
Venous Insufficiency: El Paso Back Clinic
Arteries carry blood from the heart to the rest of the body. The veins transport blood back to the heart, and the valves in the veins stop the blood from flowing backward. When the veins have difficulties sending blood from the limbs back to the heart, this is known as venous insufficiency. With this condition, the blood does not flow back properly to the heart, causing blood to accumulate in the veins of the legs. Chiropractic care, therapeutic massage, and functional medicine can increase and improve circulation and help manage symptoms.
Venous Insufficiency
The circulatory system is responsible for transporting blood, oxygen, and nutrients to the cells in the body. This system consists of the heart, arteries, veins, and capillaries. When blood circulation is restricted, it can lead to a buildup of toxins and waste products, which can cause various health problems, including fatigue, muscle cramps, and dizziness. Unhealthy circulation can also contribute to other health conditions like heart disease, stroke, and diabetes. The most common causes of venous insufficiency include:
- Blood clots
- Varicose veins
- A family history of venous insufficiency.
- Deep vein thrombosis.
- When forward flow through the veins is obstructed, such as in the case of a blood clot, blood builds up below the clot, which can lead to venous insufficiency.
- In varicose veins, the valves can be missing or damaged, and blood leaks back through the defective valves.
- In some cases, weakness in the leg muscles that push blood forward can also contribute to venous insufficiency.
- Venous insufficiency is more common in women than men and is more likely in adults over 50.
Circulation Symptoms
There are different symptoms associated with unhealthy circulation, and can include:
- Tingling or numbness in the extremities
- Cold hands and feet
- Pain or cramping in the muscles
- Weakness or fatigue
- Dizziness or lightheadedness
- Nausea
- Shortness of breath
- Erectile dysfunction
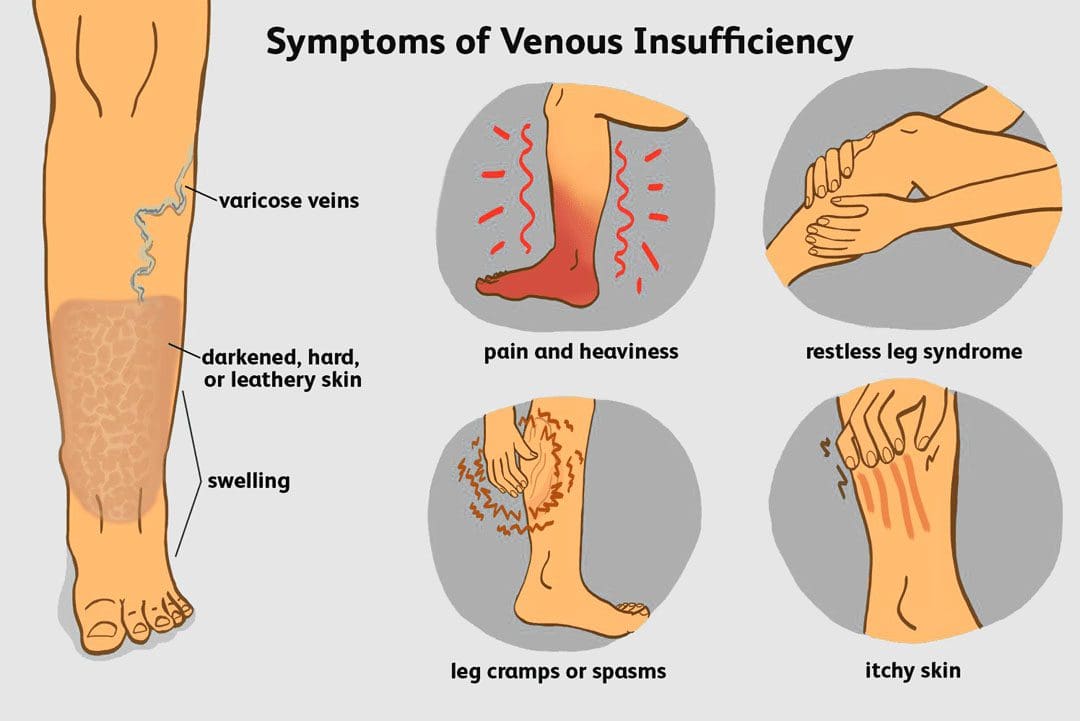
Symptoms of venous insufficiency include:
- Swelling of the legs or ankles – edema
- Pain that gets worse when standing and improves when raising the legs.
