt11/FG11_18aL.jpg
Figure 230- http://www.ajronline.org/content/184/5/1481.full.pdf
Figure 231- http://metrosportsmed.patientsites.com/Injuries-Conditions/Foot/Foot-Anatomy/a~251/article.html
Figure 232- http://www.painfreefeet.com/nerve-entrapments-of-the-leg-and-foot.html
Figures 233, 234- http://emedicine.medscape.com/article/401417-overview
Figure 235- http://web.squ.edu.om/med-Lib/MED_CD/E_CDs/anesthesia/site/content/v03/030676r00.HTM
Figure 236- http://www.nysora.com/peripheral_nerve_blocks/classic_block_tecniques/3035-ankle_block.html
Figure 237- http://ultrasoundvillage.net/imagelibrary/cases/?id=122&media=464&testyourself=0
Figure 238- http://www.joint-pain-expert.net/foot-anatomy.html
Figure 239- http://jap.physiology.org/content/109/4/1045.full
Figure 240- http://microsurgeon.org/secondtoe
Figure 241- http://elu.sgul.ac.uk/rehash/guest/scorm/406/package/content/common_iliac_veins.htm
Close Accordion
General Disclaimer, Licenses and Board Certifications *
Professional Scope of Practice *
The information herein on "Hips Positioning And MRI Anatomy" is not intended to replace a one-on-one relationship with a qualified health care professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional.
Blog Information & Scope Discussions
Welcome to El Paso's Premier Wellness and Injury Care Clinic & Wellness Blog, where Dr. Alex Jimenez, DC, FNP-C, a Multi-State board-certified Family Practice Nurse Practitioner (FNP-BC) and Chiropractor (DC), presents insights on how our multidisciplinary team is dedicated to holistic healing and personalized care. Our practice aligns with evidence-based treatment protocols inspired by integrative medicine principles, similar to those on this site and on our family practice-based chiromed.com site, focusing on naturally restoring health for patients of all ages.
Our areas of multidisciplinary practice include Wellness & Nutrition, Chronic Pain, Personal Injury, Auto Accident Care, Work Injuries, Back Injury, Low Back Pain, Neck Pain, Migraine Headaches, Sports Injuries, Severe Sciatica, Scoliosis, Complex Herniated Discs, Fibromyalgia, Chronic Pain, Complex Injuries, Stress Management, Functional Medicine Treatments, and in-scope care protocols.
Our information scope is multidisciplinary, focusing on musculoskeletal and physical medicine; wellness; contributing etiological viscerosomatic disturbances within clinical presentations; associated somato-visceral reflex clinical dynamics; subluxation complexes; sensitive health issues; and functional medicine articles, topics, and discussions.
We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and licensure jurisdiction. We use functional health & wellness protocols to treat and support care for musculoskeletal injuries or disorders.
Our videos, posts, topics, and insights address clinical matters and issues that directly or indirectly relate to our clinical scope of practice.
Our office has made a reasonable effort to provide supportive citations and has identified relevant research studies that support our posts. We provide copies of supporting research studies upon request to regulatory boards and the public.
We understand that we cover matters that require an additional explanation of how they may assist in a particular care plan or treatment protocol; therefore, to discuss the subject matter above further, please feel free to ask Dr. Alex Jimenez, DC, APRN, FNP-BC, or contact us at 915-850-0900.
We are here to help you and your family.
Blessings
Dr. Alex Jimenez, DC, MSACP, APRN, FNP-BC*, CCST, IFMCP, CFMP, ATN
email: [email protected]
Multidisciplinary Licensing & Board Certifications:
Licensed as a Doctor of Chiropractic (DC) in Texas & New Mexico*
Texas DC License #: TX5807, Verified: TX5807
New Mexico DC License #: NM-DC2182, Verified: NM-DC2182
Multi-State Advanced Practice Registered Nurse (APRN*) in Texas & Multi-States
Multi-state Compact APRN License by Endorsement (42 States)
Texas APRN License #: 1191402, Verified: 1191402 *
Florida APRN License #: 11043890, Verified: APRN11043890 *
Colorado License #: C-APN.0105610-C-NP, Verified: C-APN.0105610-C-NP
New York License #: N25929, Verified N25929
License Verification Link: Nursys License Verifier
* Prescriptive Authority Authorized
ANCC FNP-BC: Board Certified Nurse Practitioner*
Compact Status: Multi-State License: Authorized to Practice in 40 States*
Graduate with Honors: ICHS: MSN-FNP (Family Nurse Practitioner Program)
Degree Granted. Master's in Family Practice MSN Diploma (Cum Laude)
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
(Board Certified: Family Practice Nurse Practitioner—Multistate)*
(Licensed Nurse Practitioner & Chiropractor - Multistate)*
Clinical Director
Digital Business Card
Dr. Maria Cardenas, MD
(Board Certified: Internal Medicine)
(Licensed Medical Doctor)
Medical Director, Clinical Director & Collaborative Physician
NPI # 1164426749
MD License #: J2933
Licenses and Board Certifications:
MD: Medical Doctor
DC: Doctor of Chiropractic
APRNP: Advanced Practice Registered Nurse
FNP-BC: Family Practice Specialization (Multi-State Board Certified)
RN: Registered Nurse (Multi-State Compact License)
CFMP: Certified Functional Medicine Provider
MSN-FNP: Master of Science in Family Practice Medicine
MSACP: Master of Science in Advanced Clinical Practice
IFMCP: Institute of Functional Medicine
CCST: Certified Chiropractic Spinal Trauma
ATN: Advanced Translational Neutrogenomics
Memberships & Associations:
TCA: Texas Chiropractic Association: Member ID: 104311
AANP: American Association of Nurse Practitioners: Member ID: 2198960
ANA: American Nurse Association: Member ID: 06458222 (District TX01)
TNA: Texas Nurse Association: Member ID: 06458222
NPI: 1205907805
| Primary Taxonomy | Selected Taxonomy | State | License Number |
|---|---|---|---|
| No | 111N00000X - Chiropractor | NM | DC2182 |
| Yes | 111N00000X - Chiropractor | TX | DC5807 |
| Yes | 363LF0000X - Nurse Practitioner - Family | TX | 1191402 |
| Yes | 363LF0000X - Nurse Practitioner - Family | FL | 11043890 |
| Yes | 363LF0000X - Nurse Practitioner - Family | CO | C-APN.0105610-C-NP |
| Yes | 363LF0000X - Nurse Practitioner - Family | NY | N25929 |
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
(Board Certified: Family Practice Nurse Practitioner—Multistate)*
(Licensed Nurse Practitioner & Chiropractor - Multistate)*
Clinical Director
Digital Business Card
Dr. Maria Cardenas, MD
(Board Certified: Internal Medicine)*
(Licensed Medical Doctor)*
Medical Director, Clinical Director & Collaborative Physician
NPI # 1164426749
MD License #: J2933