- Aching, throbbing, or a feeling of heaviness in the legs.
- A sense of tightness in the calves.
- Leg cramps
- Weak legs
- Itchy legs
- Thickening of the skin on the legs or ankles.
- Skin that is changing color, especially around the ankles
- Varicose veins
- Leg ulcers
Diagnosis
A doctor will perform a physical examination and take a complete medical history. They may order imaging tests to locate the source of the problem. These tests may include a venogram or a duplex ultrasound.
Venogram
- A doctor will insert an intravenous contrast dye into the veins.
- Contrast dye causes the blood vessels to appear opaque on the X-ray image, which helps the doctor see them on the image.
- This dye will give the doctor a clear image of the blood vessels.
Duplex Ultrasound
- A duplex ultrasound tests the speed and direction of blood circulation in the veins.
- A technician will place gel on the skin and press a small hand-held instrument on and around the area.
- The instrument uses sound waves that bounce back to a computer and produce images of blood circulation.
Treatment
Treatment will depend on various factors, including the reason for the condition and individual health status and history. Other factors a doctor will consider include:
- Specific symptoms
- Age
- The severity of the condition
- Medication and/or procedure tolerance
The most common treatment is prescription compression stockings.
- These special stockings apply pressure on the ankle and lower leg.
- They help improve blood circulation and reduce leg swelling.
- Compression stockings come in a range of prescription strengths and lengths.
Strategies
Treatments can include several methods.
Improving Circulation
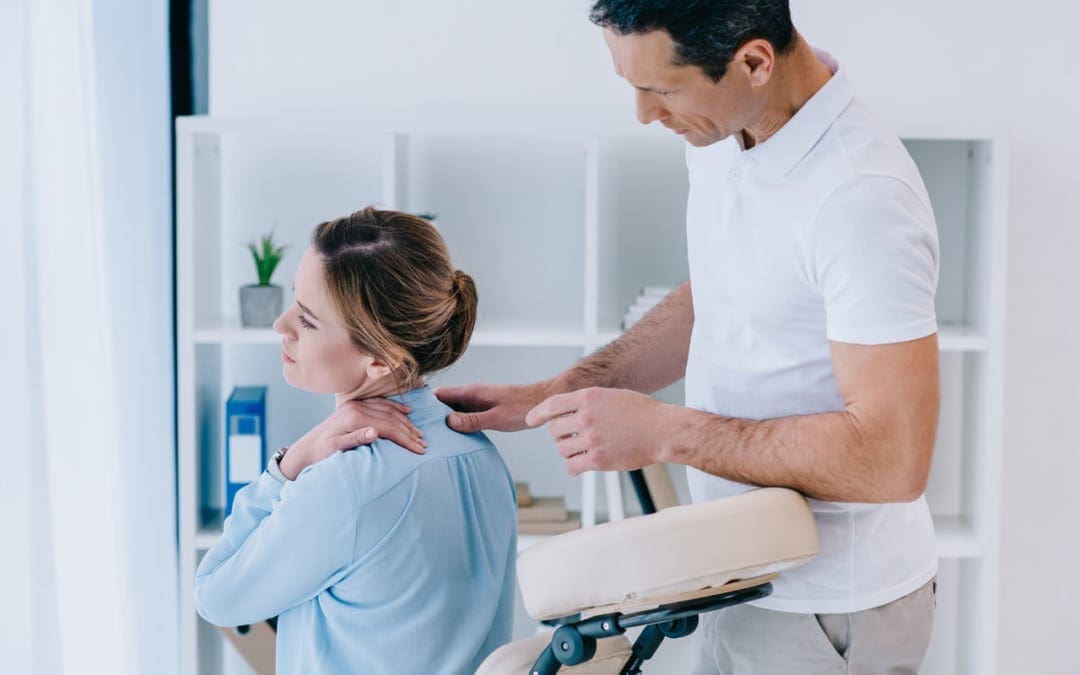
Chiropractic adjustments and vascular massage therapy on the legs can help improve blood circulation. Massage therapies such as vascular and lymphatic drainage massages aim to increase circulation, improve tissue nutrition, and can benefit patients with varicose veins and chronic venous insufficiency.
- The technique for lymphatic drainage involves light strokes to move lymph fluid into lymph vessels.
- The technique used to improve circulation involves short strokes to move blood from the valves to the veins.
However, massage therapy is not for all patients with vein diseases and conditions.
- Massage therapy is not recommended for patients with advanced-stage vein disease, in which large and bulging veins, ulcerations, and discoloration are present.
- Massaging the area could cause the weakened veins to burst, worsening the condition.
- Massage therapy is also unsafe for patients with deep vein thrombosis (DVT), as it could dislodge a clot and cause it to travel.
Medications
Medications may be prescribed. These include:
- Diuretics – medications that draw extra fluid from the body and are excreted through the kidneys.
- Anticoagulants – medicines that thin the blood.
- Pentoxifylline – medicine that helps improve blood circulation.
Surgery
More serious cases may require surgery. A doctor may suggest one of the following surgical procedures:
- Surgical repair of the veins or valves.
- Removing the damaged vein.
- Minimally invasive endoscopic surgery – The surgeon inserts a thin tube with a camera to see and tie off damaged veins.
- Laser surgery – A treatment that uses laser light to fade or close off damaged veins.
- Vein bypass – A healthy vein is transplanted from a different body area. Generally used only in the upper thigh and as a last option for severe cases.
Venous Insufficiency: What You Need To Know
References
Annamaraju P, Baradhi KM. Pentoxifylline. [Updated 2022 Sep 19]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2022 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK559096/
Chronic venous insufficiency. (n.d.). hopkinsmedicine.org/healthlibrary/conditions/cardiovascular_diseases/chronic_venous_insufficiency_85,P08250/
Evrard-Bras, M et al. “Drainage lymphatique manuel” [Manual lymphatic drainage]. La Revue du praticien vol. 50,11 (2000): 1199-203.
FIELDS, A. “Leg cramps.” California medicine vol. 92,3 (1960): 204-6.
Felty, Cindy L, and Thom W Rooke. “Compression therapy for chronic venous insufficiency.” Seminars in vascular surgery vol. 18,1 (2005): 36-40. doi:10.1053/j.semvascsurg.2004.12.010
Mayo Clinic Staff. (2017). Varicose veins.mayoclinic.org/diseases-conditions/varicose-veins/diagnosis-treatment/drc-20350649
Patel SK, Surowiec SM. Venous Insufficiency. [Updated 2022 Aug 1]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2022 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK430975/
Youn, Young Jin, and Juyong Lee. “Chronic venous insufficiency and varicose veins of the lower extremities.” The Korean journal of internal medicine vol. 34,2 (2019): 269-283. doi:10.3904/kjim.2018.230





 Nutritional Strategies: The focus of this paper is to explore better strategies for optimizing bone strength and reducing risk of fracture, while at the same time decreasing risk of cardiovascular disease. The majority of Americans do not consume the current recommended dietary allowance for calcium, and the lifetime risk of osteoporosis is about 50%. However, traditional mono-nutrient calcium supplements may not be ideal. We comprehensively and systematically reviewed the scientific literature in order to determine the optimal dietary nutritional strategies and nutritional supplements for long- term skeletal health and cardiovascular health. To summarize, the following steps may be helpful for building strong bones while maintaining soft and supple arteries: (1) calcium is best obtained from dietary sources rather than supplements; (2) ensure that adequate animal protein intake is coupled with calcium intake of 1000 mg/day; (3) maintain vitamin D levels in the normal range; (4) increase intake of fruits and vegetables to alkalinize the system and promote bone health; (5) concomitantly increase potassium consumption while reducing sodium intake; (6) consider increasing the intake of foods rich in vitamins K1 and K2; (7) consider including bones in the diet; they are a rich source of calcium-hydroxyapatite and many other nutrients needed for building bone.
Nutritional Strategies: The focus of this paper is to explore better strategies for optimizing bone strength and reducing risk of fracture, while at the same time decreasing risk of cardiovascular disease. The majority of Americans do not consume the current recommended dietary allowance for calcium, and the lifetime risk of osteoporosis is about 50%. However, traditional mono-nutrient calcium supplements may not be ideal. We comprehensively and systematically reviewed the scientific literature in order to determine the optimal dietary nutritional strategies and nutritional supplements for long- term skeletal health and cardiovascular health. To summarize, the following steps may be helpful for building strong bones while maintaining soft and supple arteries: (1) calcium is best obtained from dietary sources rather than supplements; (2) ensure that adequate animal protein intake is coupled with calcium intake of 1000 mg/day; (3) maintain vitamin D levels in the normal range; (4) increase intake of fruits and vegetables to alkalinize the system and promote bone health; (5) concomitantly increase potassium consumption while reducing sodium intake; (6) consider increasing the intake of foods rich in vitamins K1 and K2; (7) consider including bones in the diet; they are a rich source of calcium-hydroxyapatite and many other nutrients needed for building bone. Most vegetarians, especially vegans, appear to absorb less calcium because of the oxalic and phytic acid contained in many plant, grain and legume products.1 Indeed, several studies have reported that risks of bone fracture are higher in vegans�likely due, at least in part, to their lower dietary calcium intake, and/or poor absorption of this key mineral (table 1).21
Most vegetarians, especially vegans, appear to absorb less calcium because of the oxalic and phytic acid contained in many plant, grain and legume products.1 Indeed, several studies have reported that risks of bone fracture are higher in vegans�likely due, at least in part, to their lower dietary calcium intake, and/or poor absorption of this key mineral (table 1).21
 Maintaining replete magnesium status may reduce risk for the metabolic syndrome, diabetes, hypertension and MI.30 Circumstantial and experimental evidence has also implicated magnesium deficiency in osteoporosis.31�34 Optimal dietary magnesium intake is about 7�10 mg/ kg/day, preferably in the context of a net base-yielding diet, since a net acid-yielding diet increases excretion of both magnesium and calcium (table 2).
Maintaining replete magnesium status may reduce risk for the metabolic syndrome, diabetes, hypertension and MI.30 Circumstantial and experimental evidence has also implicated magnesium deficiency in osteoporosis.31�34 Optimal dietary magnesium intake is about 7�10 mg/ kg/day, preferably in the context of a net base-yielding diet, since a net acid-yielding diet increases excretion of both magnesium and calcium (table 2). Vitamin K2 intake has been associated with decreased arterial calcium deposition and the ability to reverse vascular calcification in animal models. Vitamin K2 prevents pathological calcification in soft tissues via the carboxylation of protective MGP. The undercarboxylated (inactive) species of MGP is formed during inadequate Vitamin K status, or as a result of Vitamin K�
Vitamin K2 intake has been associated with decreased arterial calcium deposition and the ability to reverse vascular calcification in animal models. Vitamin K2 prevents pathological calcification in soft tissues via the carboxylation of protective MGP. The undercarboxylated (inactive) species of MGP is formed during inadequate Vitamin K status, or as a result of Vitamin K�

 adequate calcium intake without predisposing to CVD risk. Ingestion of micro- crystalline hydroxyapatite (the form of calcium found in bone) produces less of an acute spike in blood calcium levels compared to soluble calcium salts typically used in standard supplements, and thus may be less likely to increase vascular calcification and coronary risk.65 Hydroxyapatite also stimulates bone osteoblast cells and contains virtually all the essential building blocks needed to construct bone tissue. In a small placebo- controlled randomized trial, women who took 1000 mg of calcium in the form of hydroxyapatite in conjunction with oral Vitamin D showed a significant increase in bone thickness, whereas those who took 1000 mg of a standard calcium carbonate supplement did not (figure 4).70 Another double-blind placebo-controlled study found�
adequate calcium intake without predisposing to CVD risk. Ingestion of micro- crystalline hydroxyapatite (the form of calcium found in bone) produces less of an acute spike in blood calcium levels compared to soluble calcium salts typically used in standard supplements, and thus may be less likely to increase vascular calcification and coronary risk.65 Hydroxyapatite also stimulates bone osteoblast cells and contains virtually all the essential building blocks needed to construct bone tissue. In a small placebo- controlled randomized trial, women who took 1000 mg of calcium in the form of hydroxyapatite in conjunction with oral Vitamin D showed a significant increase in bone thickness, whereas those who took 1000 mg of a standard calcium carbonate supplement did not (figure 4).70 Another double-blind placebo-controlled study found�





